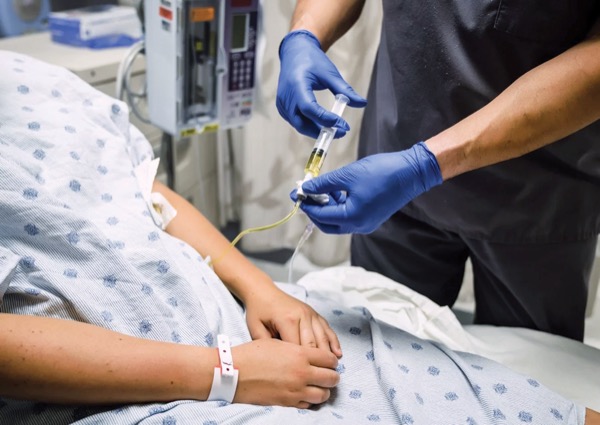
When acute bacterial skin and skin structure infections (ABSSSIs) are not cured by oral antibiotics, many health systems opt for inpatient treatment with IV generics. However, these infections treated in the emergency department (ED) with dalbavancin (Dalvance, AbbVie), an antibiotic requiring a single 30-minute infusion, can offer clinically similar and cost-effective results compared with hospital admission.
“Being able to take patients who are often only admitted for intravenous antibiotics and shift care to the outpatient [setting] benefits all [stakeholders in a health system],” explained study author Bruce M. Jones, PharmD, an infectious diseases clinical pharmacy specialist at St. Joseph’s/Candler Health System, in Savannah, Ga., who presented the study at IDWeek 2024, in Los Angeles.
The retrospective study followed the outcomes of a new protocol for treating ABSSSIs. Pharmacists and ED staff identified patients who would be appropriate for treatment in the ED instead of hospital admission.
Fifty-seven patients (average age 56.85 years; 30% female) were discharged from the ED after receiving a 1,500-mg infusion of dalbavancin. Patients suffered from various conditions including abscesses, cellulitis and postoperative wounds. Most of the cohort met multiple diagnostic criteria for treatment with dalbavancin, including more than three-fourths of patients reporting erythema, tenderness or swelling. Patients with an anticipated need of less than 14 days of antibiotics for their ABSSSI, osteomyelitis, necrotizing fasciitis, gangrene or diabetic foot ulcer were excluded.
The patients often faced financial barriers to care and difficulty adhering to medication regimens. Only six patients (10.5%) were admitted to the hospital within 30 days of dalbavancin administration. This was similar to the national average outcomes for inpatient ABSSSI treatment cited by the investigators.
Each ED visit included a roughly $3,800 average reimbursement per patient receiving dalbavancin. “This was a process that did not lose money for the health system overall,” Dr. Jones said. This is in contrast to inpatient stays where reimbursements for drugs and care may not cover the incurred costs. However, a limitation of the study was that there was no head-to-head comparison between the outpatient and inpatient therapies.
Despite the lack of comparative data, Kyle C. Molina, PharmD, of the Division of Infectious Diseases at University of Colorado Anschutz Medical Campus School of Medicine, in Aurora, who was not associated with the study, found the results intriguing. He noted that the results demonstrated the possibility of setting up a dalbavancin protocol in a larger community health system. “This is especially important for patient populations who are not good candidates for alternative therapies like oral antibiotics or admission for IV antibiotics, like patients who inject drugs and other vulnerable populations,” Dr. Molina said.
Both clinicians emphasized there are hurdles to implementing this protocol. Dr. Jones highlighted that clinical staff needs to be taught to select the correct patient, making sure that those with sepsis or unstable comorbidities are admitted to the hospital. However, even when staff is trained appropriately, implementation of the protocol is limited by a hospital administrator’s incentive structure.
Dr. Jones reported a consultantship with and being part of the speakers bureau for AbbVie. Dr. Molina consulted for Melinta and received free study drug from AbbVie.
This article is from the December 2024 print issue.