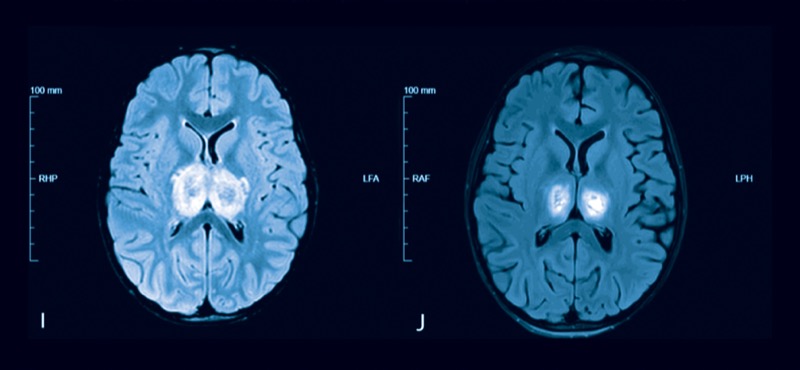
A newly released CDC report reveals that 13% of children who have died of influenza this season had influenza-associated encephalopathy or encephalitis (IAE), a severe neurologic complication.
As of Feb. 8, 2025, IAE was identified in nine of 68 children who had influenza and died. This includes four children who were diagnosed with acute necrotizing encephalopathy (ANE) (MMWR Morb Mortal Wkly Rep 2025;74[6]:91-95).
All of the ANE deaths occurred in children younger than 5 years of age with laboratory-confirmed influenza A(H1N1)pdm09, one of whom had underlying medical conditions.
Although the authors noted that it is not known whether cases observed in the 2024-2025 season vary from expected numbers, data from the Influenza-Associated Pediatric Mortality Surveillance System show that the median proportion of pediatric influenza deaths with IAE during the 2010-2011 through 2024-2025 flu seasons was 9%. Currently, no national surveillance for IAE exists in the United States.
“We know that flu can cause encephalopathy, but this appears to be more prominent than we’ve been aware of in the past,” William Schaffner, MD, a professor of preventive medicine and infectious diseases in the Department of Health Policy at Vanderbilt University Medical Center, in Nashville, Tenn., told Infectious Disease Special Edition.
“These findings are provocative, and sad,” Dr. Schaffner added. He noted that, while these preliminary data could end up being a statistical aberration, research is needed to better understand why IAE can occur in normally healthy children.
The deaths have come during a particularly brutal influenza season.
Levels of flu seem to have peaked during the week of Feb. 8. The CDC has classified the 2024-2025 flu season as a “high severity” season for all age groups—the first high severity season since 2017-2018. So far this season, there have been an estimated 44 million illnesses, 580,000 hospitalizations and 25,000 deaths from flu. By March 29, there were 168 pediatric deaths from influenza.
“Based on data from FluSurv-NET, the cumulative hospitalization rate for seasonal influenza, the week ending Feb. 22, 2025, is the highest observed since the 2010-2011 season,” Paul D. Prince, a CDC spokesperson, told Infectious Disease Special Edition.
“We have had a very serious influenza season,” Dr. Schaffner said. “It’s starting to nose down, but it has been the worst season in many years.”
Most flu cases this season have been caused by influenza A virus. Among the 1,616 influenza A viruses subtyped during the week ending March 22, 52.2% were influenza A(H1N1)pdm09 and 47.8% A(H3N2).
Interim vaccine effectiveness data released by the CDC show that the current influenza vaccine has been effective at significantly decreasing doctor visits and hospitalizations during the 2024-2025 flu season (MMWR Morb Mortal Wkly Rep 2025;74[6]:83-90).
The report shows that children who received the influenza vaccine were 32% to 60% less likely to visit a doctor because of flu and 63% to 78% less likely to be hospitalized. Among adults, those who received a flu vaccine were 36% to 54% less likely to visit a doctor due to flu, and 41% to 55% less likely to be hospitalized.
In contrast to influenza, both COVID-19 and respiratory syncytial virus (RSV) have yet to cause significant outbreaks during the 2024-2025 season. Although COVID-19 activity was elevated in many areas of the country, a large winter surge never materialized. “While we had an increase in COVID-19 this winter, it was fortunately less than expected and less than we saw last summer,” Dr. Schaffner said.
The peak hospital demand due to COVID-19 occurred during the week ending Jan. 4, 2025, with 4.2 hospital admissions per 100,000. This rate was lower than all previous seasons, and nearly 50% lower than last season’s peak.
Per the CDC, population immunity from last summer’s COVID-19 surge may have contributed to the decline in hospitalizations this season. COVID-19 vaccine uptake also has been higher this season than last year. Data as of Feb. 1, 2025, show that 22.6% of adults at least 18 years of age and older received the 2024-2025 COVID-19 vaccine, compared with 20.0% as of Feb. 3, 2024.
“For the first time since the COVID-19 pandemic, influenza-associated deaths among individuals with respiratory illness surpassed those from COVID-19,” Mr. Prince said.
Regarding RSV, preliminary CDC surveillance data for the 2024-2025 season estimate there have been 3.3 million to 6.2 million outpatient doctor visits due to RSV, 170,000 to 330,000 hospitalizations and 9,300 to 21,000 deaths through Feb. 22.
Nationally, RSV activity began to rise in October 2024, and peaked in early January 2025. “RSV came in a bit late, and appears now to be topping out,” Dr. Schaffner said.
RSV-related hospitalization reached a peak of 3.8 hospital admissions per 100,000 people during the week ending Jan. 4. This level is lower than the peak demand of 4.3 hospital admissions per 100,000 seen during last year’s respiratory virus season.
Vaccines Prove Effective
CDC data on the effectiveness of the existing COVID-19 vaccine show that, much like the influenza vaccine, it has been helpful in averting hospital visits and related hospitalizations (MMWR Morb Mortal Wkly Rep 2025;74[6]:73-82).
Among adults 18 years of age and older, those who received the 2024-2025 COVID-19 vaccine were 33% less likely to experience COVID-19–associated emergency department or urgent care visits than those who were unvaccinated. Immunocompromised adults 65 years of age and older vaccinated with the 2024-25 shot were 45% to 46% less likely to be hospitalized compared with those who did not receive a COVID-19 vaccine.
In addition, the effectiveness against hospitalizations in immunocompromised adults ages 65 and older was 40%.
“The best modern science can’t yet give us vaccines that can prevent each and every case of these illnesses,” Dr. Schaffner said. “But what they do best is prevent serious disease and deaths. And clearly, these vaccines have performed well in this regard.”
Mr. Prince commented that while “specific to this influenza season, we are experiencing high severity levels.” Overall, “this respiratory season has looked similar to pre-pandemic seasons.”
The sources reported no relevant financial disclosures.
This article is from the April 2025 print issue.