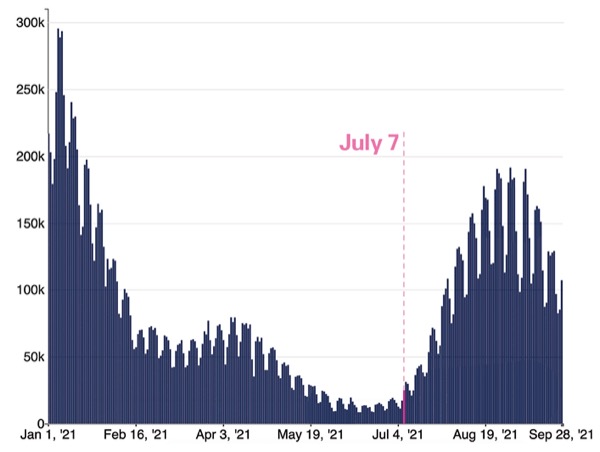
We had finally figured out the rhythm of COVID-19. There were ways to detect SARS-CoV-2, treat SARS-CoV-2 infection and prevent COVID-19. Cases had plateaued and were starting to decline, and people began going about their business, going back to work, visiting friends and family, taking vacations and enjoying dinner in restaurants.
However, some people had their own take on the pandemic and resisted the mitigation actions that were still in place, particularly mask wearing and vaccination, and as the United States headed into those hot, steamy summer days, there was yet another surge.
In late June, the seven-day moving average of reported cases was around 12,000. On July 27, it was more than 60,000, which was similar to the case rate seen before COVID-19 vaccines became available, according to the CDC.
By Sept. 7, the United States passed a landmark: 40 million positive cases of COVID-19 since the start of the pandemic, with more than 4 million occurring in just a couple of weeks in August. Along with that increase in cases, the country saw an increase in hospitalizations and deaths, mostly among the unvaccinated.
By Sept. 8, a total of 652,480 people had died from COVID-19 in the United States—one in every 500 people.
On Sept. 21, the nation hit the saddest milestone: U.S. deaths from COVID-19 totaled 676,200, more than the estimated 675,000 Americans who died in the 1918-1919 influenza pandemic, making COVID-19 the worst pandemic in U.S. history. More than 9,000 people were hospitalized, and more than 1,500 were dying each day.
Striking a Dominant Chord
The delta variant quickly surpassed the wild-type strain and other variants to become the dominant strain circulating in the United States. Of sequenced specimens, 99% have been identified as delta by the CDC’s surveillance laboratories as of Sept. 24.
In fact, the wild-type SARS-CoV-2 strain can no longer be detected, and “variants of the virus that causes COVID-19 are now responsible for all cases in the United States,” the CDC said.
“This variant [delta] is certainly a concern because of the evidence that it is more transmissible,” said Jay C. Butler, MD, FIDSA, the deputy director for infectious diseases at the CDC during a press briefing in July. “More transmissible” might have been an understatement, because the delta variant’s basic reproduction number (R0) is twice the original SARS-CoV-2 strain (R0, 5 vs. 2.5).
Mutations are always a concern because there is a chance they can develop resistance to therapeutics or reduce vaccine efficacy, according to Dr. Butler.
All of the variants have been a concern, but none more so than B.1.617.2, commonly called delta, because of its transmissibility and some data that point to it causing more severe disease, according to CDC Director Rochelle P. Walensky, MD.
“It is one of the most infectious respiratory viruses we know of and that I have seen in my 20-year career,” she said at a briefing this summer.
Emergency departments (EDs) and hospitals started filling up, which increased the unease. One ED at the UC Davis Medical Center, in San Diego, saw a 33% increase in COVID-19 patients during the first week of August. The proportion of ED patients diagnosed with COVID-19 had tripled between June 21, when it was 0.6%, and Sept. 5, when it was 1.8%, according to the CDC.
Most of the cases occurred in people who had not received COVID-19 vaccination, and states with low vaccination rates, mostly in the South and West, saw the worst of the surge, but delta affected every state in the country.
Several states declared crisis standards of care. Rationing of care in Alaska, Idaho, Kentucky, Montana, New Mexico, Ohio and Wisconsin began in September due to a shortage of beds and hospital staff. Physicians were triaging patients based on their prognosis (Crisis Standards of Care: Summary of a Workshop Series. https://www.ncbi.nlm.nih.gov/ books/ NBK32753/ ).
“Our health care professionals are accustomed to providing the best care they possibly can for their patients, but resources are now stretched to a point that most of us never expected to see in our careers. Difficult decisions will need to be made over whose care should be prioritized, and we’re here to support our providers to provide the best care for as many patients as possible during these challenging times,” said Alaska’s Chief Medical Officer Anne Zink, MD, FACEP-ASTHO.
The CDC formed COVID-19 rapid response teams to help states, but by press time Infectious Disease Special Edition had not heard from the agency about how many teams were dispatched.
Some data indicate the delta variant might cause more severe illness than previous variants in unvaccinated people.
In two different studies from Canada and Scotland, patients infected with the delta variant were more likely to be hospitalized than patients infected with the alpha variant (B.1.1.17) or wild-type SARS-CoV-2. The Canadian study, which looked at variants of concern (VOC) that were circulating in Canada from February to June found that the adjusted increase in risk associated with delta was 108% (80%-138%) for hospitalization, 234% (164%-331%) for ICU admission and 132% (47%-230%) for death (MedRxiv 2021 Aug 4. doi:10.1101/2021.07.05.21260050).
“The progressive increase in transmissibility and virulence of SARS-CoV-2 VOCs will result in a significantly larger, and more deadly, pandemic than would have occurred in the absence of VOC emergence,” the authors concluded.
The Scottish study looked at surveillance data between April 1 and June 6. There were 19,543 confirmed cases of COVID-19, of whom 377 were hospitalized. Although they saw more younger people hospitalized than earlier in the pandemic, most of the hospitalizations were among older people and people with multiple comorbidities. “Risk of COVID-19 hospital admission was approximately doubled in those with the Delta VOC when compared to the Alpha VOC, with risk of admission particularly increased in those with five or more relevant comorbidities,” they wrote (Lancet 2021;397[10293]:2461-2462).
In the United States, most hospitalizations and death caused by COVID-19 during the surge were among unvaccinated people. Low vaccine uptake is what drove the most recent surge, according to Dr. Butler.
When delta began to assert dominance, only 49% of people in the United States were fully vaccinated, and the experts who worried that low vaccination rates and disregard of mitigation efforts would allow the virus more opportunities to mutate were proved correct.
Blue Note
Data continue to come in about whether the COVID-19 vaccines are effective against the infection. Early data point to high efficacy for hospitalizations and death, but lower efficacy against infection.
“CDC data continue to show the power of vaccination, with recent reports showing a fivefold reduction in the risk for infection, 10-fold reduction in the risk for hospitalization, and 11-fold reduction in the risk for death after vaccination,” said Dr. Walensky on Sept. 24.
An analysis by Public Health England found that the Pfizer-BioNTech messenger RNA (mRNA) vaccine (Comirnaty) was 96% effective against hospitalization, which is comparable to the effectiveness against the alpha variant (https://bit.ly/ 3m1mT6m-IDSE), but reports from Israel claim the vaccine is only 64% effective against delta in preventing infection and symptomatic illness. “Nevertheless, the vaccine maintains an effectiveness rate of about 93% in preventing serious illness and hospitalizations, they said (https://www.gov.il/ en/ departments/ news/ 05072021-03).
Recent data published by the CDC examined vaccine efficacy across nine states based on 32,867 medical encounters, including 14,636 hospitalizations between June and August 2021, during the time when the delta variant became predominant in the United States. In the analysis, the Moderna COVID-19 vaccine efficacy against COVID-19 urgent care or ED visit was 92% (95% CI, 89%-93%) and against hospitalization was 95% (95% CI, 92%-97%) at a median of 96 and 106 days, respectively, after vaccination. Across all age groups, efficacy was reported to be significantly higher for the Moderna vaccine than other COVID-19 vaccines (MMWR Morb Mortal Wky Rep 2021;70[37]:1291-1293).
A study from Canada found that both mRNA vaccines were highly effective at preventing hospitalizations, but less effective in preventing symptomatic infection (Pfizer, 87%; Moderna, 72%) (medRxiv 2021 Jul 3. https://doi.org/ 10.1101/ 2021.06.28.21259420).
The Johnson & Johnson single-dose adenovirus vaccine has an efficacy of about 85% in protecting against severe disease, hospitalization and death, according to one trial (N Engl J Med 2021;384:2187-2201).
Breakthrough infections have been reported in people who are fully vaccinated. A May 28 report said there were 10,262 breakthrough infections in 46 states as of April 30, out of 101 million people who were fully vaccinated (MMWR Morb Mortal Wkly Rep 2021;70[21]:792-793).
Even if the rate is low, there is concern about continued transmission, according to Dr. Walensky. “Some vaccinated people infected with the delta variant after vaccination may be contagious and spread the virus to others,” she said. “The science is worrisome.”
Vaccination has arguably been the most contentious COVID-19 issue, with many people still hesitant to receive their shots.
Many states, health systems and long-term care facilities, and companies have made COVID-19 vaccination a condition of employment.
In fact, tired of cajoling and begging people to be vaccinated, President Joe Biden announced a similar policy for federal workers and federal vendors in September.
In addition, he expanded his requirement that all nursing home employees who treat Medicare and Medicaid patients be vaccinated to include all health care workers who work in hospitals, home health care or other medical facilities that accept Medicare and Medicaid patients. “If you are seeking care at a health facility, you should be able to know that the people treating you are vaccinated. Simple. Straightforward. Period,” he said.
But it isn’t quite so simple. Several states, including California and New York, have also said state workers must be vaccinated as a condition of employment, even though they faced staff shortages. But many people are complying. As Infectious Disease Special Edition went to press, most of New York's health care workers were lining up for the shot by the Sept. 27 deadline: 87% of hospital workers and 92% of long-term care staff had received at least one vaccine. California is seeing similar success.
On Sept. 22, the FDA approved a booster dose of the Pfizer-BioNTech vaccine for people ages 65 years and older and individuals at high risk for severe COVID-19, as well as those whose work puts them at risk for COVID-19 infection, such as health care workers and teachers. Among the data considered for the approval, the FDA looked at data presented from Israel that included an analysis of about 1.1 million people, 60 years and older, who were eligible for a booster dose of the vaccine between July 30 and Aug. 31. The booster dose restored very high levels of protection against COVID-19 infection and severe disease against the delta strain. People who received a booster dose were less likely, by a factor of 11.3 (95% CI, 10.4-12.3), to develop a confirmed infection and less likely by a factor of 19.5 (95% CI, 21.9-29.5) to develop severe disease than those who were fully vaccinated but did not receive a booster dose (N Engl J Med 2021 Sep 15. doi:10.1056/NEJMoa2114255).
With news of waning immunity came recommendations for boosters and third doses. The FDA expanded its emergency use authorization (EUA) and the CDC recommended a third dose for anyone with a weakened immune system, such as those with cancer, in early September.
Then the FDA expanded the EUA for the Pfizer-BioNTech mRNA vaccine to allow boosters six months after the primary series for a wide group of people, including those with an occupational exposure such as health care workers, and the CDC endorsed that recommendation. Both Moderna and J&J have asked the FDA to consider boosters for their COVID-19 vaccines, and the FDA's advisory committee will take up the requests on Oct. 14-15.
Not everyone agrees that those with an occupational exposure should receive boosters. In fact, the Advisory Committee on Immunization Practices, which advises the CDC, did not recommend it. In a highly unusual move, Dr. Walensky decided not to accept that recommendation and instead aligned with the FDA’s EUA.
“As CDC Director, it is my job to recognize where our actions can have the greatest impact. At CDC, we are tasked with analyzing complex, often imperfect data to make concrete recommendations that optimize health. In a pandemic, even with uncertainty, we must take actions that we anticipate will do the greatest good,” Dr. Walensky said in a statement, released after that recommendation was made.
“I believe we can best serve the nation’s public health needs by providing booster doses for the elderly, those in long-term care facilities, people with underlying medical conditions, and for adults at high risk of disease from occupational and institutional exposures to COVID-19. This aligns with the FDA’s booster authorization and makes these groups eligible for a booster shot,” she added.
As of Sept. 29, only 55.5% of Americans were fully vaccinated, but 64.5% have had at least one dose. If one just looks at adults, 66.8% are fully vaccinated and 77.2% have had at least one dose, and 2.4 million people have received a third dose.
What is clear is there is no coda for COVID-19 more than 19 months into the pandemic, and although America is not recommending that everyone sequester at home, mitigation actions, such as masking and social distancing, have been reinstituted in many places, even for those who are vaccinated. So, the rhythm of COVID-19 has adapted once again.
The way out of the pandemic, according to public health officials, remains vaccination, and the goal is to vaccinate the unvaccinated, and give boosters to those who need it to increase their immune response against infection.
“Vaccinating the unvaccinated remains a high priority, and we must not lose sight of this goal with all the discussion around booster shots. That is why we will continue our efforts to reach those who are not yet vaccinated, using a combination of increased access and community-based information campaigns to help people get accurate scientific information from sources they trust,” said Vice Adm. Vivek J. Murthy, MD, MBA, the surgeon general.
“Getting our nation vaccinated remains our most important path out of this pandemic,” he said.
{RELATED-HORIZONTAL}