By Meaghan Lee Callaghan
Although it is nothing like the 3 million to 4 million cases per year of measles before an effective vaccine, measles cases this year are more than double that in 2024, according to a meeting of the CDC Advisory Committee on Immunization Practices (ACIP).
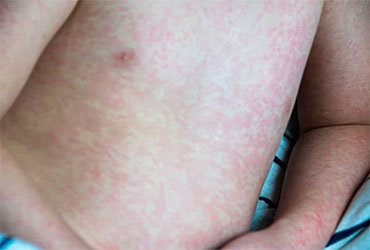
Newly updated numbers as of April 18 count 800 confirmed cases of measles in the United States.
The vast majority of cases (90%) are centered around a close-knit community in Gaines County, Texas, where the two-dose vaccine coverage in public schools is only 82%, and potentially lower in private school and homeschool which do not have required reporting of coverage, according to presenter Capt. David Sugerman, MD, MPH, FACEP, USPHS, the senior scientist of the 2025 Measles Response. Dr. Sugerman reported that this outbreak has spread to 21 additional counties in Texas and three counties in neighboring New Mexico.
Falling Vaccination Rates
What is one cause of this bad measles year? The 95% vaccination rate needed for herd immunity has fallen steadily since the COVID-19 pandemic, Dr. Sugerman said. Data for 2023-2024 in this country show that approximately 280,000 (7%) of kindergarteners didn’t have documentation of two doses of the measles, mumps and rubella (MMR) vaccine. However, coverage is different depending on location. In certain states, such as New York, Massachusetts, West Virigina and Tennessee, there is at least 95% coverage; but in other states, such as Wisconsin, Minnesota, Ohio, Florida, New Hampshire and Alaska, coverage rates are less than 90%. Furthermore it differs by county, too.
“Since the COVID-19 pandemic, we’ve had a measles resurgence due to increased international measles transmission abroad, a surge in international travel and declines in measles vaccination, especially in close-knit communities with already low vaccine coverage,” Dr. Sugerman said. The confirmed caseload has steadily increased from 59 in 2023, 285 in 2024, and now 800 in 2025.
Retaining Elimination Status
There have been 11 large outbreaks since elimination (defined as more than 50 cases); however, seven of these have only occurred in the last five years. The majority (nine outbreaks) were seen among close-knit communities with low vaccination coverage, Dr. Sugerman said.
Although the number of separate outbreaks is lower than last year (seven compared with 16), a higher proportion of cases is now related to the outbreaks (93% vs. 68%), with five outbreaks ongoing. “We’ll be tracking duration, working closely with our state and local partners, to ensure we don’t cross the 12-month threshold and preserve our elimination status,” Dr. Sugerman said.
Although half of states are showing cases, “most states are reporting no or limited further spread from importations,” he noted.
International outbreaks are also contributing factors. Currently there is also an outbreak in a close-knit community in Ontario, Canada, which borders Minnesota through New York, and another outbreak in Chihuahua, Mexico, bordering Texas and New Mexico.
Although over 90% of current measles cases are connected to the outbreak in the Southwest, there are unrelated cases that are mostly importations and are coming from travel to Canada or Vietnam.
“Measles virus genotyping plays an important role in tracking transmission pathways during an outbreak investigation—in other words, the connection between cases,” Dr. Sugerman said. Only two are currently in circulation: B3 and D8. D8-9179 is the most common and found in Texas, Oklahoma, New Mexico and Kansas, as well as in Chihuahua and Ontario. The majority of B3 cases are from Vietnam, he said.
Outbreak Specifics
The majority of U.S. cases are in unvaccinated children with a median age of 8 years. Almost all (97%) are unvaccinated or have an unknown status. “The reasons for unknown vaccination status are multifactorial,” Dr. Sugerman said. “First, Texas has an opt-in immunization information system requiring patient consent to share immunization records with public health, and second, adults often do not have access to their vaccine records.”
In addition, 1% of cases involve one dose of MMR and 2% have two doses. Of these total cases, 12% were hospitalized, which is lower than the typical 20%, he said.
In the hospitalized population, 68% are unvaccinated and 31% were unknown status, he said.
“Very sadly, three deaths have been reported,” Dr. Sugerman said. “The two from Texas were among unvaccinated school-aged children without any past medical history. Measles was also detected following the death of an unvaccinated adult from New Mexico; the official cause of death is still under investigation by the New Mexico Office of the Medical Investigator.”
Fighting the Outbreaks
What can be done to combat these outbreaks? The CDC has sent both experts’ boots on the ground and virtual expertise to tackle measles. “On the ground, we've provided infection prevention control assistance to seven healthcare facilities with ventilation assessments and proposed solutions; reviewed school infection control activities and risk mitigation strategies; developed an internal dashboard for Texas to track cases by location and exposure location; and supported measles prevention communication,” Dr. Sugerman said. “Our team at headquarters continues to provide remote technical assistance to multiple state health departments to include laboratory diagnostics and genomic sequencing of the virus; guidance on postexposure prophylaxis; healthcare infection prevention; case investigation and confirmation; and communication support.
“We're holding bi-weekly national measles calls with public health partners to provide a forum for CDC and health departments to share information regarding the measles outbreak, and bi-weekly trilateral calls with Canada and Mexico to share updates and best practices. CDC's immunization services division continues to make additional outbreak-related MMR vaccine doses available for health departments to order at their request.”