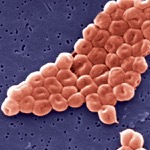
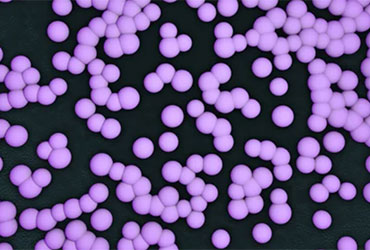
Mupirocin-resistant strains of Staphylococcus aureus may be more common in healthcare settings than appreciated.
“This is a cautionary tale,” said Austin Terlecky, BS, a research technician in infectious disease at Hackensack Meridian Health’s Center for Discovery and Innovation, in Nutley, N.J. Hospital leaders may wish to proactively look for mupirocin-resistant S. aureus, Mr. Terlecky added, before using mupirocin in decolonization efforts. He added that antimicrobial resistance testing may not be common for topical agents, and that mupirocin resistance surveillance is not routine.
“There are protocols in place to give mupirocin prophylactically,” Mr. Terlecky noted. At Hackensack Meridian and other health systems, it’s often given topically. This research suggests mupirocin will be less effective than hoped.
Resistance in 35% of Isolates
Mr. Terlecky and colleagues evaluated 5,663 nasal swabs collected over seven months at a New Jersey hospital, collected during intensive care, neonatal intensive care and transplant center admissions. Among these nasal swabs, there were 1,390 S. aureus isolates, along with 134 bloodstream S. aureus isolates.
Using polymerase chain reaction (PCR) technology, researchers identified which of the S. aureus isolates contained mupA, the gene responsible for high-level mupirocin resistance. They found mupA in 35% of all isolates, more than reported in previous literature (J Hosp Infect 2013;85[4]:249-256).
This proportion rose to 48% in mupirocin-resistant S. aureus strains.
The PCR testing for mupirocin resistance only took about two hours to identify presence of mupA, Mr. Terlecky noted, so in theory, it could become part of routine surveillance efforts. That process would also involve sample collecting, identification, transportation and purification.
“Maybe this is something that could be easily implemented,” Mr. Terlecky said.
What to Do About Mupirocin Resistance
Even if a health system identified concerning levels of mupirocin-resistant S. aureus, it’s unclear how to respond to that fact. During Mr. Terlecky’s presentation, audience members pointed out that mupirocin is a prime tool against S. aureus even if it is less effective than desired.
“This is a good study for putting mupirocin resistance onto people’s radar which is something I do not think many practitioners think about. We don’t typically screen for mupirocin resistance in the clinical realm,” said Taylor Morrisette, PharmD, MPH, an associate professor and infectious disease pharmacist at the Medical University of South Carolina, in Charleston.
Sometimes mupirocin resistance rates approach the 35% found in this study, Dr. Morrisette said, based on a scan he did of the literature. But many other reports have found that they are typically much lower.
“Overall, we know there’s drastic variation in resistance rates dependent on geographical location,” said Dr. Morrisette, who is also an Infectious Disease Special Edition editorial advisory board member. He said these varied rates point to the need for local surveillance that can guide local decolonization efforts.
Dr. Morrisette said it would be interesting to perform exploratory analyses to evaluate if S. aureus mupirocin resistance rates are higher in the transplant ward or intensive care unit than elsewhere, and thus driving the overall resistance trends. Resistance in the neonatal ward is less likely to be driving overall trends, Dr. Morrisette said, given that neonates typically have had less antibiotic exposure in their shorter lives.
It would also be good to compare mupirocin resistance rates in these high acuity areas of the hospital with those of patients in the general medical ward, Dr. Morrisette added.
Dr. Morrisette reported that he is currently receiving grant funding through AbbVie and Stellus Rx; has participated in scientific advisory boards for AbbVie and Shionogi; has provided expert witness testimony to Copeland, Stair, Valz & Lovell as well as Huff, Powell & Bailey; and has received honoraria from Infectious Disease Special Edition, Managed Healthcare Executive and Shionogi. Mr. Terlecky, who presented his research at ASM Microbe 2025, reported no relevant financial disclosures.