By Marie Rosenthal, MS, and Ethan Covey
We’ve got a nice mix for you this week. A new mouse model study found that a COVID-19 vaccine does not affect fetal growth or cause birth defects, so perhaps putting some vaccine misinformation to rest. Two new technologies, a special type of MRI and an artificial intelligence tool might help overcome the challenges of visualizing the lung damage in long-COVID patients. Two Chicago get-togethers give new meaning to the phrase, “party hard.” And finally, researchers out of the Netherlands wanted to answer the question: Why did some people weather the pandemic emotionally better than others? (Hint: you might be able to thank your mom and dad.)
COVID-19 Vaccine Does Not Affect Fetal Growth or Cause Birth Defects
Despite growing evidence that COVID-19 vaccination during pregnancy can benefit both mother and child, safety concerns are a significant cause of vaccine hesitancy. Popular claims, in particular, hold that vaccination during pregnancy could harm the fetus, and that vaccination prior to pregnancy could reduce female fertility.
 Image by Hannah J. Lee (CC-BY 4.0, https://creativecommons.org/licenses/by/4.0/)
Image by Hannah J. Lee (CC-BY 4.0, https://creativecommons.org/licenses/by/4.0/)The scientists also injected other pregnant mice with a substance known as poly(I:C), which simulates viral infection; fetuses from these mice had reduced growth. Overall, the mouse experiments suggest that vaccination during pregnancy is safer for both mother and fetus than infection during pregnancy.
Next, the researchers collected blood samples from both vaccinated and unvaccinated human volunteers. They found that those who had been vaccinated did not have elevated levels of antibodies against the protein syncytin-1, suggesting that fears of reduced fertility due to COVID-19 vaccination’s effects on this protein are unfounded.
The authors noted that, as more people are vaccinated and clinical trials progress, the resulting data will continue to address widespread concerns about vaccination. In particular, they noted, it will be useful to confirm that COVID-19 vaccination is safe at all stages of pregnancy.
“This work provides evidence in a mouse model that vaccination in early pregnancy does not harm fetal growth or development, and instead protects the fetus throughout later stages of pregnancy,” Ms. Lu-Culligan added. “It also directly challenges misinformation deterring many nonpregnant people from vaccination. We show that the antibodies generated by vaccination do not target a rumored placental protein and that these misconceptions around infertility are not supported by the data.”
Image: Hyperpolarized xenon 129MRI, or Hp-XeMRI, has shown promise in detecting abnormalities of alveolar gas exchange—where oxygen moves from the lungs to the bloodstream and
carbon dioxide passes from the blood to the lungs—even when CT scans and lung function tests were normal. Image courtesy of Radiological Society of North America
MRI Finds Lung Abnormalities in Nonhospitalized Long-COVID Patients
A special type of MRI found lung abnormalities in patients who had had COVID-19, even those who had not been hospitalized with the illness (Radiology 2022 May 24. https://doi.org/10.1148/radiol.220069).
More than 200 symptoms have been reported from patients with long COVID, but the most common are breathlessness, fatigue and brain fog. COVID-19 can cause lasting harm to the lungs, but doctors have struggled to visualize this damage.
A novel imaging technique, hyperpolarized xenon 129MRI, or Hp-XeMRI, has shown promise in detecting abnormalities of alveolar gas exchange—where oxygen moves from the lungs to the bloodstream and carbon dioxide passes from the blood to the lungs—even when CT scans and lung function tests were normal. Hp-XeMRI enables the assessment of ventilation and gas exchange into red blood cells. It provides regional information of pulmonary vasculature integrity and may be able to identify lung abnormalities not apparent on CT.
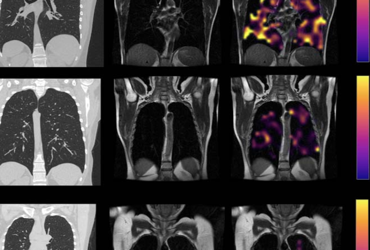 Example CT, proton, proton and RBC:TP imaging from post-Covid-19 condition participants. The top row is a participant with RBC:TP=0.49, the middle row is a participant with RBC:TP of 0.31, and the bottom row is a participant with RBC:TP=0.24. Imaging showed little to no discernible damage on CT, and yet highly heterogeneous and low RBC:TP in the lungs of non-hospitalized post-Covid-19 condition participants. RBC:TP = Hyperpolarized 129Xenon MRI lung ratio of red blood cell spectral peak to tissue phase spectral peak Courtesy of the Radiological Society of North America.
Example CT, proton, proton and RBC:TP imaging from post-Covid-19 condition participants. The top row is a participant with RBC:TP=0.49, the middle row is a participant with RBC:TP of 0.31, and the bottom row is a participant with RBC:TP=0.24. Imaging showed little to no discernible damage on CT, and yet highly heterogeneous and low RBC:TP in the lungs of non-hospitalized post-Covid-19 condition participants. RBC:TP = Hyperpolarized 129Xenon MRI lung ratio of red blood cell spectral peak to tissue phase spectral peak Courtesy of the Radiological Society of North America.For this prospective study, researchers determined whether previously described lung abnormalities on Hp-XeMRI in post-hospitalized COVID-19 participants are also present in nonhospitalized participants with long COVID.
Eleven nonhospitalized long-COVID participants (240-334 days from infection) and 12 post-hospitalized COVID-19 participants (105-190 days from infection) were enrolled from June 2020 to August 2021. All participants had symptoms of breathlessness. As a control group, healthy volunteers with no evidence of prior COVID-19 infection were recruited from staff at the University of Sheffield and the University of Oxford, in England.
Participants were given chest CT scans, Hp-XeMRI, pulmonary function tests, one-minute sit-to-stand tests and breathlessness questionnaires. Control participants underwent HP-XeMRI only. CT scans were analyzed for post–COVID-19 lung disease severity using a previously published scoring system, and full-scale airway network modeling. Analysis used group and pairwise comparisons be-tween participants and controls, and correlations between participant clinical and imaging data. Normal or near-normal CT scans were seen in both COVID-19 patient groups.
The results showed that there were significant differences in the mean red blood cell-to-tissue plasma ratio between healthy controls and post-hospitalized COVID-19/nonhospitalized long-COVID participants, indicating potential differences in lung function. Although participants had normal or near-normal CT scores, total lung diffusion capacity for carbon monoxide percentage was significantly lower between the nonhospitalized and hospitalized participants, potentially indicating a de-crease in lung function but not structure.
“We saw that the ability of gas to transfer from the lungs into the bloodstream was less in nonhospitalized pa-tients in comparison to those hospitalized with COVID,” said Fergus Gleeson, MBB, from the Department of Oncology, University of Oxford, and Department of Radiology, Oxford University Hospitals NHS Trust, in England. “Furthermore, both groups of participants had lower dissolved phase Hp-XeMRI values than healthy participants, pointing to potential defects in either the lining of the lung or the surrounding blood vessels.”
Image: A new AI diagnostic tool allows doctors to visualize lung damage caused by COVID-19 in more detail. ©2022 KAUST; Ivan Gromicho
AI Helps Diagnose Post–COVID-19 Lung Problems
Another new diagnostic tool developed by KAUST scientists could help overcome some of the challenges of monitoring lung health following viral infection (Nat Machine Intelligence 2022 May 23. doi:10.1038/s42256-022-00483-7).
Conventional chest scans do not reliably detect signs of lung scarring and other pulmonary abnormalities, which makes it difficult to track the health and recovery of people with persistent breathing problems and other post–COVID-19 complications.
The new method developed by KAUST—known as deep-lung parenchyma-enhancing (DLPE)—overlays AI algorithms on top of standard chest imaging data to reveal otherwise indiscernible visu-al features indicative of lung dysfunction.
Through DLPE augmentation, “radiologists can discover and analyze novel subvisual lung lesions,” said computer scientist and computational biologist Xin Gao, PhD. “Analysis of these lesions could then help explain patients’ respiratory symptoms,” allowing for better disease management and treatment, he added.
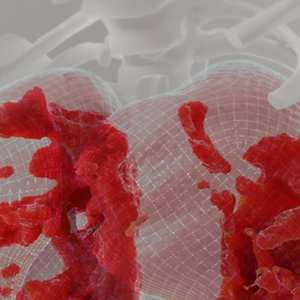
The method first eliminates any anatomic features not associated with the lung parenchyma; the tissues involved in gas exchange serve as the main sites of COVID-19–induced damage. That means removing airways and blood vessels, and then enhancing the images of what is left behind to expose lesions that might be missed without the computer’s help.
The researchers trained and validated their algorithms using CT chest scans from thousands of people hospitalized with COVID-19 in China. They refined the method with input from expert radiologists and then applied DLPE in a prospective fashion for dozens of COVID-19 survivors with lung problems, all of whom had experienced severe disease requiring intensive care treatment.
In this way, Dr. Gao and his colleagues demonstrated that the tool could reveal signs of pulmonary fibrosis in COVID long-haulers, thus helping to account for shortness of breath, coughing and other lung troubles. A diagnosis, he suggests, that would be impossible with standard CT image analytics.
Chicago Party Leads to 5-State Omicron Outbreak
A private party and dinner that took place in Chicago last Thanksgiving resulted in a multistate COVID-19 outbreak, providing further evidence of how rapidly the omicron variant can be transmitted (Emerg Infect Dis2022;28[6]:1281-1283 https://doi.org/10.3201/eid2806.220411).
“While this outbreak primarily affected invited attendees at a party held at a bar, the outbreak was notable because there were patrons of the bar who got sick who were not known to have any direct contact with the gathering,” said Hillary Spencer, MD, an Epidemic Intelligence Service officer with the CDC. “This underscores how easily the omicron variant can spread, particularly in a setting in which masks are not worn 100% of the time.”
On Nov. 27, 2021, a party was held in a Chicago bar. The same evening, many of the attendees also participated in a dinner at a private event space. A subsequent investigation identified 15 cases—14 of whom were confirmed by SARS-CoV-2 testing, and one probable case. Cases were spread across five U.S. states.
Nearly all of the cases (93%) had visited the bar where the party took place; one attended the dinner only, and one attended both events. Eighty percent of the cases were in individuals who were fully vaccinated, and their cases were mild.
“The outbreak shows the importance of being up to date on vaccines,” Dr. Spencer noted. “Most of those in the outbreak were fully vaccinated and none had severe outcomes.”
As highly infectious strains of COVID-19, such as omicron, circulate, outbreaks like this highlight the risks associat-ed with social activities, particularly when mitigation efforts are not, or cannot be, fully followed.
“Bars and restaurants pose a greater risk for COVID exposure than places where masks are worn all of the time and people can distance from others,” Dr. Spencer said. “Holidays also can lead to spread when people come togeth-er from all over the country and may take the virus back home with them.
“When choosing to engage in higher risk activities, everyone should weigh both the health risks and personal risks—such as impacted travel and work—of acquiring COVID,” she added. ”The best means of prevention remain vaccination, masking and social distancing.”
In addition, people may benefit from following local case trends when making decisions regarding participation at social events.
“People should consider personal risks such as their health and community COVID levels,” Dr. Spencer said. “When community levels are low, going to a bar might be less risky, but if community levels are high, wearing a mask or gathering outdoors can lower risk of spread.”
Genes Partly Responsible for Well-Being During Pandemic
Everyone was affected by the COVID-19 pandemic, but some people weathered the stress of the pandemic better than others, in part, due to their genetics (PLoS Genet 2022 May 12. doi:10.1371/journal.pgen.1010135).
How a person perceives their quality of life depends on a combination of factors that include the genes they inherited from their parents and environment. Studying genes related to quality of life can be complicated, but the pandem-ic allowed Lude Franke, PhD, of the University of Groningen, in the Netherlands, and colleagues to investigate how this stressful, worldwide event interacted with a person’s genetics to affect their overall well-being.
The team screened the genomes of more than 27,000 participants in the Netherlands who had donated genetic material to a biobank. Then they looked for connections between genetic variants and the participants’ responses to a series of questionnaires about lifestyle and mental and physical health given over 10 months, starting in March 2020.
The researchers found that some individuals had a genetic tendency toward better well-being than others during the pandemic. As the pandemic wore on, they also found that genetic tendency had an increasingly powerful influ-ence on how those people perceived their quality of life, potentially due to the social isolation required by strict COVID-19 containment measures. Moreover, the findings demonstrate that the contribution of genetics to complex traits like well-being can change over time.
“The COVID-19 pandemic has been a unique opportunity to investigate the impact of genetics on well-being in a time wherein we had to socially isolate ourselves. We found that it is during the first, stressful year of the pandemic that it is our nature that has gained relative impact on how we rate our lives,” said Robert Warmerdam, PhD, a co-researcher from the University of Groningen.
{RELATED-HORIZONTAL}