By Ethan Covey
More testing is needed to clarify results from Moderna’s paused clinical trial of the safety and efficacy of respiratory syncytial virus (RSV) vaccines in young children, according to a discussion with the FDA’s Vaccines and Related Biological Products Advisory Committee (VRBPAC).
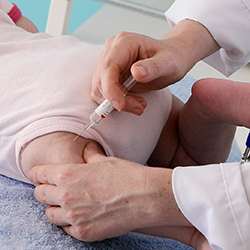
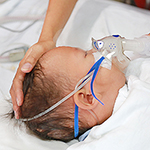
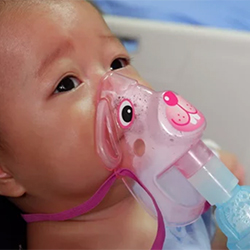
In July, Moderna stopped vaccination and enrollment in a trial focused on its RSV (mRNA-1345) and RSV plus human metapneumovirus (RSV/hMPV; mRNA-1365) vaccines, and notified the FDA and the Data and Safety Monitoring Board that some children who received the RSV vaccine had developed severe to very severe RSV lower respiratory tract infections.
“In a recent phase 1 trial, we have identified a potential imbalance of severe or hospitalized RSV in RSV-naive infants 5 to 7 months of age, with more cases in the vaccine than the placebo recipients,” said Christine Shaw, PhD, the vice president, portfolio head for Infectious Disease Vaccines at ModernaTX Inc., during a presentation to the VRBPAC in December.
Five out of 35 children (14%) in the vaccine group and one out of 18 (6%) in the placebo group exhibited this imbalance,” Dr. Shaw said. Surveillance of study participants continues. However, Dr. Shaw said, “there is currently no plan to continue this program in children younger than 2 years of age.”
In response to these results, the FDA issued a briefing document on Dec. 12, stating that U.S. pediatric RSV vaccine trials in enrolling children younger than 24 months, as well as RSV-naive children from 24 months to 5 years of age, were being halted. These results were disappointing because RSV takes an outsized toll on children, in the United States and abroad, according to the agency.
“There is a large global burden of RSV disease,” said Mark Connelly, MD, the team leader in the Division of Clinical and Toxicology Review, Office of Vaccines Research and Review at the FDA, in a presentation to the VRBPAC. “Children in low- and middle-income countries, and those under 6 months of age, are especially impacted.”
Dr. Connelly highlighted that the risk for RSV infection depends on age, with approximately 53% of U.S. infants infected by 12 months old. Nearly all children are infected at least once by 36 months of age, and reinfection with the virus is common.
“Active immunization may offer additional benefits for children, including more available RSV preventative options, immune priming to provide protection in vaccinated individuals,” he said.
During the VRBPAC meeting, members of the committee were asked to weigh in on the Moderna results and discuss how to best proceed.
Committee member Michael R. Nelson, MD, PhD, the chief of the Asthma, Allergy and Immunology Division at the University of Virginia School of Medicine, in Charlottesville, applauded the efficiency of the safety warning system and noted that more study is needed to clarify the findings.
“The system worked,” he said. “The safety signal was reached. A proper pause was put in place.”
Dr. Nelson added: “We haven't achieved enough understanding of the exact immune response of study participants, and in particular, I don't think we've learned enough from those who experienced the severe adverse events; and some more attention to be investigating what happens to them in real time, I think, could be incorporated?in future clinical trials as well.”
Henry H. Bernstein, DO, a professor of pediatrics at the Zucker School of Medicine at Hofstra/Northwell, in New Hyde Park, N.Y., called the results “an incredible conundrum,” and noted that “lots of unanswered questions remain.”
This sentiment was echoed by many of the VRBPAC members, who stressed the need to address these questions through carefully conducted trials.
“Let’s keep our eyes open, continue to do studies, gather more data, and then I think we will be able to speak on this in a more informed manner,” said Paul A. Offit, MD, the director of the Vaccine Education Center, and a professor of pediatrics at the Children’s Hospital of Philadelphia.