As the risk for drug-resistant fungal infections rises, healthcare professionals should be aware of how these infections are likely to present in people with HIV, according to a review published by researchers in Brazil (mBio 2025 Apr 2. doi:10.1128/mbio.00562-25).
Both candidiasis and fungal meningitis cases appear to be rising in people with HIV, but Aspergillus cases do not, the review found. However, having HIV appears to increase the severity of infections with Aspergillus spp., which are more likely to be drug resistant.
The review points out that factors, such as tuberculosis, COVID-19, influenza and Pseudomonas aeruginosa infection, also may play an important role in fungal coinfections for people with HIV.
“HIV infection is not necessarily the only predisposing factor for fungal infections,” said Daniel A. Santos, PhD, a professor of microbiology at the Universidade Federal de Minas Gerais, in Brazil, who led the review.
ART Makes the Biggest Difference
At the end of 2023, nearly 80% of people around the world living with HIV had access to antiretroviral therapy (ART), Department of Health & Human Services data show (hiv.gov/hiv-basics/overview/data-and-trends/global-statistics).
“Antiretroviral therapy changes everything,” said Arturo Casadevall, MD, a microbiologist and the chair of molecular microbiology and immunology at the Johns Hopkins Bloomberg School of Public Health, in Baltimore. “Individuals with well-controlled HIV have almost the same risk of getting a fungal infection as people who are not immunocompromised.”
The review included a French study, published in 2002, that indicated a mortality rate of 68% for invasive aspergillosis in people with HIV who were not taking ART (J Hosp Infect 2002;51[4]:288-296).
That rate dropped to 31% for people who were taking ART in addition to antifungal drugs.
Widespread use of ART has decreased opportunistic fungal infections, such as thrush, in people who have HIV. However, the review noted that other immunocompromising factors could linger in people with well-controlled HIV.
The review indicated that invasive aspergillosis and obstructive bronchial forms of the fungal infection were the most common among people living with HIV. However, these infections are still uncommon among people with HIV compared with those who are immunocompromised for other reasons, such as having TB, COVID-19 or influenza.
The review found that when they do occur, Aspergillus coinfections appear more commonly in people with HIV who have also depleted neutrophils and macrophages.
However, the review found that HIV appears to promote changes in the native commensal fungal microbiota, which can make people more susceptible to endogenous coinfections, such as candidiasis. These infections more commonly targeted the kidneys, but it’s unclear why.
“It could be a consequence of blood filtration, poor neutrophil recruitment, or there could be some metabolite or nutrient in the kidneys that favors Candida proliferation,” Dr. Santos said.
Uncertain Future
Decreased funding for organizations that prescribe HIV drugs in places such as sub-Saharan Africa, growing drug resistance, and climate change are creating a precarious situation for fungal infections, not just for people with HIV.
“Cryptococcosis remains a huge problem in Africa,” Dr. Casadevall said. “One of the concerns is with the elimination of PEPFAR [President’s Emergency Plan for AIDS Relief], which was providing a lot of antiretroviral therapies to people,” and the immunity of those people will decline.
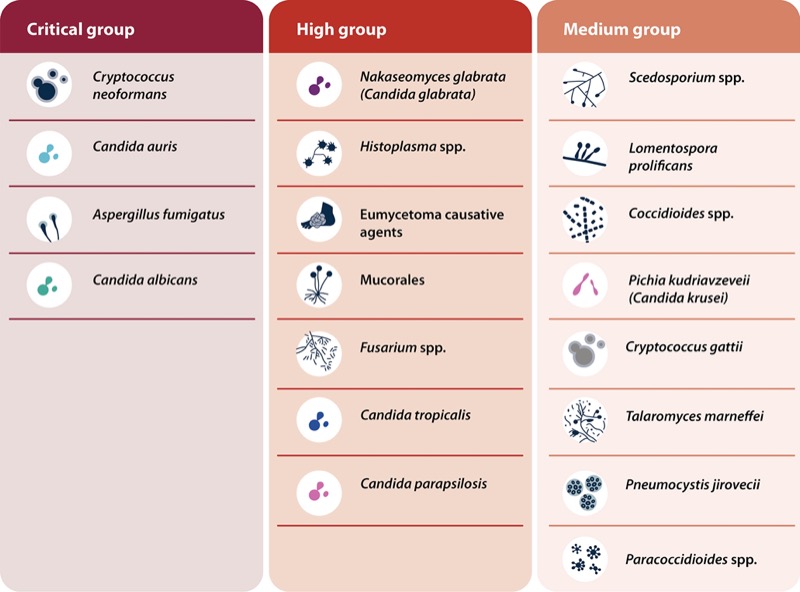
At the same time, the WHO’s list of 19 fungal pathogens to watch includes both Aspergillus and multiple species of Candida (global-pps.com/who-fungal-priority-pathogens-list/). Candida albicans, C. auris and Aspergillus fumigatus are three of the four fungi listed as critical for public health officials to control and prevent. (Cryptococcus neoformans tops the list.)
“We have a lot of problems regarding coinfections, not only the expression, but global warming,” Dr. Santos said. “Pathogens that weren’t detected before are now being detected in a lot of places.”
For now, only one fungal infection should put HIV in the differential if it has not already been diagnosed. “Fungal meningitis is an HIV-defining disease,” Dr. Santos said.
Low CD4+ counts are associated with cryptococcal meningitis infections in people with HIV and remain a major cause of mortality. The infection almost always occurs in people who are not taking ART, often because they do not know they’ve been infected.
“In Baltimore, we see this several times a year. People don’t know they have HIV, and they show up at the ER with an invasive fungal infection and are then diagnosed with HIV. That is still happening in the U.S.,” Dr. Casadevall said.
The sources reported no relevant financial disclosures.
This article is from the October 2025 print issue.