Marie Rosenthal, MS
Schistosoma haematobium infection can trigger cancer-related gene activity that may increase a person’s risk for cervical cancer. The changes become even more pronounced after treatment, according to a presentation at ESCMID Global 2025, in Vienna.
“Overall, women with parasitology clearance after treatment had an increase of or an upregulation of oncogenic pathways, genes and inflammatory genes,” said Anna Maria Mertelsmann, MD, a researcher at University Hospital Zurich and Weill Cornell Medicine, in New York City.
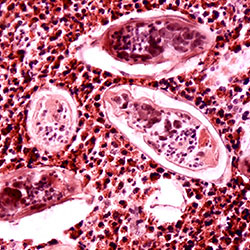
S. haematobium, one of the main species responsible for human schistosomiasis, infects more than 110 million people worldwide by depositing eggs that infiltrate the urinary and reproductive tracts. Although this parasite is recognized as a cause of bladder cancer, its potential role in cervical cancer has remained poorly understood, Dr. Mertelsmann said.
“It is well known that S. haematobium eggs can lead to bladder cancer in women when entrapped in the reproductive tract,” she said, “but it can cause female genital schistosomiasis or in short, FGS. Past research suggests that FGS can lead to an increased acquisition of viruses, such as HIV and HPV, but its role in cervical cancer remains uncertain.”
In this study, researchers analyzed cervical tissue samples from 39 Tanzanian women with (n=20) and without (n=19) S. haematobium infection. Infected women received praziquantel treatment, and samples were collected at baseline and four to 12 months after treatment. Dr. Mertelsmann and her colleagues were able to identify cancer-related pathways through RNA sequencing and gene-expression analysis. Nine genes were expressed differently between infected and uninfected women; 23 genes changed in women who cleared the infection after treatment; and 29 genes differed between women post-treatment and those who never experienced an infection.
Among the nine most significantly altered genes between infected and uninfected women, four were linked to cancer:
- BLK proto-oncogene: a tyrosine kinase that drives cell proliferation and can contribute to tumor formation when dysregulated;
- Long intergenic non-protein coding RNA 2084: a prognostic marker in head, neck and colon cancers, influencing gene regulation tied to tumor progression;
- Trichohyalin: involved in keratin complex formation and upregulated in certain cancers; and
- TCL1 family AKT coactivator A: promotes cell survival and proliferation, and is linked to T- and B-cell lymphomas.
After treatment, certain cancer-related biological pathways became more active, particularly those involved in inflammation, tissue remodeling and the breakdown of protective barriers in the cervix, according to Dr. Mertelsmann. These changes were linked to increased blood vessel formation, activation of tumor-related processes and apoptosis—a key mechanism for eliminating abnormal cells.
“The findings suggest that infection may trigger molecular changes that make women more vulnerable to cancer-related processes in the cervix, especially after treatment,” Dr. Mertelsmann explained. “One particularly concerning observation was the downregulation of genes responsible for maintaining cervical tissue integrity, including claudins and tight junction proteins. This loss of protective function could facilitate HPV infection and persistence, a major risk factor for cervical cancer.”
Dr. Mertelsmann stressed the need for greater awareness of female genital schistosomiasis, as many women with S. haematobium are also affected by this difficult-to-diagnose condition. “Women diagnosed with S. haematobium should be closely monitored for early signs of cervical tissue abnormalities,” she emphasized.
She also suggested that additional treatments, such as anti-inflammatory or immune-modulating therapies, could help counteract the harmful effects seen after treatment. Moreover, widespread HPV vaccination could play a crucial role in reducing cervical cancer risk for women affected by schistosomiasis.
A larger study following 180 women over 12 months is underway to confirm these findings.
Dr. Mertelsmann reported no relevant financial conflicts of interest.