By Marie Rosenthal, MS
This week’s COVID-19 roundup is all about the children, and it reminds us that COVID-19 is not benign for every child. Some children have lingering complications months after being hospitalized for COVID-19. Another study found that long-COVID symptoms can occur even in children with mild disease. There are two recent studies about pregnant women: The first found that mRNA vaccines are safe for them to use, which is good news, because another found pregnant women with COVID-19 are at increased risk for cardiovascular effects if they are not vaccinated.
More Than 1 in 4 Children Hospitalized With COVID-19 or MIS-C See Lingering Complications
In one of the largest follow-up studies to date, involving 25 pediatric hospitals, more than one-fourth of children and adolescents hospitalized with COVID-19 early in the pandemic still had health problems two to four months later, either persisting symptoms or activity impairment (Pediatrics 2022 Aug 12. https://doi.org/10.1542/peds.2022-057798).
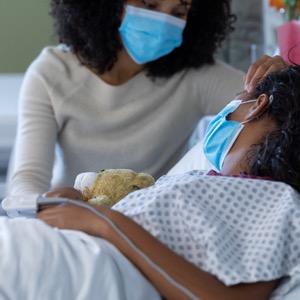
As part of the national Overcoming COVID-19 study, investigators led by Adrienne Randolph, MD, MSc, of Boston Children’s Hospital, surveyed family caregivers of patients under 21 years of age who were hospitalized with COVID-19 or multisystem inflammatory syndrome in children (MIS-C). The study period ran from May 2020 to May 2021, before vaccines were available. Of 358 patients, the researchers received survey responses from 279, or 78%.
Roughly 40% were hospitalized with acute COVID-19 and roughly 60% with MIS-C; 50% and 86%, respectively, were admitted to the ICU. At two- to four-month follow-up, 27% of patients with acute COVID-19 and 30% of those with MIS-C had persistent symptoms, activity impairment or both.
“Almost three-quarters were back to baseline, which is reassuring,” Dr. Randolph said. “But unfortunately, more than one in four were not. Although this is much better than many reports in hospitalized older adults, it is still very worrisome. The risks of severe illness and lingering complications are higher than the risk of complications from the vaccine, which are very rare.”
Of the children and adolescents with lingering symptoms, the most common symptoms were:
- fatigue or weakness, affecting 11.3% of those with COVID-19 and 20% of those with MIS-C;
- shortness of breath (9.2% and 2.5%, respectively);
- cough (9.2% and 2.5%);
- headache (8.4% and 7.5%);
- muscle and body aches (5% and 3.1%); and
- fever (2.5% and 0.6%).
Activity impairment was somewhat more common after MIS-C (affecting 21.3%) than after acute COVID-19 (14.3%). According to caregiver reports:
- 6.7% of the COVID-19 group and 14.4% of the MIS-C group experienced difficulties with walking or exercise;
- 6.7% and 7.5%, respectively, were sleeping much more than usual; and
- 4.2% and 3.8%, respectively, had difficulty completing schoolwork or felt distracted and unable to focus.
Three factors predicted an increased risk for a prolonged recovery or activity impairment:
- more organ system involvement in patients with acute COVID-19;
- underlying respiratory conditions (usually asthma) in patients with MIS-C; and
- obesity in patients with MIS-C.
Dr. Randolph noted that this study was limited to children and adolescents who needed to be admitted to the hospital, and that it took place early in the pandemic; most were admitted before the delta surge, but they are looking at later periods.
Neurologic Complications Common in Children Hospitalized With COVID-19
Physicians at Monroe Carell Jr. Children’s Hospital at Vanderbilt found neurologic complications among children hospitalized with COVID-19 (Pediatrics 2022 Aug 11. doi:10.1542/peds.2022-058167).
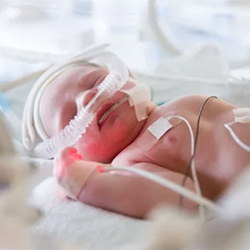
“We determined that neurologic complications are relatively common, occurring in about 8% of children hospitalized with COVID-19,” said James Antoon, MD, PhD, MPH, an assistant professor of pediatrics at Monroe Carell, in Nashville, Tenn. “The complications are almost uniformly associated with worse outcomes and can be life-altering conditions.”
The researchers looked at pediatric admissions at 52 children’s hospitals over a two-year period. Dr. Antoon and colleagues noted that when the omicron variant first emerged, cases of neurologic complications in children were reported, but most of the understanding of the complications was derived from adult studies.
This recent analysis of children between 2 months and 18 years of age showed that neurologic complications—defined as encephalopathy, encephalitis, aseptic meningitis, febrile seizure, nonfebrile seizure, brain abscess and bacterial meningitis, Reye’s syndrome, and cerebral infarction—were associated with an increased risk for ICU admission, readmissions, in-hospital mortality and increased hospital costs compared with hospitalizations without neurologic complications.
As of April 2022, more than 13 million cases of COVID-19 were reported in children and adolescents in the United States, according to the study.
“As we found in our study, COVID-related complications can have a significant impact on the lives of children,” Dr. Antoon said. “With the emergence of new, highly contagious variants, the potential patients that are at risk is growing.
“Our findings emphasize the importance of vaccination and prevention of COVID-19 in children in order to prevent these potentially life-threatening complications.”
Children With Mild COVID-19 Can Still Develop Long COVID
A new study found that children infected with COVID-19, but not hospitalized, also can experience long-COVID symptoms up to three months past infection (Pediatri Infect Dis J 2022 Aug 2. doi:10.1097/INF.0000000000003653).

The researchers examined data from volunteers across the state of Texas between the ages of 5 and 18 years who were enrolled in the Texas CARES survey, which began in October 2020 with the goal of assessing COVID-19 antibody status over time among a population of adults and children in Texas.
Data were collected before and after the vaccine rollout and during the waves of the delta and omicron variants.
“We were interested in understanding if children impacted with an acute or severe infection of COVID-19 would go on to have persisting symptoms, or what we call long COVID,” said Sarah Messiah, PhD, MPH, a professor of epidemiology, human genetics and environmental sciences and the director of the Center for Pediatric Population Health at UTHealth School of Public Health in Dallas. “This particular study is unique as the first population-based study in literature to report on prevalence of long COVID in children who have not been hospitalized with COVID-19.”
A total of 82 pediatric volunteers (4.8% of the total 1,813) reported having long-COVID symptoms: 1.5% showed symptoms that lasted between four and 12 weeks, including loss of taste and smell, fatigue, and cough. An additional 3.3% reported that symptoms such as loss of taste and smell, cough, and difficulty breathing persisted for longer than 12 weeks.
“From this information we wanted to know, ‘What would put a child more at risk for long COVID, and who is more susceptible to this?’ When we looked at risk factors of those who reported symptoms past 12 weeks, we found that children who were unvaccinated and who had obesity had a higher chance of developing long COVID. These findings are consistent with other literature that found children and adults who have comorbid health conditions and are unvaccinated are at a higher risk of being hospitalized for the virus,” Dr. Messiah said.
The researchers also found that children infected with COVID-19 before the emergence of the delta variant were more at risk for developing long COVID. “If you had COVID-19 earlier in the pandemic, you were more at risk for longer symptoms. With delta and omicron, we did see a lot of children who ended up hospitalized, but their symptoms were less severe, and our results show they were also less likely to report persistent symptoms, too,” Dr. Messiah said.
“There may be a perception that one needs to be hospitalized to have long COVID, and that is not what we found. I encourage parents to still take caution and get their child vaccinated against COVID-19, because we now know that it will decrease the risk of infection and long COVID,” she said.
COVID-19 mRNA Vaccines Safe in Pregnancy
COVID-19 messenger RNA (mRNA) vaccines are safe to use in pregnancy, and pregnant women experienced lower rates of health events after vaccination than similarly aged, nonpregnant vaccinated people, according to a large Canadian study (Lancet Infect Dis 2022 Aug 11. https://doi.org/10.1016/S1473-3099(22)00426-1).
The pandemic has disproportionately affected pregnant women, who are at higher risk for severe COVID-19 disease compared with similarly aged nonpregnant individuals, and many countries recommend COVID-19 vaccines for pregnant women.

“In the early stages of the COVID-19 vaccine rollout, there was low vaccine uptake among pregnant people due to concerns about data availability and vaccine safety. There still is lower-than-average uptake among nonpregnant women of reproductive age,” said Manish Sadarangani, PhD, MS, from the BC Children’s Hospital Research Institute, in Vancouver, and first author on this study.
The Canadian National Vaccine Safety Network examined data from participants across seven Canadian provinces and territories between December 2020 and November 2021. All vaccinated participants were asked to self-report any health events during the seven days following each dose of COVID-19 vaccine. The unvaccinated pregnant control group was asked to record any health problems over the seven days before they filled out the survey. In total, 191,360 women aged 15 to 49 years with known pregnancy status completed the first-dose survey and 94,937 completed the second-dose survey.
A significant health event was defined as a new or worse health event that caused the participant to miss school/work, require medical consultation and/or prevent daily activities in the previous seven days. A serious health event was defined as any event resulting in an emergency department visit and/or hospitalization in the previous seven days.
The researchers found that 4% (226/5,597) of mRNA-vaccinated pregnant women reported a significant health event within seven days after dose 1 of an mRNA vaccine, and 7.3% (227/3,108) after dose 2. The most common significant health events after dose 2 in pregnant women were a general feeling of being unwell, headache/migraine and respiratory tract infection.
In comparison, 3.2% (11/339) of pregnant unvaccinated participants reported similar events in the seven days prior to survey completion. In the vaccinated nonpregnant control group, 6.3% (10,950/174,765) reported a significant health event in the week after dose 1 and 11.3% (10,254/91,131) after dose 2. Serious health events were rare in all groups (<1%) and occurred at similar rates in vaccinated pregnant individuals, vaccinated nonpregnant people and unvaccinated controls after doses 1 and 2.
Miscarriage or stillbirth was reported by 2.1% (7/339) of unvaccinated pregnant women and 1.5% (83/5,597) of vaccinated pregnant women within seven days after dose 1 of any mRNA vaccine.
The authors caution that most participants who reported ethnicity in this study were white, and these data may therefore not be fully generalizable to other populations. In addition, this study focused on health events occurring within the first seven days following vaccination, and so cannot conclude anything about long-term reactions.
COVID-19 Associated With Increased Risk for Adverse Events Among Pregnant Women
COVID-19 infection in pregnant women is associated with an increased risk for cardiovascular adverse outcomes compared with women who are not pregnant (JACC Adv2022 Aug 10. doi:10.1016/j.jacadv.2022.100057).

Cardiovascular complications include myocardial infarctions, arrythmias, heart failure and long-COVID symptoms that may be difficult to distinguish from other cardiac complications of pregnancy and require the cardiovascular care team to be vigilant when assessing pregnant women with COVID-19.
According to the authors, there is an increased risk for cardiovascular complications in pregnant women compared with other groups because of the low vaccination rate in this population. In a recent study of more than 130,000 pregnant people, over three-fourths of those requiring hospital admission, most requiring critical care and all fetal deaths occurred in unvaccinated compared with vaccinated women.
The management of cardiac complications and diagnosis in pregnant COVID-19 patients can be challenging, given the overlap of COVID-19 symptoms, cardiovascular disease and pregnancy. According to the authors, imaging findings and timing of presentation may be helpful in differentiation and determining diagnosis. Clinicians also may need to adjust medical therapy during pregnancy and lactation.
The authors suggest management of cardiac complications in pregnant COVID-19 patients requires the creation of a “Pregnancy Heart Team” to optimize care, which may include providers comfortable with high-risk pregnancy, obstetric anesthesia, cardiology, critical care and neonatal care, depending on the nature of the complication, stage of pregnancy and severity of infection.
“Recognition of cardiovascular complication is hampered by failure to include pregnant women in clinical trials despite calls for inclusion of pregnant populations,” said Joan Briller, MD, a cardiologist and professor of clinical obstetrics and gynecology at the University of Illinois Chicago.
“Consequently, women may be undertreated or inadequately treated due to a lack of studies addressing safety and efficacy of therapies during pregnancy, or conversely be exposed to therapies where safety is not known.”
The CDC found pregnant women are at an increased risk for other adverse outcomes with COVID-19, including severe infection (10%), ICU admission (4%), mechanical ventilation (3%) and use of extracorporeal membrane oxygenation hemodynamic support (0.2%), compared with nonpregnant women of reproductive age. They are at higher risk for pre-term birth and stillbirth, and more than 33% of infants born to patients with COVID-19 were admitted to the neonatal ICU. In addition, pregnant patients who were older, overweight or had other preexisting conditions—such as chronic hypertension, preeclampsia and preexisting diabetes—were at even higher risk for severe infection.
A U.S.-specific study found substantial racial disparities in these outcomes. While non-Hispanic Black women accounted for 14.1% of the study cohort, they represented 26.5% of pregnancy-associated deaths. Pregnancy was associated with a 2.4 times risk for death in Hispanic women with COVID-19, and pregnant Asian and Native Hawaiian/Pacific Islanders were among those at the highest risk for ICU admissions.
“Pregnant people need to know that they are increased risk of a severe COVID-19 infection, including ICU admissions, cardiac complications, need for critical care and death for the patient or fetus. Unfortunately, pregnant women have lagged behind other groups getting vaccinated,” Dr. Briller said.
{RELATED-HORIZONTAL}