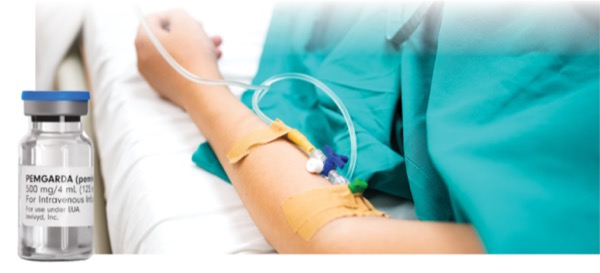
Follow-up data from a phase 3 clinical trial show that pemivibart (Pemgarda, Invivyd) offers long-term protection against COVID-19, according to a study presented at IDWeek 2024, in Los Angeles.
Pemivibart is an IV monoclonal antibody that was engineered from adintrevimab, another mAb developed by Invivyd. It targets the spike protein receptor-binding domain of SARS-CoV-2, preventing the virus from entering the human angiotensin-converting enzyme 2 receptor on host cells.
“When infused with pemivibart, our belief is you are packing a lot of protective punch,” aid Marc Elia, the chairman of the Board of Directors of Invivyd.
In March, the FDA granted emergency use authorization (EUA) to pemivibart to prevent COVID-19 in people 12 years of age and older weighing at least 88 pounds who are moderately to severely immunocompromised and might not mount an adequate immune response to vaccination. The EUA was based on the scientific evidence available, including data from the CANOPY phase 3 clinical trial that used immunobridging to compare the titer levels of pemivibart in the immunocompromised cohort with titer levels associated with efficacy in a prior clinical trial with adintrevimab. The results showed that the former’s outcomes were also consistent with other mAbs.
“This approach [immunobridging], borrowed from vaccine development, can provide clinicians and regulators alike with a useful framework for mAbs as we innovate toward rational, scalable, high efficacy medicines that can protect vulnerable populations against COVID-19,” said Mark Wingertzahn, PhD, the senior vice president of Clinical Development and Medical Affairs.
In six-month follow-up data, there were 19 COVID-19 cases in the placebo arm (n=160) compared with six in the pemivibart arm (n=317) among immunocompetent people, showing an overall relative risk reduction (RRR) in symptomatic disease of 84%. At 12 months, the RRR was 64% even though pemivibart has an estimated in vivo half-life of approximately 45 days.
“We showed over the period of which immunocompetent people were on the drug an 84% reduction in getting symptomatic COVID-19,” Dr. Elia said, which is longer than vaccination (bit.ly/4eVoKms-IDSE).
Last August, the Infectious Diseases Society of America (IDSA) released clinical guidance suggesting its use for immunocompromised patients. Adarsh Bhimraj, MD, FIDSA, the director of infectious diseases education and fellowship at Houston Methodist Hospital and the lead author of the guideline, said he is pleased to see these new data on pemivibart’s efficacy, “but it is not enough for us to change either the strength of the recommendation or the direction of the recommendation,” he said. Information about which immunodeficiencies would benefit most from pemivibart would be helpful.
However, he reiterated its benefit in patients at moderate to high risk for immunodeficiency, such as those with a hematologic malignancy and/or have received an organ transplant. “If I have a lung transplant patient on immunosuppressive therapy, where vaccine efficacy is likely to be suboptimal and the risk of COVID-19 exposure is high, I would consider prophylaxis with pemivibart,” Dr. Bhimraj said.
This article is from the December 2024 print issue.