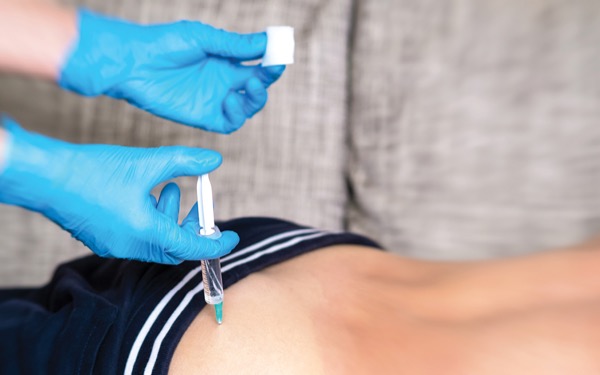
Results from a phase 4 study demonstrated that long-acting injectable cabotegravir (CAB-LA; Apretude, ViiV Healthcare) was an effective HIV-1 pre-exposure prophylaxis (PrEP) option over a one-year period in men who have sex with men (MSM) and transgender men, according to data presented at CROI 2025, in San Francisco (abstract 196).
“We’ve come super far in our ending the HIV epidemic war, but we’re not there yet,” said author Taimur Khan, MD, an infectious disease specialist and the associate medical research director of The Fenway Institute, in Boston. “The last part is getting the prevention and treatment into the hands of the people that need it the most, and this study did two of those things and provided a new modality that is less frequent and cumbersome for patients.”
CAB-LA is injected every two months and is the only long-acting PrEP medication that is approved by the FDA. However, there are barriers to its use, according to Patrick Sullivan, DVM, PhD, a professor of epidemiology in the Rollins School of Public Health at Emory University, in Atlanta. “Although the efficacy of PrEP is clear from clinical studies, we know that only about one-third of people who would benefit from PrEP are taking it,” he said.
Some of the biggest challenges underserved populations can face include lack of awareness, high out-of-pocket costs for people and a stigma that can be associated with PrEP use, he explained.
“In our own research, we have observed that some participants discontinue PrEP because they don’t have a private place to store their medications and are concerned what a roommate or others might think if they knew that a PrEP user had antiretroviral medications in their possession,” Dr. Sullivan said.
The PILLAR study assessed how CAB-LA was administered to MSM and transgender men at 17 clinics across the United States. Overall, 201 participants enrolled from May 2022 to August 2023, and 6% were transgender men. Researchers assessed HIV incidence, HIV diagnostic testing, safety and tolerability, and persistence, which is the length of time that a person continued to receive injections of cabotegravir.
“Persistence was key because we wanted to determine if we have the capability to have people stay on the medication for a long time. The good news is that we found that 85% of people that were in the study stayed on it through six months, and then by the end of the year or six or seven injections [later], about three-quarters of people were staying on the medication,” he said.
A total of 70% (or 141) of participants completed all of the study injections, with five patients missing an injection and receiving oral cabotegravir or an alternative PrEP, both of which have to be administered more frequently. Of note, no new cases of HIV were observed during the 12-month period.
“The findings from the research about long-acting injectable PrEP speak directly to the importance of having convenient options for PrEP, and especially for the importance of PrEP formulations that don’t require daily pill taking,” Dr. Sullivan said.

A companion study to PILLAR called EBONI is expected to be completed this year. It is evaluating CAB-LA administration for Black cis- and transgender women at 20 clinics. A number of other future PrEP studies are planned as well.
“I think the long-term goal for injectable PrEP is to make them less tedious and have fewer requirements to be able to get it,” Dr. Khan said.
To ensure the people who need PrEP receive it, Drs. Khan and Sullivan stressed the importance of giving patients multiple pathways to access the treatment.
“Preferences for one formulation or dosing schedule for PrEP will vary based on personal preference, out-of-pocket costs, living circumstances and relative importance of convenience and flexibility in regimens,” Dr. Sullivan said.
Dr. Khan received logistical support for presenting data at CROI by ViiV Healthcare. Dr. Sullivan reported no relevant financial disclosures.
This article is from the June 2025 print issue.