Vaccination remains one of public health’s greatest achievements, dramatically reducing mortality and morbidity from infectious diseases.1 However, those gains are attributable to the high coverage rates of vaccines. When uptake declines—because of hesitancy, access barriers, or misinformation—vaccine-preventable diseases (VPDs) reemerge, as recent US data starkly illustrate. In 2025, the United States already has reported more measles cases than in any year since prior to the disease being declared eliminated in 2000.2 As of September 16, there were 1,491 confirmed cases from 38 separate outbreaks in 42 states and cities.2 Varicella clusters have resurfaced in under-vaccinated communities. Pertussis cases reached 35,000 in 2024,3 and infant deaths are continuing into 2025. Given that the routine schedule now protects against more than 20 pathogens, clinicians need a framework for anticipating which VPDs are most likely to rebound—and why.
The likelihood of a VPD’s resurgence depends on pathogen characteristics, the nature of the vaccine, and host factors. On the pathogen side, communicability plays a central role. Measles, for example, has an R0 (basic reproduction number, the average number of people an infected person will spread the disease to in a completely susceptible population) between 12 and 18,4 meaning a single infected individual can infect up to 18 susceptible people. Endemicity matters as well: Varicella-zoster virus is still present in the community because it is latent in people previously infected and can reactivate as shingles, constantly reintroducing the pathogen to the population. Small decreases in vaccination can easily lead to outbreaks of disease. However, diphtheria no longer circulates in the United States, making outbreaks dependent on importation into an unvaccinated community. Strain and serotype variation is another key issue. Influenza vaccines must be reformulated annually to match circulating strains, and protection may be decreased if the match is poor.5 With more than 100 known serotypes of pneumococcus, pneumococcal vaccines target specific serotypes that cause invasive disease, but nonvaccine serotypes can still cause illness and fill the ecological niche left behind with the reduction of vaccine-preventable serotypes.6
Vaccine characteristics also influence disease patterns and the likelihood of outbreaks. Some vaccines, such as the Haemophilus influenzae type b (Hib) vaccine, prevent both colonization and infection.7 This limits the reservoir of bacteria in a community, effectively cutting off transmission even if vaccination rates decline. Other vaccines, such as acellular pertussis vaccines, may permit colonization8 while still reducing symptomatic disease. In that case, a vaccinated person may not get sick but can pass the bacteria on to a susceptible person and cause illness. Vaccines for many respiratory infections primarily prevent severe disease but do not produce mucosal immunity, allowing mild infection to occur. The durability of immunity is another consideration. Two doses of measles vaccine typically provides lifelong protection, while immunity from acellular pertussis vaccines wanes within a few years, requiring adherence to booster schedules to keep the population protected.
Host behavior and susceptibility add further complexity. Unvaccinated individuals may be vulnerable for different reasons. Some may be undergoing chemotherapy or have other medical contraindications and are often highly cautious, reducing their time in crowds and/or requiring face masks. Others may remain unvaccinated by choice and engage in social behaviors that increase transmission risk, leading to clustering of infections in communities with similarly low vaccination coverage. Finally, certain populations, such as young infants or older adults, may be at risk for more severe disease just by nature of effectiveness of their immune system.
Considering all these factors, it is prudent for clinicians to consider how disease manifestations may increase or change in an era of decreasing vaccination rates.
From Mild to Wild
Clinicians who are comfortable treating mild cases of respiratory illness due to COVID-19, respiratory syncytial virus, and influenza viruses may see an increase in more severe cases as more people are unvaccinated. Although these viruses are quite different biologically and use different vaccine platforms, their vaccines share a common goal: to prevent emergency department visits, hospitalizations, and deaths. There is no mechanism for eliminating circulation of viruses in the population altogether. Because of their short incubation periods, people who have been vaccinated may be infected and have early mild symptoms but then mount a quick immune response that mitigates symptoms. However, without vaccination, these same infections can progress from mild to severe, and clinicians will see a corresponding rise in acute care utilization, followed by increases in hospitalizations and mortality.
Sporadic Outbreaks Likely to Increase
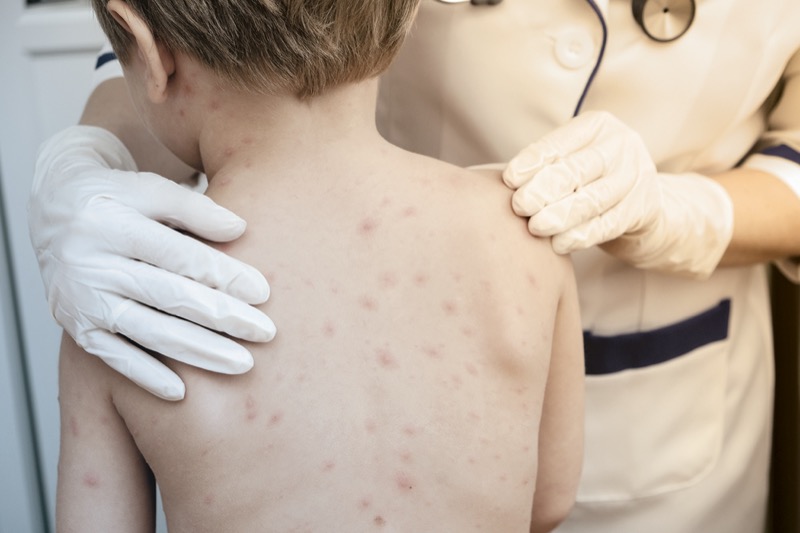
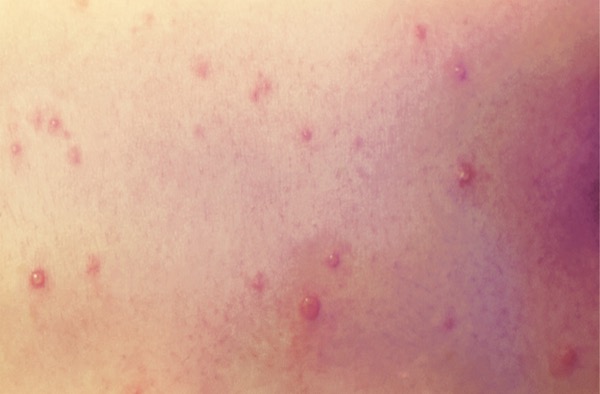
Certain diseases are likely to reappear in sporadic outbreaks when vaccination coverage drops. Varicella, the virus that causes chickenpox, remains present in the community because the virus establishes latency in people and can later reactivate as shingles, maintaining a reservoir in the human population.9 The illness presents first with a nonspecific prodrome of fever and fatigue, followed by a characteristic rash 1 or 2 days later. The rash usually begins on the chest, back, and face, and then spreads to the rest of the body. The itchy rash contains vesicles on a red base that then crust, often described as “dewdrops on a rose petal,” in varying stages of development. Patients can have 250 to 500 lesions (Image 1). Breakthrough cases in vaccinated individuals tend to be mild, with fewer lesions that may not have the characteristic vesicular appearance.
The current 2-dose varicella vaccine, which is a live-attenuated virus, is highly effective, but outbreaks will occur in under-vaccinated communities.9 Whether varicella manifests as primary chickenpox, breakthrough disease in the vaccinated, or shingles in someone previously infected, the virus remains transmissible, particularly to immunocompromised individuals, pregnant people, and unvaccinated adolescents and adults.
Pertussis is another persistent infection in the community. Pertussis begins with a catarrhal phase resembling the common cold, followed by a paroxysmal phase characterized by intense coughing fits, post-tussive vomiting, and the classic “whoop” sound; infants may instead present with apnea. The convalescent phase involves gradual symptom resolution over weeks to months. Older children and adults may experience prolonged coughing, pneumonia, and fatigue, whereas infants are at risk for seizures, encephalopathy, and death.
Although acellular DTaP (diphtheria, tetanus, acellular pertussis) and Tdap (tetanus, diphtheria, acellular pertussis) vaccines reduce disease severity, they do not prevent colonization or transmission as effectively as earlier whole-cell vaccines. Additionally, immunity wanes. The combination of waning immunity; decreasing rates in vaccination of pregnant people, infants, and those eligible for boosters; persistent colonization; and the high R0 of 12 to 17, has led to ongoing outbreaks that are likely to increase.8 Young infants will be at highest risk for disease and severe complications. In 2024, there were 10 pertussis-related deaths in the United States, 6 of them in infants younger than 12 months of age.3 In 2025, this trend continues, with infant hospitalizations and deaths continuing to occur.10
Mumps outbreaks will continue to increase with decreased measles, mumps, and rubella vaccination rates. Parotitis is the hallmark of mumps, although complications like orchitis, meningitis, and sensorineural hearing loss can occur. Outbreaks are more common in close-contact environments such as college campuses.11
In particular, the mumps vaccine, which is a live-attenuated virus vaccine, does not convey lifelong immunity. This means that just at a time when older teens congregate in college settings and social situations, their mumps immunity is waning, making outbreaks in this age group common. As with pertussis and varicella, mumps outbreaks will be highly sensitive to vaccination rates.
Hepatitis A, a fecal–oral transmitted virus, leads to malaise, jaundice, abdominal pain, and dark urine. While the illness is self-limited in most, fulminant hepatitis can occur, particularly in those with preexisting liver disease.
The inactivated vaccine for hepatitis A is highly effective, with 2 doses providing close to 100% protection. Hepatitis A has resurged in populations with declining vaccine uptake and poor sanitation, as well as with exposure to contaminated food. People experiencing insecure housing and those who use drugs are at risk due to poor hygiene.
Rotavirus, a leading cause of severe diarrhea in infants and young children, can cause dehydration, hospitalization, and even death in severe cases. This live-attenuated vaccine is highly effective in preventing hospitalization, but the virus continues to circulate in the population. Communities with low vaccine uptake may again experience seasonal peaks leading to pediatric hospitalizations within a few years.
Sustained at Low Levels
Vaccines for bacteria including Streptococcus pneumoniae, Hib, and Neisseria meningitidis follow another trajectory. These pathogens circulate at low levels, and vaccines are highly effective at the individual level. Infections will increase gradually as coverage declines.
Pneumococcus causes a wide range of illness, from otitis media to life-threatening conditions like pneumonia, bacteremia, and meningitis. Clinical presentation depends on the site of infection, and diagnosis is made through culture or polymerase chain reaction testing of blood, cerebrospinal fluid, or other sterile sites. Prompt antibiotic treatment is critical, and long-term complications may include hearing loss, neurologic impairment, or death, particularly following meningitis.
Pneumococcal conjugate vaccines reduce colonization of vaccine-targeted strains, which in turn decreases disease incidence in both vaccinated and unvaccinated individuals.12 This effect was first observed in older adults after the introduction of pediatric pneumococcal vaccination. As vaccination rates decline, disease will rise in young children. If adults also limit their degree of vaccination, their risk will also increase.
Hib similarly can cause a spectrum of illness. Before widespread vaccination, Hib was a leading cause of invasive bacterial infections in children, including meningitis, epiglottitis, pneumonia, and septic arthritis. Epiglottitis can progress rapidly and cause airway obstruction, making it a feared presentation in emergency settings. Survivors of Hib meningitis may suffer long-term sequelae such as hearing loss and cognitive delays.
Hib vaccines are remarkably effective at reducing both colonization and disease.7 A significant decline in vaccination could allow Hib to reestablish itself within a few years, especially in communities with lower vaccination rates.
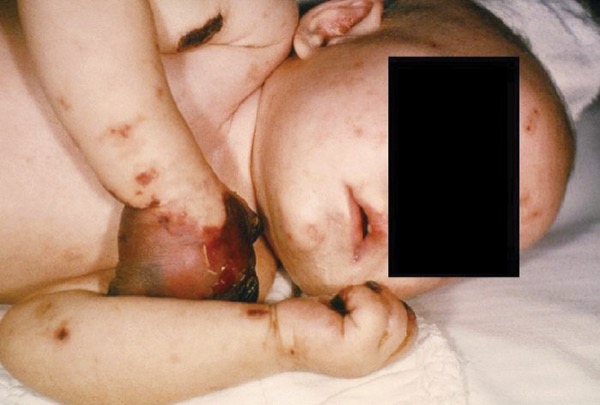
N. meningitidis can cause rapidly progressing and often fatal infections, including meningitis and meningococcemia. Meningitis typically presents with fever, headache, neck stiffness, and photophobia, while meningococcemia can lead to purpura, hypotension, and multi-organ failure (Image 2). The disease can be fatal within hours. Adolescents and young adults are particularly vulnerable, especially in close-contact settings such as college dormitories and military barracks.
Vaccination with quadrivalent (disease caused by serogroups A, C, W, and Y) and serogroup B vaccines is effective and particularly important in high-risk populations. Because the disease is rare, with approximately 500 cases reported in 2024,13 a broad decline in adolescent vaccine uptake may not immediately result in widespread outbreaks, but the risk for localized outbreaks increases substantially, particularly if lower vaccination rates occur in close-contact settings.
Tetanus remains incredibly rare, likely because those unvaccinated can vaccinate after an injury. Caused by a toxin from Clostridium tetani, which is present in the environment, tetanus is not spread from person to person. The disease begins with muscle rigidity and spasms, often starting with lockjaw and progressing to generalized spasms and autonomic instability. It can be fatal, especially in neonates and older adults. Diagnosis is clinical, and treatment includes wound care, immune globulin, and intensive supportive care.
Cases arise from individual failures to vaccinate rather than from community transmission. Routine DTaP or Tdap vaccination and booster doses with the toxoid vaccine are essential to prevent cases. Additionally, the use of vaccination after an injury likely contaminated with dirt, such as stepping on a nail or outdoor crush injuries, is highly effective.14
Gone, but Not Forgotten
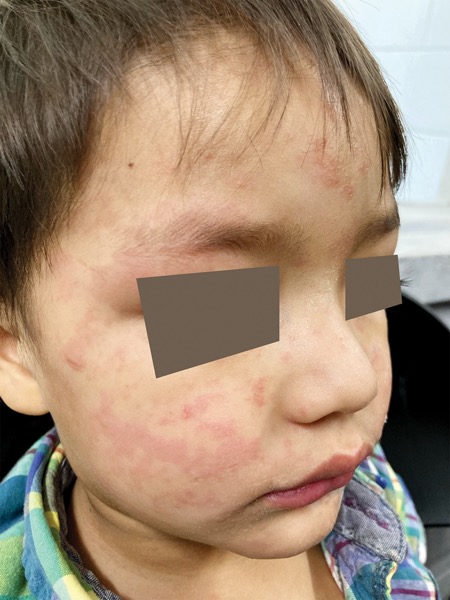
Finally, 4 diseases that have been eliminated in the United States—measles, rubella, polio, and diphtheria—will remain threats if vaccination coverage falls.15 Measles, with its extraordinarily high R0, can rapidly spread after a single importation. The virus causes high fever, cough, coryza, conjunctivitis, and a descending maculopapular rash that may become raised; it starts at the hairline and moves down the body, disappearing in the same order in which it appeared (Image 3). Measles is feared due to the frequency with which it causes dehydration, pneumonia, encephalitis, and death in up to 1 in 1,000 people infected. It also causes an immune amnesia, leading to increased vulnerability to other infections. Subacute sclerosing panencephalitis, a fatal degenerative neurologic condition, can occur years after measles infection.
Despite elimination, outbreaks have occurred in 2025 due to declining coverage, both in the United States and abroad.16 The measles vaccine, a live-attenuated viral vaccine, is highly effective. Two doses of vaccine provide 97% protection, which is lifelong. However, the contagiousness of the virus means 95% of people need to be fully vaccinated to prevent spread. Measles outbreaks are the first sign of the return of VPDs.
Polio is caused by 3 types of poliovirus. Although 2 of the 3 wild types have been eradicated, 1 remains. Additionally, vaccine-derived polioviruses exist as mutated forms of the oral poliovirus vaccine. Once a feared cause of paralysis and death, polio has been eliminated in the United States since 1979 (Image 4). The virus is highly contagious. Although many infected have no symptoms, some will have minor symptoms like sore throat, fever, tiredness, stomach pain, vomiting, or constipation. A small number develop meningitis, while an even smaller number develop paralytic polio. A clinically apparent case of polio (either vaccine derived or wild type) in a community indicates a likely larger reservoir of virus leading to asymptomatic infection, as was seen in New York in 2022. While only 1 case presented to medical care, wastewater sampling indicated more covert spread.17
The vaccine now used in the United States to prevent polio is an inactivated vaccine. This protects people from paralytic disease, but the virus can still live and reproduce in the intestines. Polio vaccination across the globe remains critical to preventing resurgence, and vigilance is needed to detect cases.
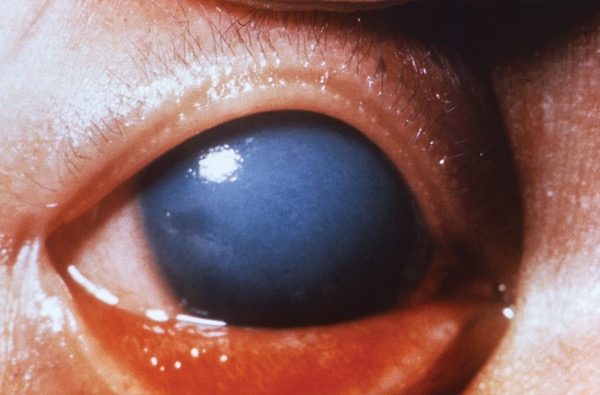
Rubella, also known as German measles, causes a mild febrile illness and rash in children. It is devastating when contracted during pregnancy, leading to congenital rubella syndrome. Birth defects include deafness, cataracts, and heart defects (Image 5). The rubella vaccine is 97% effective against rubella. Elimination was achieved in 2004. To see this disease return, there would need to be immunity gaps as well as reintroduction from international travel.
Diphtheria, caused by Corynebacterium diphtheriae, produces a thick pseudomembrane in the throat that can obstruct breathing. Although respiratory diphtheria was last confirmed in 2003 in the United States, it remains endemic in other parts of the world. An imported case in an under-vaccinated community could lead to rapid spread and severe outcomes. This, too, would be exceedingly rare.
Cancer Prevention
Two vaccines also provide long-term cancer prevention: HPV and hepatitis B (HepB). The HPV vaccine protects against strains that cause cervical, anal, and oropharyngeal cancers. The HepB vaccine prevents chronic liver infection that can progress to cirrhosis and hepatocellular carcinoma. Decreasing rates of these vaccines will not immediately manifest as increased rates of diseases, but are crucial for long-term public health.
Conclusion
The resurgence of measles, chickenpox, and pertussis—even in communities with historically high vaccine uptake—illustrates how quickly progress can unravel. Other pathogens, such as rotavirus and mumps, loom as threats if we allow immunity to decline. Maintaining high coverage of vaccines in primary series, as well as adhering to booster guidance and maternal vaccination guidance during pregnancy, are needed to keep tight control of these contagious pathogens. Vaccines are not “set it and forget it” tools. We can prevent the return of diseases that vaccines have made rare—or eliminated entirely—only through sustained collective action.
References
- Talbird SE, Carrico J, La EM, et al. Impact of routine childhood immunization in reducing vaccine-preventable diseases in the United States. Pediatrics. 2022;150(3):e2021056013.
- Measles cases and outbreaks. CDC. Published September 17, 2025. Accessed September 17, 2025. cdc.gov/measles/data-research/index.html
- 2024 Provisional Pertussis Surveillance Report. CDC. Published January 2025. Accessed July 8, 2025. cdc.gov/pertussis/media/pdfs/2025/01/pertuss-surv-report-2024_PROVISIONAL-508.pdf
- Guerra FM, Bolotin S, Lim G, et al. The basic reproduction number (R0) of measles: a systematic review. Lancet Infect Dis. 2017;17(12):e420-e428.
- Tricco AC, Chit A, Soobiah C, et al. Comparing influenza vaccine efficacy against mismatched and matched strains: a systematic review and meta-analysis. BMC Med. 2013;11:153.
- Hanquet G, Krizova P, Dalby T, et al. Serotype replacement after introduction of 10-valent and 13-valent pneumococcal conjugate vaccines in 10 countries, Europe. Emerg Infect Dis. 2022;28(1):137-138.
- Barbour ML, Mayon-White RT, Coles C, et al. The impact of conjugate vaccine on carriage of Haemophilus influenzae type B. J Infect Dis. 1995;171(1):93-98.
- Burdin N, Handy LK, Plotkin SA. What is wrong with pertussis vaccine immunity? The problem of waning effectiveness of pertussis vaccines. Cold Spring Harb Perspect Biol. 2017;9(12):a029454.
- Marin M, Seward JF, Gershon AA. 25 Years of varicella vaccination in the United States. J Infect Dis. 2022;226(suppl 4):S375-S379.
- Pan American Health Organization. Epidemiological alert: increased pertussis (whooping cough) in the Americas Region. Published May 31, 2025. Accessed September 2, 2025. paho.org/sites/default/files/2025-05/2025-05-31-epi-alert-pertussis-whooping-cough-final.pdf
- Melgar M, Yockey B, Marlow MA. Impact of vaccine effectiveness and coverage on preventing large mumps outbreaks on college campuses: implications for vaccination strategy. Epidemics. 2022;40:100594.
- Shiri T, Datta S, Madan J, et al. Indirect effects of childhood pneumococcal conjugate vaccination on invasive pneumococcal disease: a systematic review and meta-analysis. Lancet Glob Health. 2017;5(1):e51-e59.
- Meningococcal disease surveillance and trends. CDC. Published May 9, 2025. Accessed September 2, 2025. cdc.gov/meningococcal/php/surveillance/index.html
- Hammarlund E, Thomas A, Poore EA, et al. Durability of vaccine-induced immunity against tetanus and diphtheria toxins: a cross-sectional analysis. Clin Infect Dis. 2016;62(9):1111-1118.
- Kiang MV, Bubar KM, Maldonado Y, et al. Modeling reemergence of vaccine-eliminated infectious diseases under declining vaccination in the US. JAMA. 2025;333(24):2176-2187.
- Do LAH, Mulholland K. Measles 2025. N Engl J Med. Published online June 25, 2025. doi:10.1056/nejmra2504516
- Ryerson AB, Lang D, Alazawi MA, et al. Wastewater testing and detection of poliovirus type 2 genetically linked to virus isolated from a paralytic polio case — New York, March 9–October 11, 2022. MMWR Morb Mortal Wkly Rep. 2022;71(44):1418-1424.
Copyright © 2025 McMahon Publishing, 545 West 45th Street, New York, NY 10036. Printed in the USA. All rights reserved, including the right of reproduction, in whole or in part, in any form.

Download to read this article in PDF document:![]() Vaccine-Preventable Diseases Make a Comeback
Vaccine-Preventable Diseases Make a Comeback