By IDSE News Staff
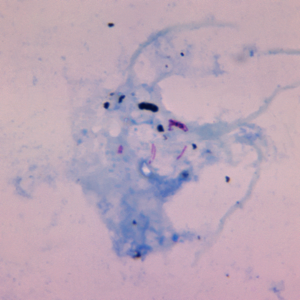
Although tuberculosis is the leading cause of death from infectious disease in the world, it’s estimated that those deaths represent perhaps 5% of infections with Mycobacterium tuberculosis. A growing body of evidence suggests genetic vulnerabilities to TB account for the severity of disease in some patients.
Researchers from The Rockefeller University, in New York City, have found a rare mutation that leaves its carriers much more likely to become ill with TB—but, curiously, not with other infectious diseases. This finding may upend long-held assumptions about the immune system, they said (Nature 2024 Aug 28. https://doi.org/10.1038/s41586-024-07866-3).
An acquired deficiency of the pro-inflammatory cytokine, tumor necrosis factor (TNF) is linked to an increased risk of developing TB. The current study, led by Rockefeller’s Stéphanie Boisson-Dupuis, PhD, and Jean-Laurent Casanova, MD, PhD, showed a genetic cause of TNF deficiency, as well as the underlying mechanism: A lack of TNF incapacitates a specific immune process in the lungs, leading to severe, but surprisingly targeted, illness.
The findings suggest that TNF, long considered a key galvanizer of the immune response, might play a much narrower role—a discovery with far-reaching clinical implications, they said.
“The past 40 years of scientific literature have attributed a wide variety of pro-inflammatory functions to TNF,” said Dr. Casanova, the head of the St. Giles Laboratory of Human Genetics of Infectious Diseases. “But beyond protecting the lungs against TB, it may have a limited role in inflammation and immunity.”
Dr. Casanova’s lab has been studying the genetic causes of TB for more than two decades. They maintain an ever-growing database of whole-exome sequences from a global pool of patients—more than 25,000 people to date. Of those, some 2,000 have had TB.
Over the years, they’ve identified several rare genetic mutations that render some people more vulnerable to TB. For example, mutations in the CYBB gene can disable an immune mechanism called the respiratory burst, which produces reactive oxygen species (ROS), which help phagocytes destroy the invaders they’ve devoured. If ROS aren’t produced, those pathogens can thrive unchecked, leading to debilitating complications. As a result, carriers of this CYBB mutation become vulnerable to not just TB but to a variety of infectious diseases.
For the current study, the team suspected that a similar mutation may exist behind the severe recurrent TB infections experienced by two people in Colombia—a 28-year-old woman and her 32-year-old cousin—who had been repeatedly hospitalized with significant lung conditions. In each cycle, they initially responded well to anti-TB antibiotics, but within a year, they were sick again.
However, it’s puzzling that their long-term health records showed their immune systems functioned normally, and they were otherwise healthy.
To find out why they were particularly prone to recurrent infections of TB, the researchers performed whole-exome sequencing on the two, as well as a genetic analysis of their respective parents and relatives.
The two were the only members of their extended family with a mutation in the TNF gene, which encodes for proteins linked to the regulation of a variety of biological processes. TNF production is also associated with a variety of conditions, including septic shock, cancer, rheumatoid arthritis and cachexia, which causes dangerous weight loss.
The protein is largely secreted by macrophages, which rely on the ROS molecules generated by the respiratory burst to finish off pathogens they’ve consumed.
In these two patients, the TNF gene failed to function, preventing the respiratory burst from occurring, and thus the creation of ROS molecules. As a result, the patients’ alveolar macrophages, located in their lungs, were overrun with M. tuberculosis.
“We knew that the respiratory burst was important for protecting people against various types of mycobacteria, but now we know that TNF is actually regulating the process,” Dr. Boisson-Dupuis said. “And when it’s missing in alveolar macrophages, people will be susceptible to airborne TB.”
She added, “It’s very surprising that the people we studied are adults who have never been sick with other infectious diseases, despite being repeatedly exposed to their microbes. They are apparently selectively at risk for TB.”
The discovery also solves a long-standing mystery about why TNF inhibitors, which are used to treat autoimmune and inflammatory diseases, raise the chances of contracting TB. Without TNF, a key part of the defense against it is defunct. The findings may lead to a radical reassessment of TNF’s role in immune function—and new treatment possibilities.