Fungi seen in medical tourists in Mexico and people visiting bat-inhabited caves, as well as a new species transmitted from cats to humans, were among the top outbreaks investigated recently by the CDC. Experts spoke about the updates during a presentation at IDWeek 2025, in Atlanta.
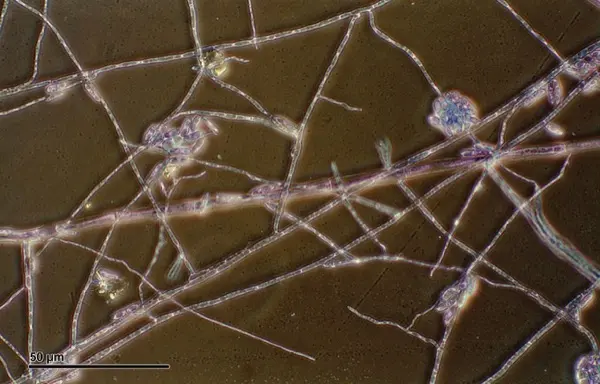
Fusarium solani
In May 2023, the CDC received an email about two unusual cases of meningitis of unknown etiology, in which both patients had epidural anesthesia during cosmetic procedures in Matamoros, Mexico, said Dallas Smith, PharmD, MAS, an epidemiologist with the CDC’s Mycotic Diseases Branch, at IDWeek. Several other cases were reported soon after, affiliated with two clinics in Matamoros. Other than a positive beta-D-glucan test, tests were negative.
That month, Mexican authorities used polymerase chain reaction (PCR) testing to confirm the Fusarium solani species complex. Simultaneously, in the United States, Dr. Smith and colleagues searched for ways to identify etiology, finding just one U.S. laboratory with a pan-fungal PCR test and one with a metagenomics test approved by Clinical Laboratory Improvement Amendments (CLIA) that identified F. solani. The labs later confirmed the results through cultures from two patients.
CDC investigators obtained a list of 230 patients potentially exposed at the clinics and were able to contact 170 of them for potential testing, Dr. Smith said. Of those contacted, 104 had received epidurals and 53 had symptoms. Twenty-four were found to have confirmed or probable fungal meningitis, and 12 died (Clin Infect Dis 2025 July 22. doi:10.1093/cid/ciaf399).
The CDC’s investigations linked all 24 cases to the same anesthesiologist who brought their own medication to mix morphine with bupivacaine for epidurals, Dr. Smith said. Incubation periods ranged from 0 to 58 days from the procedure to the onset of symptoms, he said, and time from procedure to hospitalization ranged from 14 to 106 days. “If someone has been exposed to fusarium for over 100 days, that is a very difficult infection to treat,” he said.
CDC mycologists initially developed recommendations for treatment with intravenous voriconazole and liposomal amphotericin B, he said. But when antifungal susceptibility testing became available that July, they suggested that manogepix (prodrug fosmanogepix) would have the best minimum inhibitory concentration. Through a compassionate use program, they were able to get the phase 3 drug to patients who survived to that point. The case-mortality rate was 14% among patients taking fosmanogepix compared with 65% among those who didn’t.
Investigators are still monitoring for additional cases of fungal meningitis linked to medical tourism, Dr. Smith said. The case highlights the need for better access to CLIA-approved fungal diagnostics to facilitate identification of causative organisms, he said.
Other Investigations
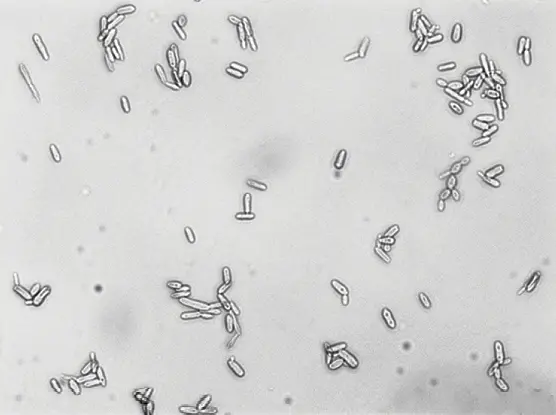
Rates of the mold Purpureocillium lilacinum are increasing, from 56.6 in 100,000 fungal cultures in 2019 to 74.3 in 2024, Dr. Smith said. A cluster of P. lilacinum was found among three patients following LASIK surgery in New York City, resulting in severe disease (one needing a corneal transplant). A pseudo-outbreak was seen among 22 patients with positive skin specimens collected using contaminated saline.
The CDC has reviewed three outbreaks in the last year of U.S. and Canadian travelers returning home from Costa Rica (MMWR Morb Mortal Wkly Rep 2025 74[17]:289-292), Mexico (Can Commun Dis Rep 2025;51[5]:187-190), and Belize with histoplasmosis. Each outbreak involved families who toured bat-inhabited caves or flooded caves in these countries, with 18 of 19 (95%) exposed travelers becoming ill, Dr. Smith said. Eight (67%) were initially misdiagnosed or prescribed antibiotics inappropriately, he noted.
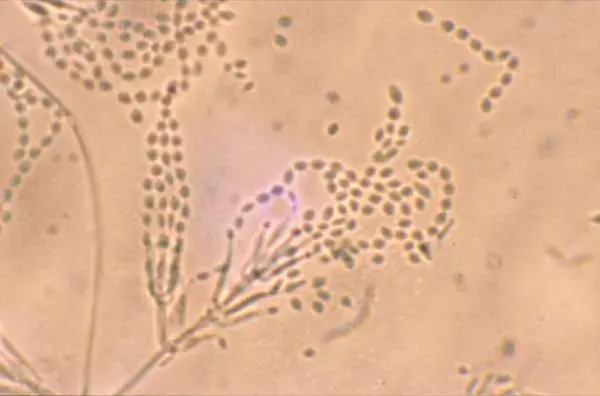
Sporothrix brasiliensis
Zoonotic sporotrichosis, mainly transmitted from cats to humans, continues to spread in Latin America and beyond, with a new more virulent species, Sporothrix brasiliensis, requiring three to six months of treatment. It can spread through scratches or sneezes, Dr. Smith said, and can survive on metal surfaces for up to three months. “This is a really huge concern, not only in South America but also in really any country that might import these cats,” he said.
Teamwork Is ‘Lifesaving’
The session showed how much we have learned in fighting these infections, according to Cesar Berto, MD, an assistant professor of medicine and infectious diseases at the University of Alabama at Birmingham, who co-moderated the session. “There is a lot we have learned from the outbreaks that we have had within the United States in terms of fungal infections,” Dr. Berto told Infectious Disease Special Edition. Dr. Smith highlighted the importance of working quickly with the CDC to develop CLIA-approved fungal testing for the fungal meningitis cases, Dr. Berto said, and working along with pharmaceutical companies to obtain expanded release for medications that were not yet approved for these patients “was essentially lifesaving.”
The Importance of Therapeutic Drug Monitoring
The session also addressed the role of azole therapeutic drug monitoring (TDM)—measuring specific drug concentrations in the blood or other fluids at designated time points to ensure appropriate levels are achieved/maintained—in treating invasive fungal infections. The practice helps prevent adverse events and toxicity and mitigate drug–drug interactions, said Mirando So, PharmD, MPH, the manager of the antimicrobial stewardship program at University Health Network, in Mississauga, Ontario.
TDM is recommended as routine for voriconazole and should be considered for specific patients for itraconazole (e.g., pediatrics, critically ill patients, or those on long-term courses) and posaconazole (e.g., patients with absorption concerns, risk for toxicity, or UGT1A4 polymorphism), she said. It is not routinely recommended for fluconazole and isavuconazole but can be considered in pediatric and some other populations.
The speakers reported no relevant financial disclosures.
This article is from the February 2026 print issue.