Chikungunya cases are increasing around the world due to a number of factors, including climate change, increased travel and urbanization, according to WHO, which issued a public health advisory earlier this year.
By July 2025, approximately 240,000 chikungunya virus disease (CHIKVD) cases and 90 CHIKVD-related deaths had been reported in 16 countries and territories, according to the European Centre for Disease Prevention and Control (ECDC), with the Americas, Africa, Asia and Europe all reporting cases. This includes a large outbreak on RÉunion island, which had not seen a case since 2014.
“Chikungunya is not a disease that is widely known, but it has been detected and transmitted in 119 countries globally, putting 5.6 billion people at risk,” said WHO’s Diana Rojas Alvarez, MD, PhD, the medical officer and team lead for arboviruses, in Geneva. Dr. Alvarez presented data at an EPI-WIN—an epidemic information network—webinar about chikungunya sponsored by the WHO in May 2025 (youtube.com/watch?v=ot_v2gqz51A).
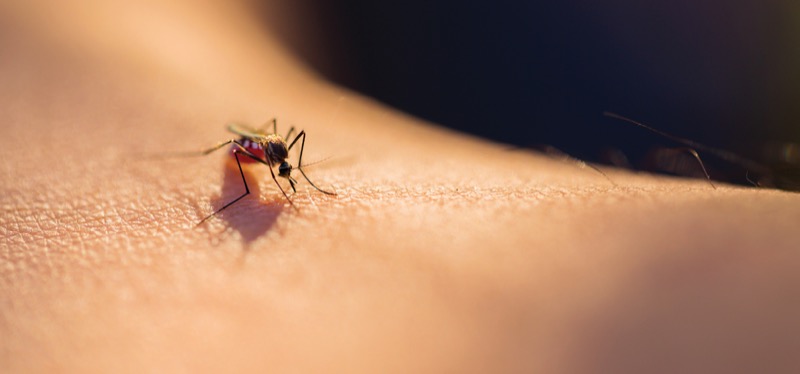
Once limited to tropical and subtropical climates, the Aedes mosquito that transmits chikungunya, as well as dengue, yellow fever and Zika virus, “is spreading to new regions due to climate change, population growth, and increased travel and urbanization, increasing the risks for outbreaks,” Dr. Alvarez said. As late as September, Italy and France were still reporting cases, according to the ECDC.
More than 50% of patients with CHIKVD will experience symptoms such as fever and severe, sometimes incapacitating arthralgia. In fact, the severe pain gives chikungunya its name, according to Dr. Alvarez. The word chikungunya comes from the Kimakonde language of Tanzania, where it was first identified in 1952, which means “man who can’t bend over.”
The pain and symptoms can last up to three months. If the symptoms continue, it’s characterized as chronic disease. “About 40% to 50% of the people with acute disease can progress to chronic disease that can last for years,” Dr. Alvarez said.
For those who develop chronic CHIKVD, “the really excruciating pain and arthritis that characterizes the disease can last for months or even years. And that pain can have a big impact on their quality of life, their ability to work and to perform daily tasks,” said Ben Simone, MD, MPH, the global medical affairs director of travel vaccines at Bavarian Nordic, which makes the recombinant chikungunya vaccine, Vimkunya. (Dr. Simone was not a presenter at the webinar but was asked to discuss the disease.)
Disease onset is typically four to eight days but can appear as soon as two days or as late as 12 days after exposure. Although infrequent, some patients, particularly those with comorbidities, can develop severe chikungunya with cardiovascular disease (CVD) and neurologic and multi-organ involvement, which may result in hospital admission, intensive care and death.
Vulnerable populations at high risk include older adults and neonates infected through vertical transmission or after birth through infected mosquito bites. “The occurrence of severe disease in patients over 65 and in newborns infected during birth or soon afterward highlights concerns about the impact of the disease on vulnerable populations,” said Maria Van Kerkhove, PhD, MS, the director of the Department of Epidemic and Pandemic Threat Management at WHO, during the webinar.
Comorbidities increase the risk for severe or chronic disease, Dr. Simone told Infectious Disease Special Edition. “For example, people with diabetes, obesity [and] cardiovascular disease are at increased risk, and people with rheumatological disease—for them, chikungunya can make their condition worse.
“But even healthy people can develop severe chikungunya,” he said.
Challenging Diagnosis
Diagnosing CHIKVD can be challenging because the symptoms overlap with other febrile illnesses, according to Dr. Simone. In addition, in some regions, multiple arboviruses may circulate simultaneously. As outbreaks increase and spread to new regions, it is imperative for healthcare professionals to recognize this threat and keep it in their differential, especially if the patient has traveled to an endemic area.
“It’s impossible to diagnose chikungunya unless you are specifically looking for it,” Dr. Simone said. “So, if you have a patient who has just returned from travel to an at-risk area who has fever, who has pains, you should really ask for a diagnostic laboratory confirmation test. This would be an RT-PCR [reverse transcriptase–polymerase chain reaction] if it’s a recent infection or serology if it is a few days old.
“What’s really important is when you have a patient who has a positive travel history, with compatible symptomatology, you should keep chikungunya in the back of your mind and get laboratory confirmation,” he said. This improves surveillance not only in the United States but low-resource nations because they might not have the infrastructure to track and report cases, although WHO is helping to improve surveillance throughout the world.
“Diagnoses of chikungunya in returning travelers by an American Doctor essentially serve as sentinel events,” Dr. Simone explained.
Treatment for CHIKVD entails symptom management, so prevention is key. The mosquito is a day-biting insect, not one that bites at dusk or night, so countermeasures such as bed nets are not useful. However, wearing long-sleeved shirts, long pants tucked under socks, using insect repellents that contain DEET and removing standing water, which are mosquito breeding sites around the home, can be helpful. But vaccination is the most important and effective prophylaxis.
Until July, there were two vaccines available in the United States: a live-attenuated vaccine (Ixchiq, Valneva) that was indicated for those 18 years of age and older, and a virus-like particle vaccine (Vimkunya, Bavarian Nordic) approved for people 12 and older.
When IDSE went to press, Ixchiq, which was approved in 2023 with a warning the vaccine could cause severe or prolonged chikungunya-like adverse reactions, was no longer licensed in the United States. In May, the FDA issued a safety communication and paused the use of Ixchiq because of post-marketing reports of serious adverse events, including neurologic and cardiac events after vaccination. On Aug. 6, the FDA lifted the pause in people 60 years of age and older after investigating those reports. Then on Aug. 22, the FDA’s Center for Biologics Evaluation and Research suspended the license for Ixchiq due to “serious safety concerns” reported on the Vaccine Adverse Event Reporting System, a passive surveillance system. The vaccine is still available outside the United States.
There have been no health authority investigations of Vimkunya, which remains approved for use in the United States. Vimkunya, a virus-like particle vaccine, which mimics the chikungunya virus to induce an immune response, was approved in February 2025, based on the results from two phase 3 clinical trials that enrolled more than 3,500 healthy people 12 years of age and older. The vaccine induced neutralizing antibodies in up to 97.8% of vaccinated people at 21 days after vaccination. In addition, a rapid immune response developed within one week of vaccination, according to the vaccine’s prescribing information.
Since these vaccines are new, post-marketing research is necessary, especially in the context of outbreaks, according to Phil Kraus, MD, an advisor to the WHO R&D Blueprint for Epidemics, whose goal is to maximize research efforts to inform response and prevention strategies for outbreaks and pandemics. “Research priorities for vaccine evaluation in the context of an outbreak need to emphasize speed and transparency, as well as having the tools and core protocols available at the beginning of the outbreak,” Dr. Kraus said. The vaccine developers said they were working on developing protocols.
The recent outbreaks on the islands of Mauritius and RÉunion “are going to provide critical information about what it takes to prevent [and] protect populations and communities against this disease,” Dr. Kraus said.
Mosquito control with insecticides is going to be the most important means for controlling outbreaks, at least for now, he added.
“Our ultimate goal is to reduce morbidity and mortality due to chikungunya and other arboviral diseases by moving from the posture of reactive outbreak response to that of building preventative capacities during and after outbreak periods to better mitigates the impacts of moving forward,” Dr. Van Kerkhove said.
The sources reported no relevant financial disclosures beyond their employment.
This article is from the October 2025 print issue.