The changing environment—urbanization, industrialization and climate change—is leading to the spread of Coccidioides. Until recently, the fungus that causes Valley fever lived mostly in the southwestern United States, but today clinicians throughout the country should keep an open mind about this condition (JAMA Insights 2025 Feb 20. doi:10.1001/jama.2024.27274).
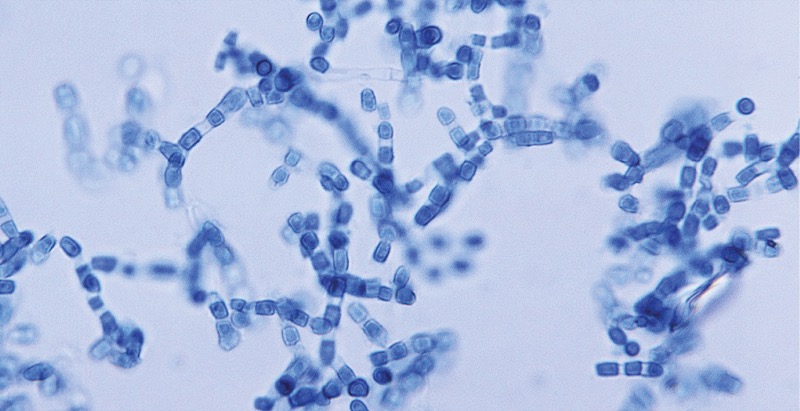
“Valley fever is caused by Coccidioides, a fungus that prefers dry areas,” said Pamela S. Lee, MS, MD, of the Division of Infectious Diseases at Harbor-UCLA Medical Center, in Torrance, Calif. “Valley fever refers to the San Joaquin Valley [in California], but also has ‘hot spots’ in Arizona and Texas.”
Coccidioides resides in soil, and its growth is thought to increase with heavy precipitation. In their paper, Dr. Lee and her colleagues discussed how several years of drought followed by the very wet storms in California in 2022-2023 led to “record-high numbers of coccidioidomycosis in 2023.”
Effect of Climate Change
“Climate change has already increased temperatures and evaporative demand (i.e., the propensity of air to drive evaporation from the land surface and bodies of water) in the U.S. These changes have increased drought severity and soil dryness in the American West, with further increases anticipated depending on future global warming trajectory,” Dr. Lee and her team wrote. “Decreases in soil moisture and/or increasingly wide or frequent swings between dry and wet conditions may promote environmental settings increasingly favorable to Coccidioides growth and dispersion.”
Coccidioidomycosis occurs with inhalation of spores that emerge from the soil when areas dry out, explained John Galgiani, MD, a professor of medicine in infectious diseases at the University of Arizona College of Medicine–Tucson.
“Many people do not know they are infected and become immune without clinical illness that requires any medical attention,” Dr. Galgiani said. “These people are asymptomatic or have mild symptoms.”
Other people may develop more severe infections with symptoms that can include respiratory issues, joint aches or fatigue that can last weeks or months, he said.
“A small percentage of people—probably about one out of 200—will go on to have progressive infection where the fungus goes from the bloodstream to other parts of the body like the brain or the bone, which can be very problematic,” Dr. Galgiani said. “If a patient develops Valley fever meningitis, that can be fatal.”
Increased Awareness
Dr. Lee and her colleagues published their paper in part, she said, to try to increase awareness of Valley fever, which “tends to be very underdiagnosed, with patients sometimes going to urgent care or the emergency department multiple times with complaints without ever getting tested for this fungal infection,” she said. “If climate change modeling pans out, and Coccidioides becomes endemic in places it currently isn’t, that will widen the underdiagnosis gap.”
Underdiagnosis exists even in places where Coccidioides is more common. As an example, Dr. Galgiani recently saw a patient diagnosed with Valley fever who had been experiencing symptoms since spring 2024.
“He has half a dozen lesions in his bones that have destroyed his vertebral column, and he went undiagnosed for nine months,” Dr. Galgiani said.
It is important for clinicians to ask if patients have traveled to places where Valley fever is endemic, Dr. Lee said. Testing for the infection with a blood test is simple and inexpensive.
Within his health system’s urgent care clinics, Dr. Galgiani said education has increased the rates of testing for Valley fever in people with pneumonia symptoms from 2% in 2020 to 40% in 2024. He was also involved in the research that led to the discovery of a vaccine against Valley fever, which is being developed by Anivive Life Sciences and is proceeding toward a first-in-human clinical trial.
“I would encourage people to keep an open mind about where coccidioidomycosis can occur,” Dr. Lee said. “Those geographic boundaries often taught in medical school are not the be-all [and] end-all.”
Drs. Galgiani and Lee reported no relevant financial disclosures.
This article is from the October 2025 print issue.