By IDSE News Staff
Current or previous use of the antiretroviral (ARV) drug abacavir was associated with an elevated risk for major adverse cardiovascular events (MACE) in people with HIV, according to an exploratory analysis from a large international clinical trial that was presented at AIDS 2024, in Munich.
There was no elevated MACE risk for the other ARVs included in the analysis.
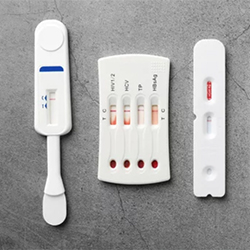
REPRIEVE (the Randomized Trial to Prevent Vascular Events in HIV) enrolled 7,769 study participants with HIV from 12 countries that found daily use of a cholesterol-fighting statin drug reduced the risk for MACE, such as myocardial infarctions and strokes, by more than one-third. The REPRIEVE study team also performed statistical analyses to assess whether selected ARVs were associated with MACE risk among study participants, all of whom had low to moderate cardiovascular disease (CVD) risk. The ARVs selected for analysis had been linked to CVD risk and included abacavir, tenofovir, zidovudine, stavudine and several protease inhibitors (PIs). All were taken as part of multidrug ARV regimens.
Overall, 22% of study participants reported prior exposure to abacavir, 86% to tenofovir, 49% to zidovudine or stavudine, and 47% to PIs. At study entry, 13% of participants were taking abacavir, 61% tenofovir, 10% zidovudine or stavudine, and 26% PIs. In the investigators’ analyses, participants with prior and current use of abacavir had a 50% and 42% elevated risk for MACE, respectively, compared with participants with no abacavir exposure. Former or current use of other ARVs was not associated with any change in MACE risk, and the coadministration of common ARV drug classes as part of an ARV regimen did not affect the elevated MACE risk among participants with current or prior abacavir exposure.
According to the researchers, these findings align with previous studies that also identified an elevated CVD risk associated with abacavir.
They suggested that more research is needed to better understand the increased risk observed in this analysis, including how these findings should be considered in the context of known CVD risk factors, such as dyslipidemia, diabetes and hypertension, for people with HIV.