By Ethan Covey
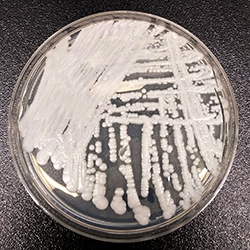
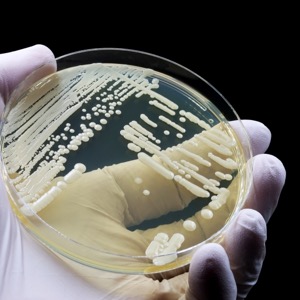
Although infections caused by Candida auris are a growing concern in healthcare facilities, strict adherence to standard infection prevention and control (IPC) protocols appears adequate to prevent the spread of C. auris in settings providing hemodialysis services (MMWR Morb Mortal Wkly Rep 2025;74:415-421).
“Prior to this report, there was very little published regarding transmission of C. auris in the dialysis setting,” said the study’s lead author, Alexandra Kurutz, MPH, an epidemiologist with the Tennessee Department of Health.“Experimental research and extrapolation from other healthcare settings create a foundation for understanding how emerging pathogens are transmitted and maintained in the healthcare environment, but applied epidemiology reports like this one are also important to understand what is really happening in the field.”
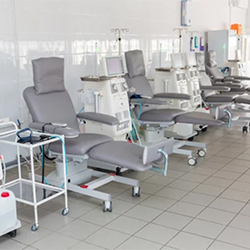
The study focused on five renal dialysis facilities located in four U.S. states—New Jersey, North Carolina, South Carolina and Tennessee—from 2020 through 2023. During this period, six patients infected or colonized with C. auris received dialysis treatment for up to four months. The C. auris status of five of the patients was unknown to the facilities where they received dialysis treatment.
The study found the use of standard IPC practices—not C. auris-specific efforts—prevented further spread of the infections in the five facilities that were unaware of positive C. auris cases.
The report highlights the difference in standard dialysis IPC precautions compared with other healthcare settings and how those practices may be helping prevent transmission of organisms such as C. auris.
“Dialysis facilities already use bleach solutions as their primary disinfectant, which we know to be effective against C. auris, and elements of personal protective equipment (PPE) are used and changed for each patient as a standard,” said senior author, Simone Godwin, DVM, an epidemiologist with the Tennessee Department of Health. “Patients also typically receive dialysis on an outpatient basis and are only present in the facility a few hours, which may have a reduced risk than when patients are admitted to a hospital or nursing home for extended periods.
“On the other hand, dialysis treatment poses some additional risks, such as an immunocompromised patient population and the frequent access of indwelling devices,” Dr. Godwin added. “The standard dialysis IPC practices already address many of those risks, but additional precautions as outlined in the report add an extra layer of safety for this vulnerable patient population. From the clinical perspective, a recent paper by Zoi et al. also suggested the use of targeted antifungal lock protocols [Int Urol Nephrol 2025 June 13. doi:10.1007/s11255-025-04600-4].”
Communication about a patient’s multidrug-resistant organism (MDRO) status among facilities is crucial, according to the authors. They found that lapses in communication between healthcare facilities and public health jurisdictions “posed a significant impediment to containment response efforts by most participating states.”
“This has been emphasized by CDC MDRO Prevention Strategies, but these communication gaps can also occur when patients are transferred to healthcare settings other than hospitals and nursing homes,” Ms. Kurutz added.
“Prompt and accurate information sharing between a healthcare facility and dialysis setting using tools like interfacility transfer forms or Antimicrobial Resistance Information Exchanges where available can help the dialysis setting ensure the C. auris patient is placed on the correct precautions to ensure correct IPC practices are used.”
The sources reported no relevant financial disclosures.