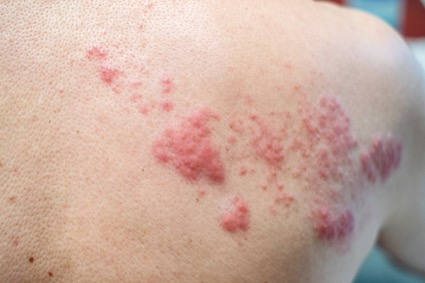
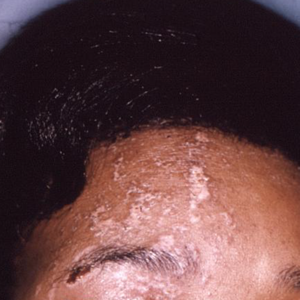
There is a significantly increased risk for developing herpes zoster, or shingles, in adults aged 50 years and older who have been diagnosed with COVID-19, according to a retrospective cohort study (Open Forum Infect Dis 2022;9[5]:ofac118).
“The COVID-19 pandemic exposed how vulnerable older adults are to infectious disease,” said lead author Amit Bhavsar, MBBS, MHA, a physician and the director of clinical research and development at GSK in Belgium.
“We wanted to expand research to further understand the impacts of the pandemic on adults aged 50 or older, which led to this first-of-its-kind observational study between COVID-19 and zoster,” he added.
The researchers performed a large retrospective cohort study to assess the risk for developing shingles after a COVID-19 diagnosis. They compared the incidence of shingles in people 50 years of age and older diagnosed with COVID-19 versus those without COVID-19. They used data from the MarketScan Commercial Claims and Encounters and Medicare Supplemental (March 2020 to February 2021) as well as the Optum Clinformatics Data Mart (March to December 2020) databases.
A Higher Risk Seen
According to the study, the researchers exact-matched individuals with COVID-19 1:4 to those without COVID-19 by age, sex, presence of risk factors for shingles and healthcare cost level. They estimated adjusted incidence rate ratios (aIRRs) by Poisson regression. They matched a total of 394,677 individuals 50 and older with COVID-19 to 1,577,346 without COVID-19. They balanced mean follow-up time after COVID-19 diagnosis and baseline characteristics between cohorts. Those diagnosed with COVID-19 had a 15% higher risk for developing shingles than those without COVID-19 (aIRR, 1.15; 95% CI, 1.07-1.24; P<0.001). The increased shingles risk was more pronounced (21%) following COVID-19 hospitalization (aIRR, 1.21; 95% CI, 1.03-1.41; P=0.02).
“Interestingly, the study showed that not only were people aged 50 or older who contracted COVID-19 15% more likely to develop shingles compared [with those who did not have COVID-19], but the risk of shingles was elevated for up to six months after a COVID-19 diagnosis,” Dr. Bhavsar said.
Prior to this study, a series of case reports and descriptive analyses showed a possible association between COVID-19 and shingles in older people during the first year of the pandemic (Dermatol Ther [Heidelb] 2021; 11:1119–26).
It was hypothesized that after initial infection with COVID-19, if sufficient levels of varicella-zoster virus (VZV)-specific T-cell immunity weren’t maintained and cell-mediated immunity declined, VZV reactivation leading to herpes zoster could be triggered (J Clin Virol 2010; 48:S2–7). (Older people, for example, could be more vulnerable due to immunosenescence or immunosuppressive conditions.) But until this study, the evidence wasn’t yet there.
Abinash Virk, MD, an infectious disease specialist at Mayo Clinic in Rochester, Minn., finds the outcome of this study unsurprising and yet also very interesting. “We do know that COVID-19 does likely cause short-term relative T-cell immunosuppression, which can then result in reactivation of some viral infection or other opportunistic infections,” she said, adding that “it’s important to realize that there are other vaccine-preventable diseases that can occur in these patients and alert primary care providers.”
Although the study design controlled for possible confounding, other factors may have affected the observed shingles risk, according to Dr. Bhavsar. For example, the analyzed databases contain no information on race and ethnicity. As COVID-19 has disproportionately affected the Black population, the COVID-19 cohort in this study may include proportionately more Black adults than the non–COVID-19 cohort. This may have led to an underestimation of the effect of COVID-19 on shingles, given that Black adults have a lower risk for shingles than those who are white.
Dr. Virk said she would have expected higher rates of herpes zoster in patients who receive tocilizumab (Actemra, Genentech) and other immunosuppressive regimens for the management of COVID-19, but the researchers did not identify this particular patient group separately.
“Therefore, it would be particularly helpful to look at patients who received immunosuppressive regimens for hospitalized COVID-19 infection,” she said. “Additionally, [it is] also important to look at older patients and those with immunosuppression.” Dr. Virk said she would like to know whether the shingles vaccine is still protective in these patients.
According to Dr. Bhavsar, an Avalere Health report showed that cumulatively, from January 2020 to July 2021, adults and teens may have missed an estimated 37.1 million doses of recommended vaccines compared with 2019 (https://avalere.com/insights).
“It is critical that we, as infectious disease specialists, work to educate and vaccinate patients with all the recommended vaccines,” Dr. Bhavsar said, “so that the COVID-19 pandemic does not continue to impact routine preventative care.”
Drs. Bhavsar and Virk reported no relevant financial disclosures outside of their employment.
This article is from the June 2022 print issue.