By Marie Rosenthal, MS
Updated May 9 with latest CDC data
The total number of measles cases as of May is more than three times higher than previously reported all of last year.
As of May 1, 2025, a total of 1001 cases of measles have been confirmed by 31 jurisdictions in the United States; by Dec. 31, 2024, a total of 285 measles cases were reported by 33 jurisdictions. Fourteen separate outbreaks (defined as three or more related cases) have been reported to date in 2025, and 93% of confirmed cases (869/935) are outbreak-associated, according to the CDC. For comparison, 16 outbreaks were reported during 2024, and 69% of cases (198/285) were outbreak-associated. In 2023, four outbreaks were reported, and 49% of cases (29/59) were outbreak-associated.
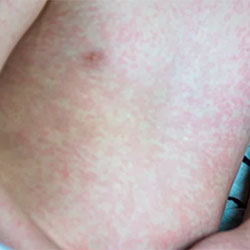
Most of the cases are among unvaccinated children.
The 2025 outbreaks also lead to a record-breaking three deaths, among two children and one adult. A child has not died from measles in this country since 2003, when two children and one adult died from the disease. The last U.S. measles death occurred in 2015, killing an immunocompromised adult.
The largest outbreak in Texas, New Mexico and Oklahoma began in January and is affecting primarily members of a close-knit community with low rates of measles vaccination (MMWR Morb Mortal Wkly Rep 2025;74[14]:232-238).
High coverage of the two-dose schedule of measles-mumps-rubella (MMR) vaccine among children enabled the United States to declare measles eliminated—meaning the absence of the continuous spread of disease was longer than 12 months—from the United States in 2000, the epidemiologists from the CDC and several state health departments wrote.
“However, measles cases and outbreaks continue to occur when travelers with measles return to the United States while they are infectious; larger U.S. outbreaks typically follow importation into close-knit communities with low vaccination coverage,” they wrote.
But the report, which discusses measles cases from Jan. 1 to April 17, when there were 800 cases, said the risk for widespread measles transmission was low because most of the country still has a high level of immunity.
“To prepare for and prevent measles cases and outbreaks, public health departments should continue working with trusted community messengers on culturally competent community engagement, education, vaccination efforts and other community infection prevention approaches (e.g., case isolation, contact monitoring, and post-exposure prophylaxis) and coordinating with health care facilities and schools,” they wrote.
“Increasing national and local MMR vaccination coverage is essential to preventing measles cases and outbreaks,” they wrote.
In March, the Department of Health and Human Services declared the 2025 measles outbreaks were “a call to action for all of us.”
In related news, Robert F. Kennedy Jr. will enlist the “entire” Department of Health and Human Services “to activate a scientific process to treat a host of diseases, including measles, with single or multiple existing drugs in combination with vitamins and other modalities. This process will work collaboratively with universities across the country to develop protocols, testing, and approval of new therapeutics that are safe and effective and meet the highest standards of science,” according to an HHS spokesperson, who provided information on background.
In answer to an email, the spokesperson told Infectious Disease Special Edition the CDC continues to recommend MMR vaccination as the best method for preventing disease. “At the same time, we recognize that some individuals and communities across the U.S. may choose not to vaccinate. Our commitment is to support all families—regardless of their vaccination status—in avoiding hospitalization and serious complications from measles, including death,” the email said.
The CDC released a toolkit that offers “a range of options tailored to meet communities where they are.”