By Gina Shaw
Empiric antibiotic coverage for methicillin-resistant Staphylococcus aureus (MRSA) and Pseudomonas aeruginosa in patients with diabetic foot infections (DFI) did not correlate with risk factors for these organisms, according to data presented at the ASHP Midyear 2024 Clinical Meeting & Exhibition, in New Orleans (poster 8-041).
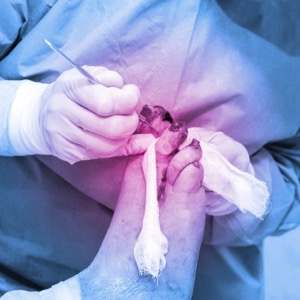
Broad-spectrum antibiotics are often used empirically for diabetic foot. “For example, vancomycin is occasionally added to regimens without regard to patient-specific risk factors,” said study author Kelsie-Ann Mita, PharmD, a pharmacist at Mount Sinai Chicago Hospital, an urban safety net community teaching hospital. “The duration of therapy of antibiotics may vary significantly based on patient-specific factors and physician preferences.”
In a retrospective review of electronic health records (EHRs), Dr. Mita and colleagues reviewed key data on 100 adult, nonpregnant patients treated for foot infections with or without osteomyelitis (OM) at Mount Sinai Chicago between 2019 and 2023. Of the patients, 24 were excluded as non-diabetic, for a total of 76 DFI included in the study. Most (54%) were classified as moderate infections with OM; 19% were moderate without OM, 17% severe with OM, 9% severe without OM and 1% as mild.
Sixty-nine patients received empiric antibiotic coverage for MRSA and 60 received empiric coverage for P. aeruginosa while only 21 and 19, respectively, presented with risk factors for those organisms. Ultimately, only 15 patients had positive culture results for MRSA and four for Pseudomonas. “Our hospital uses a vancomycin−cefepime regimen for empiric coverage of patients considered at risk for those organisms, and this study definitely shows that we have an extensive amount of patients with diabetic foot infections who are being over-covered with vancomycin and cefepime,” Dr. Mita said.
The study also found that patient hemoglobin A1c levels did not correlate with duration of therapy, and that inflammatory biomarkers, including the mean erythrocyte sedimentation rate (ESR) and mean C-reactive protein, had no strong correlations with the severity of DFI or OM. The mean ESR was 56.8 mm per hour in the moderate group, 55.2 in moderate with OM, 55 in the severe group and 54.4 in the severe with OM group. The mean C-reactive protein level was 57.1, 54.6, 75.9 and 59.2 mg/dL, respectively.
“Multiple comorbidities were common in these patients, including hypertension, renal disease, peripheral arterial disease, prior amputations and smoking, which complicated the assessment of underlying causes of infection,” Dr. Mita noted. “Going forward, we plan to educate the staff in a multidisciplinary approach involving emergency physicians, surgery, podiatry and pharmacy on how to appropriately treat patients with diabetic foot infections, focusing on optimizing the use of broad-spectrum antibiotics by patient risk factors and de-escalating to target therapies by culture and susceptibilities. We would also like to plan a larger study that would allow for the characterization of site organisms.”
Dr. Mita reported no relevant financial disclosures.