By Marie Rosenthal, MS
A higher clinical cure rate was found among patients with serious gram-negative bacterial infections who received cefiderocol (Fetroja, Shionogi) as empiric therapy or for a documented infection than among those given it as salvage therapy, according to a presentation at ESCMID Global 2025, in Vienna (poster P2542).
This is the largest real-world study of the effectiveness of the innovative siderophore cephalosporin, also known as Fetcroja outside the United States, according to a company release. The PROVE (Retrospective Cefiderocol Chart Review) study was a five-year, international, retrospective, observational medical chart review study, conducted between November 2020 and July 2024. The study described the efficacy and safety of cefiderocol use in adults with serious gram-negative bacterial infections.
The analysis presented at ESCMID reviewed data from 567 adults between 40 and 71 years of age, who were hospitalized with confirmed gram-negative bacterial infections, and received cefiderocol for the first time for at least 72 hours. The patients were from Spain, France, Italy, Germany and the United Kingdom. The researchers assessed baseline demographics, clinical characteristics, cefiderocol use, clinical cure and all-cause mortality (ACM).
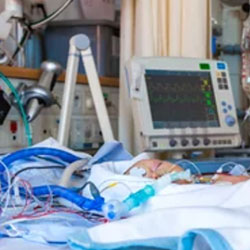
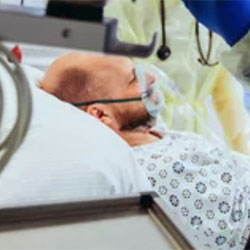
Almost 56% of patients were critically ill and treated in the ICU, and 41.3% were receiving organ support when cefiderocol was initiated. The carbapenem resistance rate was more than 70% among patients enrolled in the study. Many of the patients had comorbidities, including diabetes (24.7%), COVID-19 (20.3%) and chronic pulmonary disease (16.2%). More than 50% of the patients (n=299) had a respiratory tract infection, and 12% (n=73) had a urinary tract infection, which was the second most frequently reported site of infection.
For all pathogens, patients receiving cefiderocol achieved an overall clinical cure rate of 65.3%. The most frequently observed pathogens were Pseudomonas aeruginosa (41.3%), Acinetobacter baumannii (15.0%) and Enterobacterales (14.6%). The researchers found similar results among patients with bloodstream infection (60.7%), skin and skin structure infection (63.9%), and intraabdominal infection (64.7%).
Analysis of the European cohort found a higher clinical cure rate trend among patients who received cefiderocol for a documented infection (67.4%) or as empiric therapy (64.6%) compared with those given it as salvage therapy (58.2%).
“Among patients with P. aeruginosa infection, 73.1% achieved clinical cure and 19.7% died by day 30. Clinical cure and 30-day ACM rates were 50.6% and 35.3%, respectively, among patients with A. baumannii infection, and 63.9% and 25.3%, respectively, among patients with Enterobacterales infection,” the researchers reported in the poster.
“These data suggest a trend toward worse clinical outcomes when the use of cefiderocol to treat gram-negative bacterial infections is reserved as a last-line treatment option compared with those who received the treatment earlier. This trend may offer clinicians new evidence to justify the early and effective use of cefiderocol in patients with suspected resistant infections,” said Oliver Cornely, Prof Dr Med, the director of Translational Research, University of Cologne, in Germany, in a company statement. Dr. Cornely is also the scientific director of the Center for Clinical Trials, and he serves as an infectious diseases consultant at the University Hospital of Cologne.
The researchers reported financial relationships with Shionogi.