By Gina Shaw
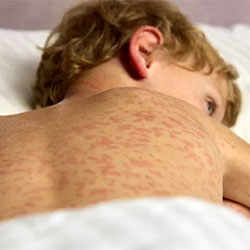
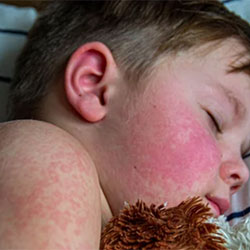
A school-age child in Los Angeles County died of subacute sclerosing panencephalitis (SSPE), a rare but devastating complication of measles infection, the California Department of Public Health (CDPH) confirmed this week. To protect confidentiality, CDPH declined to provide the child’s age or gender to Infectious Disease Special Edition, but noted the child had contracted measles as an infant—before being eligible for routine vaccination at 12 months to 15 months.
“This case is a painful reminder of how dangerous measles can be, especially for our most vulnerable community members,” said Muntu Davis, MD, MPH, the LA County Health Officer, in a statement. “Infants too young to be vaccinated rely on all of us to help protect them through community immunity. Vaccination is not just about protecting yourself—it's about protecting your family, your neighbors, and especially children who are too young to be vaccinated.”
So far this year, LA County has reported eight measles cases, including four residents and four nonresidents who were infectious while in the county, CPDH told IDSE.
SSPE is caused by persistent measles virus infection in the brain, usually manifesting years after the initial illness. “It is one of the more devastating disorders that you will ever take care of in pediatrics,” said Paul Offit, MD, of Children’s Hospital of Philadelphia. “A child gets measles, appears to fully recover, but they have an underlying chronic measles infection of the brain. About five to seven years later—sometimes longer—the symptoms begin. They initially present with changes in personality, then motor dysfunction and ultimately descend into a vegetative state from which there is no escape. It is a uniformly fatal disease.”
SSPE is estimated to occur in roughly four to 11 per 100,000 measles infections, although risk is higher when infants are infected. No cure exists (Ital J Pediatr 2025;51[1]:173).
Measles can also trigger other forms of encephalitis. Acute disseminated encephalomyelitis develops in about 1 in 1,000 measles cases, typically within days to weeks of infection, and can leave survivors with permanent neurologic deficits. Measles inclusion body encephalitis, which most commonly affects immunocompromised patients, occurs in about 1 in 1,000 cases among those populations and is almost uniformly fatal within months (Measles Virus. In :Viruses and the Lung Springer;2013:71-78).
“These complications illustrate the many ways measles can attack the brain,” Dr. Offit emphasized. “The tragedy is that they are all preventable with vaccination. This child was unable to be vaccinated at the age when they were exposed to measles, which underscores the importance of protecting those who can’t be vaccinated through maintaining high levels of community immunity.”
Citing CDC data, a CDPH news release noted that a total of 1,454 U.S. measles cases have been reported in 2025 as of Sept. 9. “Most of these cases are linked to a measles outbreak in Texas, New Mexico, Kansas and Oklahoma. The majority of cases were unvaccinated or had unknown vaccination status. Twelve percent of these cases required hospitalization for management of measles complications or isolation, and three tragically died from acute measles-related complications,” the LA County release noted.
With measles outbreaks resurging amid vaccine hesitancy, experts warn that more of these tragedies may occur. “Unfortunately, this may be something that we will see more of if increasing rates of vaccine refusal continue,” Dr. Offit cautioned.