Molecular rapid diagnostic tests (RDTs) have fundamentally transformed the diagnosis and management of common infectious diseases by providing rapid and accurate pathogen detection. Molecular testing is becoming a common adjunct to routine microbiological testing methods across a variety of patient care areas beyond large academic tertiary care centers. Additionally, clinical metagenomics increasingly are used to aid in diagnosis when traditional methods are unsuccessful.1 With this rapid and widespread availability, our understanding of how to best leverage these tools to improve patient outcomes is being outpaced by technology.
Prior to widespread adoption, there needs to be an understanding of the strengths and weaknesses of these tools, particularly when applied to specific patient populations for whom they are intended.2,3 For example, newer technologies can assist in empiric antimicrobial therapy selection but must be taken in context with local infectious diseases epidemiology.4 In addition, implementation of commercially available multiplex RDTs can result in significantly decreased time to organism identification, but also antimicrobial overuse if implemented without supporting antimicrobial stewardship (AMS) infrastructure, such as treatment algorithms or prospective audit and feedback.5 As has been demonstrated with molecular RDTs (mRDTs) for bloodstream infections (BSIs), AMS programs can have a significant and profound impact on how these tools are leveraged to improve patient outcomes.6 Antimicrobial stewardship programs should work closely with their clinical microbiology colleagues to ensure that implementation of new mRDTs across a hospital or health system is performed in a way that optimizes diagnostic and antimicrobial decisions and prompts providers to order the right test, for the right patient, leading to the right action.3,7 Due to the complexity of interventions with mRDTs, RDT development and implementation must be coupled with multifaceted AMS interventions, such as education, to facilitate informed decision making, system-based interventions to guide appropriate ordering of these diagnostic tests, and institution-specific antimicrobial treatment recommendations and considerations for real-time monitoring and feedback.8,9
RDTs combined with AMS intervention, particularly for BSIs and rapid testing for broad panels of respiratory viruses, have been deemed important AMS interventions to optimize antimicrobial use and patient outcomes.10 We should be mindful that evaluations of the clinical efficacy of mRDTs beyond BSIs are still evolving as we discuss novel mRDTs, including advances in rapid phenotypic testing, syndromic molecular testing for respiratory infections, gastrointestinal (GI) infections, and meningitis/encephalitis, as well as prospects of outpatient point of care, and their performance with current diagnostic stewardship practices.
Bloodstream Infections
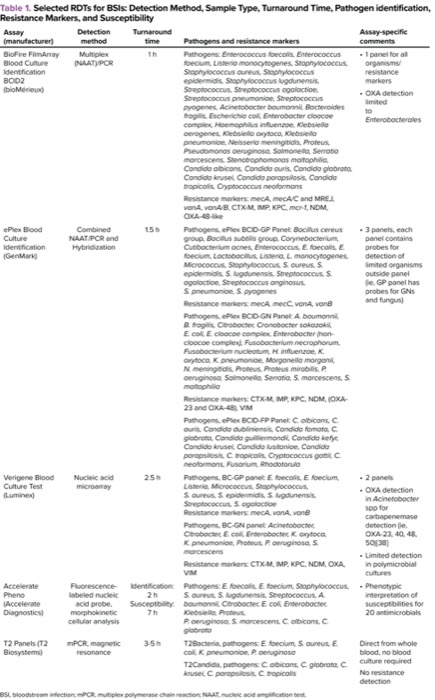
How we diagnose and manage BSIs has been fundamentally changed by mRDTs, which provide actionable information about organism identification and resistance mechanisms much earlier in the diagnostic course. Table 1 shows available blood RDTs with respect to detection method, sample type required, turnaround time, pathogen identification, resistance gene detection, and susceptibility testing. Matrix-assisted laser desorption/ionization time of flight (MALDI-TOF) (eg, bioMérieux, BD Bruker), polymerase chain reaction (PCR)-based technologies (eg, BioFire Film-Array BCID, GenMark ePlex BCID), and nanoparticle probe technology (eg, Verigene BC-GP & BC-GN) have all been associated with decreases in time to effective therapy.8,11 When paired with AMS interventions such as review of mRDT results and feedback to primary management teams, use of these tools has also been associated with reduced hospital length of stay (LOS) and mortality.6
| Table 1. Selected RDTs for BSIs: Detection Method, Sample Type, Turnaround Time, Pathogen identification, Resistance Markers, and Susceptibility | ||||
| Assay (manufacturer) | Detection method | Turnaround time | Pathogens and resistance markers | Assay-specific comments |
|---|---|---|---|---|
| BioFire FilmArray Blood Culture Identification BCID2 (bioMérieux) | Multiplex (NAAT)/PCR | 1 h | Pathogens: Enterococcus faecalis, Enterococcus faecium, Listeria monocytogenes, Staphylococcus, Staphylococcus aureus, Staphylococcus epidermidis, Staphylococcus lugdunensis, Streptococcus, Streptococcus agalactiae, Streptococcus pneumoniae, Streptococcus pyogenes, Acinetobacter baumannii, Bacteroides fragilis, Escherichia coli, Enterobacter cloacae complex, Haemophilus influenzae, Klebsiella aerogenes, Klebsiella oxytoca, Klebsiella pneumoniae, Neisseria meningitidis, Proteus, Pseudomonas aeruginosa, Salmonella, Serratia marcescens, Stenotrophomonas maltophilia, Candida albicans, Candida auris, Candida glabrata, Candida krusei, Candida parapsilosis, Candida tropicalis, Cryptococcus neoformans Resistance markers: mecA, mecA/C and MREJ, vanA, vanA/B, CTX-M, IMP, KPC, mcr-1, NDM, OXA-48-like |
|
| ePlex Blood Culture Identification (GenMark) | Combined NAAT/PCR and Hybridization | 1.5 h | Pathogens, ePlex BCID-GP Panel: Bacillus cereus group, Bacillus subtilis group, Corynebacterium, Cutibacterium acnes, Enterococcus, E. faecalis, E. faecium, Lactobacillus, Listeria, L. monocytogenes, Micrococcus, Staphylococcus, S. aureus, S. epidermidis, S. lugdunensis, Streptococcus, S. agalactiae, Streptococcus anginosus, S. pneumoniae, S. pyogenes Resistance markers: mecA, mecC, vanA, vanB Pathogens, ePlex BCID-GN Panel: A. baumannii, B. fragilis, Citrobacter, Cronobacter sakazakii, E. coli, E. cloacae complex, Enterobacter (non-cloacae complex), Fusobacterium necrophorum, Fusobacterium nucleatum, H. influenzae, K. oxytoca, K. pneumoniae, Morganella morganii, N. meningitidis, Proteus, Proteus mirabilis, P. aeruginosa, Salmonella, Serratia, S. marcescens, S. maltophilia Resistance markers: CTX-M, IMP, KPC, NDM, (OXA-23 and OXA-48), VIM Pathogens, ePlex BCID-FP Panel: C. albicans, C. auris, Candida dubliniensis, Candida famata, C. glabrata, Candida guilliermondii, Candida kefyr, Candida krusei, Candida lusitaniae, Candida parapsilosis, C. tropicalis, Cryptococcus gattii, C. neoformans, Fusarium, Rhodotorula |
|
| Verigene Blood Culture Test (Luminex) | Nucleic acid microarray | 2.5 h | Pathogens, BC-GP panel: E. faecalis, E. faecium, Listeria, Micrococcus, Staphylococcus, S. aureus, S. epidermidis, S. lugdunensis, Streptococcus, S. agalactiae Resistance markers: mecA, vanA, vanB Pathogens, BC-GN panel: Acinetobacter, Citrobacter, E. coli, Enterobacter, K. oxytoca, K. pneumoniae, Proteus, P. aeruginosa, S. marcescens Resistance markers: CTX-M, IMP, KPC, NDM, OXA, VIM |
|
| Accelerate Pheno (Accelerate Diagnostics) | Fluorescence-labeled nucleic acid probe, morphokinetic cellular analysis | Identification: 2 h Susceptibility: 7 h | Pathogens: E. faecalis, E. faecium, Staphylococcus, S. aureus, S. lugdunensis, Streptococcus, A. baumannii, Citrobacter, E. coli, Enterobacter, Klebsiella, Proteus, P. aeruginosa, S. marcescens, C. albicans, C. glabrata |
|
| T2 Panels (T2 Biosystems) | mPCR, magnetic resonance | 3-5 h | T2Bacteria, pathogens: E. faecium, S. aureus, E. coli, K. pneumoniae, P. aeruginosa T2Candida, pathogens: C. albicans, C. glabrata, C. krusei, C. parapsilosis, C. tropicalis | Direct from whole blood, no blood culture required No resistance detection |
| BSI, bloodstream infection; mPCR, multiplex polymerase chain reaction; NAAT, nucleic acid amplification test. | ||||
These tools can also be cost-effective. Several studies have demonstrated that MALDI-TOF is cost-effective.12,13 In a cost-effectiveness analysis, the benefits of multiple mRDTs for BSIs have been observed.14 Of note, there is a strong synergism between AMS and RDTs, with RDTs having a reported 80% probability of cost-effectiveness with AMS involvement.
Recently, mRDT platforms have been compared on potential desirability of antimicrobial therapy decisions using the Desirability of Outcome Ranking Management of Antimicrobial Therapy (DOOR-MAT), which uses a theoretical framework combined with a partial credit scoring system.15-17 When compared in a proof-of-concept study at a single center, both Verigene BC and ePlex BCID had high positive-predictive value (PPV) for on-panel targets, but ePlex BCID was able to identify more organisms than Verigene BC, resulting in a higher mean DOOR-MAT score (91.9 [SD, 32.1] vs 86.8 [SD, 28.5]’ P=0.01), respectively.16 Similarly, Verigene BC-GN was compared with BioFire BCID and BCID2 among gram-negative BSIs.15 The mean DOOR-MAT score was higher for BioFire BCID2 than both BioFire BCID and Verigene BC-GN. The higher mean DOOR-MAT score for BioFire BCID2 was largely attributed to the expanded detection of panel organisms (compared with Verigene) and resistance determinants (compared with BCID). These findings highlight the importance of considerations of local infection epidemiology with RDT implementation.
The introduction of the Accelerate PhenoTest BC (Accelerate Diagnostics) represents new unique opportunities to improve the management of BSIs. This test uses a combination of fluorescence in situ hybridization (FISH) technology and morphokinetic cellular analysis to yield both organism identification in approximately 1.5 hours as well as phenotypic susceptibility profiles for selected antimicrobial agents.18 Compared with routine organism identification methods, overall sensitivity and specificity for the identification of organisms and essential agreement and categorical agreement for antimicrobial susceptibility were 95.6%, 99.5%, 95.1%, and 95.5%, respectively.19 Of note, the Accelerate PhenoTest BC lacks genetic resistance determination. An in vitro study of 40 Escherichia coli, Klebsiella pneumoniae, and Proteus mirabilis isolates examined the correlation between ceftriaxone nonsusceptibility and extended-spectrum beta-lactamase (ESBL) production.20 The ESBL-confirmatory disk test was positive in 84.6% (22/26) of ESBL-producing isolates and negative in 92.9% (13/14) of non–ESBL- and/or AmpC-producing isolates. This finding allows expedited phenotypic detection for potential optimization of antimicrobial regimens. Recently, a randomized controlled trial of patients with gram-negative BSIs combined with prospective audit and feedback demonstrated significantly shorter time to antimicrobial switch (8.6 vs 14.9 hours; P=0.02).11 Importantly, for patients with BSI with an organism demonstrating antimicrobial resistance, there was a median 43-hour decrease in antimicrobial escalation, and for those with susceptible organisms, a median decrease of 13 hours to deescalation. There have been several quasi-experimental studies that examined the impact of Accelerate Pheno BC with AMS intervention. They have demonstrated shorter times to antimicrobial therapy optimization, but variable results with respect to patient outcomes.
By detecting directly from whole blood, the T2Bacteria Panel (T2 Biosystems) has the potential to improve early initiation of appropriate antibiotic therapy in BSIs.21 This system works by pairing PCR technology with magnetic resonance (T2MR) and probe-enriched superparamagnetic nanoparticles. The clinical benefit of the T2Bacteria Panel, however, remains to be fully seen.22 The T2Bacteria Panel’s sensitivity and specificity, compared with a single set of blood cultures, was 90% (95% CI, 76%-96%) and 90% (95% CI, 88%-91%), respectively.23 The panel itself, however, is limited to only 5 bacteria: the ESKAPE pathogens (Enterococcus faecium, Staphylococcus aureus, K. pneumoniae, Pseudomonas aeruginosa, and E. coli). One challenge is discordance between T2 Panel results and those of traditional microbiological methods. A recent subgroup analysis from a prospective, multicenter clinical trial evaluated the significance of positive T2Bacteria cases when blood culture was negative to gain a better understanding of whether these results were false positives or potentially associated with an infection.24 In 233 participants, 20 patients were identified with 21 (9%) discordant results. Eleven (52.5%) cases had probable BSI, 4 (19%) had possible BSI, and 6 (28.5%) were presumptive false positives. Among the probable and possible BSIs, discrepancies appeared to be associated with closed space and localized infections and recent use of active antimicrobial agents. In terms of clinical outcomes, a recent retrospective cohort study of 49 patients with panel results determined that, compared with a matched sample of patients managed by traditional methods, there was less inappropriate empiric antimicrobial therapy (5.5% vs 38.8%) and lower 28-day mortality.25 A systematic review of 14 studies comparing T2MR with blood culture for the detection of bacterial and fungal BSI found that patients with positive panel results received targeted antimicrobial therapy faster (42 hours; P<0.001). Additionally, LOS in the ICU (mean difference, –5.0 days; P=0.03) and hospital stay (mean difference, –4.8 days; P=0.03) were shorter with T2MR, but mortality was similar (28.9% vs 29.9%; relative risk, 1.02; P=0.86).26
T2 Biosystems also produces the T2Candida Panel, which can assist in the diagnosis of candidemia by detecting 5 of the most common Candida species in approximately 5 hours.27 Candidemia is one of the most common hospital-acquired BSIs, associated with up to 40% crude mortality.28 As much as a 50% reduction in mortality has been associated with prompt initiation of appropriate antifungal therapy and source control. This, however, is often delayed due to blood culture insensitivity, prolonged turnaround time needed to yield growth, and possibility of negative growth with invasive abdominal candidiasis.29 Thus, clinicians are often faced with challenges of both overuse of unnecessary antifungal therapy and delays in appropriate empiric antifungal therapy. While sensitivity and specificity seem to be much more promising compared with blood cultures—91% and 99%, respectively—the role of the T2Candida Panel in the early diagnosis and management of candidemia remains unclear.30
In 4 retrospective, single-center cohort studies, the T2Candida Panel was evaluated with the combination of active ASM intervention in adults with suspected or proven candidemia.31-34 Time to appropriate therapy decreased in patients with proven candidemia, while shorter micafungin days on therapy (DOT) and cost savings were observed in patients without microbiological evidence of invasive candidiasis. However, antifungal discontinuation with negative tests was inconsistent, despite AMS intervention such as prospective audit and feedback being performed on negative results. Bomkamp et al found that overall antifungal DOT improved after implementation of the T2Candida Panel, but the use of micafungin continued to decline after the panel was removed, likely due to the increased AMS resources.33 In contrast, Steuber et al observed antifungal discontinuation with negative tests to be unexpectedly low even with pharmacist-driven prospective audit and feedback.32 The stewardship potential of the T2Candida Panel may be heavily contingent on the effectiveness of the AMS intervention because clinicians are particularly apprehensive about deescalation in patients already at substantially high risk for fungal infections.
The performance of the T2Candida Panel for detection of invasive candidiasis, such as Intraabdominal candidiasis (IAC), has also been assessed.35,36 Blood cultures remain the gold standard for invasive candidiasis but are typically sterile in more than 80% of patients with IAC.37 In 48 high-risk patients for IAC, the sensitivity, specificity, positive-predictive value, and negative-predictive value (NPV) of the T2Candida Panel relative to blood cultures were 33%, 93%, 71%, and 74%, respectively.35 IAC was present, diagnosed by intraabdominal culture, in 100% of cases with concordant positive T2Candida/1,3-beta-D-glucan, but absent in 90% of concordant negative results. In a study of 126 ICU patients at high risk for invasive candidiasis, investigators paired the T2Candida Panel with blood cultures and Candida mannan antigen (MAg) testing. The sensitivity of the panel versus all others (likely, possible, unlikely) was 55% and the specificity was 93% (compared with blood cultures with 45% and 100%, respectively). Combining all 3 testing modalities only improved sensitivity to 64%. Overall, there are limited data for the T2Candida panel for the detection of deep-seated infections such as IAC, and more robust studies are needed.
The Karius Test (Karius) offers a new tool in the AMS armamentarium. This test performs metagenomic next-generation sequencing (mNGS) using microbial cell-free DNA in plasma, which can identify 1,250 bacteria, fungi, parasites, and viruses.40,41 It offers a noninvasive method for detecting infections from a variety of sources and patient populations, including those who are immunocompromised. It has the potential to aid in identifying etiologies for infections even after antimicrobials have been initiated. Its role may be useful in immunocompromised hosts for the diagnosis of invasive mold infections (IMI). Recently a budget impact analysis of performing the Karius Test, instead of more invasive procedures, in patients with suspected IMI postulated a cost savings of $2,277 per patient.42 The clinical effectiveness of this tool needs to be explored further. In a single-center cohort of 80 adult patients in whom the Karius Test was performed, the most common reason for the test was unknown microbiological diagnosis (78%), with avoiding invasive procedures only accounting for 14% of indications.43 The test has a positive impact on 43% of cases, primarily in those who were immunocompromised or received antimicrobials for less than 7 days. Positive impact was primarily driven by antimicrobial deescalation.
Lower Respiratory Tract Infections
In the United States, pneumonia is a major contributor to morbidity and mortality, with an estimated 100,000 annual deaths and 1.5 million annual hospitalizations.44 The American Thoracic Society (ATS) and Infectious Diseases Society of America (IDSA) recommendations for empiric antimicrobial therapy in community-acquired pneumonia (CAP) are based on selecting agents targeted to the major treatable respiratory bacterial pathogens.45 However, systematic surveillance studies indicate that patients hospitalized for suspected CAP are more than twice as likely to harbor respiratory viruses than bacteria, and influenza accounts for only a minority of respiratory viruses that could cause pneumonia.46-48 There is difficulty in distinguishing between bacterial and viral etiologies in lower respiratory tract infections (LRTIs) due to similar manifestations, commonly resulting in the overuse of antibiotics.49 In patients with isolated viral pneumonia, antibiotic therapy may be safely withheld if these infections can be easily differentiated from those with concomitant bacterial etiology.50
Procalcitonin (PCT) is a component of the innate proinflammatory response to bacterial challenge, discriminating between viral and bacterial infections.51 A Cochrane Review of randomized controlled trials (RCTs) showed a 2.4-day reduction in antibiotic exposure (5.7 vs 8.1 days; P<0.001), a lower risk for antibiotic-related adverse effects (16.3% vs 22.1%; P<0.001), and significantly lower mortality (8.6% vs 10.0%; P=0.037) with a PCT-guided AMS algorithm in adults with LRTIs compared with usual care, respectively.52 Studies outside of RCTs showed that clinicians do not rely solely on PCT to guide antimicrobial treatment decisions to improve the management of CAP.49,53-56 First, a PCT threshold allowing perfect discrimination between viral and bacterial detection has not been identified.57 Results were further supported by a meta-analysis of CAP patients demonstrating that PCT’s sensitivity (about 55%; 95% CI, 37%-71%) and specificity (76%; 95% CI, 62%-86%) are too low and variable to provide reliable evidence to enable clinicians to confidently make antimicrobial decisions based on whether the infection is bacterial or viral.58 The ATS/IDSA guidelines for the diagnosis and treatment of adults with CAP recommend empiric antibiotic therapy to be Initiated in adults with clinically suspected and radiographically confirmed CAP regardless of initial serum PCT level.45 Furthermore, PCT use does not consistently reduce antimicrobial use in patients with LRTI compared with usual care—a consequence of subpar adherence to the PCT-guided antimicrobial prescribing guideline and lack of real-time AMS prospective audit and feedback.52,59
Multiplex syndromic respiratory assays, such as the BioFire FilmArray Respiratory 2.1 Panel (bioMérieux), ePlex Respiratory Pathogen Panel (GenMark Diagnostics), and NxTAG Respiratory Pathogen Panel and Verigene Respiratory Pathogens Flex Test (Luminex), may be useful as adjunctive mRDTs. As an important intervention to reduce the use of inappropriate antibiotics, AMS guidelines advocate rapid testing for respiratory viruses.10 In a multicenter, retrospective cohort analysis of 166,273 adult patients admitted with suspected pneumonia in 179 hospitals nationwide, only 24.5% were tested for respiratory viruses, with most being tested for influenza.60 Antibacterial courses were significantly shorter for confirmed virus-positive patients versus negative patients overall (5.5 vs 6.4 days; P<0.001), but varied by bacterial testing and results. In several quasi-experimental studies, implementation of a respiratory viral panel (RVP) has demonstrated their impact on antimicrobial use, with limited changes in overall patient outcomes.61 A recent study also examined the use of the RVP in immunocompromised patients and was able to show decreased beta-lactam and macrolide use, but no difference in oseltamivir use or patient outcomes such as LOS.62
The IDSA’s Molecular Diagnostics Committee suggests that the combination of respiratory viral testing and PCT may be more likely to exclude bacterial coinfection with confidence.63 Molecular RVP combined with PCT and ASM intervention had a higher proportion of antibiotic discontinuation or deescalation, and significantly reduced IV antibiotic DOT (10.0 vs 14.5 days; P<0.001).64 These tools also can be combined with a common diagnostic stewardship intervention, “the nudge.” When combined with an electronic “nudge” to reconsider antimicrobial therapy in patients with positive RVP and low PCT, the intervention results in significantly decreased treatment durations and discharge prescriptions (20% vs 47.8%; P<0.001).65 In the absence of ASM intervention, previous evidence showed low rates of antibiotic discontinuation in patients with negative PCT and positive RVP.66 Reduction in antibiotic DOT observed with the RVP and PCT combination with a varying level of AMS intervention appears to be similar if not greater and more consistent compared with PCT alone or RVP use with antibiotic stewardship program (ASP) intervention, but more robust head-to-head comparisons are needed.49,52,64,65,67
The FDA cleared the BioFire FilmArray Pneumonia Panel (bioMérieux) and Unyvero Lower Respiratory Tract (LRT) Panel (Opgen), which are multiplex syndromic molecular testing panels for LRTIs. Both panels are compatible with multiple specimen types (sputum, endotracheal aspirates, bronchoalveolar lavage fluid). Although clinical specificity may be improved with semiquantitative analysis, neither molecular testing panels nor culture distinguish airway colonizers from invasive pathogens. Molecular testing for bacterial pathogens was not addressed by the current CAP or hospital- or ventilator-associated pneumonia guidelines because their performance and potential effect on clinical decision making have not been determined.45,68
The BioFire FilmArray Pneumonia Panel identifies 8 viruses, 3 atypical bacteria (qualitatively), 15 bacterial targets (semiquantitative analysis), and 8 resistance mechanisms.69 The BioFire FilmArray Pneumonia Panel demonstrates a positive percent agreement (PPA) and negative percent agreement (NPA) of 98.1% and 96.2%, respectively, for the identification of bacterial targets in bronchoalveolar lavage specimens compared with culture.70 Similarly, a high overall agreement of 99.2% (95% CI, 98.4%-99.6%) for viral detection is observed between the BioFire FilmArray Pneumonia Panel and culture.71 The concordance rate of the mRDTs semiquantitative analysis among positive culture specimens was only 47.7%.72 Likewise, Kolenda et al observed high sensitivity and specificity using the panel in patients with severe COVID-19 (SARS-CoV-2), but 60.5% of the bacterial targets reported with the panel were not recovered by culture and 76.9% of discordant results corresponded to bacteria belonging to commensal oral flora and/or report with 105 copies/mL or fewer bacterial nucleic acids.73 Among clinical sputum cultures, the panel detected significantly more pathogens than standard testing.74 Clinical utility and cost-effectiveness have not been fully evaluated, but a recent study of mechanically ventilated ICU patients proposed potential cost-benefit if the test resulted in real-time adjustments of empiric antimicrobial therapy.75 A retrospective multicenter study observed antimicrobial deescalation in 63 of 159 (40%) and escalation in 35 (22%) hospitalized pneumonia patients based on BioFire FilmArray Pneumonia Panel results, reinforcing its potential to reduce unnecessary antimicrobial exposure and increase the appropriateness of empiric antibiotic therapy.76 The BioFire FilmArray Pneumonia Panel may be useful to rule out bacterial coinfections and avoid inappropriate prescribing of antibiotics, but positive results should be interpreted with caution. Furthermore, although the BioFire FilmArray Pneumonia Panel can detect resistance genes with concordance with culture results, CTX-M and carbapenemase genes could not be definitively linked to the microorganism(s) detected.77
The Unyvero LRT Panel detects 30 bacterial pathogens, including Pneumocystis jirovecii, and 19 resistance genes.78 Klein et al found overall PPA and NPA of the Unyvero LRT Panel with culture of 93.4% and 98.3%, respectively, but 21.7% of specimens had additional potential pathogens identified by the panel.79 The PPA for antibiotic resistance markers compared with antibiotic susceptibility testing ranged from 80% to 100%. Challenges in interpretation also have been noted for the Curetis Unyvero LRT Panel—not all genes could be attributed to an organism, highlighting the essential continuation of current culture methods with antimicrobial susceptibility testing.80 Challenges in interpretation of newer mRDTs, especially with resistance genes, may be potentially mitigated by ASP intervention, requiring further exploration.
Surveillance Screening for MRSA by Nasal PCR
The nasal PCR screening test for methicillin-resistant S. aureus (MRSA) has become a robust AMS tool to assist in de- escalation from unnecessary MRSA therapy, such as vancomycin and linezolid. Numerous single-center studies have demonstrated the ability of AMS programs to leverage the high NPV of negative MRSA nasal swabs to alter empiric antimicrobial therapy directed toward LRTIs.81-84 Evidence for the MRSA nasal screening to rule out MRSA pneumonia has shown an NPV of 76% to 99%, depending on local prevalence.84,85 Thus, the current CAP guidelines recommend the routine use of the MRSA nasal PCR for the deescalation of MRSA coverage.45 Implementation with AMS intervention has been associated with a median decrease of 2.1 days of vancomycin use (P<0.01).86 A pharmacist-driven MRSA nasal PCR–based testing protocol with ASP effort had a 70% acceptance rate for vancomycin discontinuation within 24 hours of negative results, significantly reducing unnecessary vancomycin use with an estimated cost avoidance of $40 per vancomycin course.83 Vancomycin avoidance in suspected or confirmed pneumonia with MRSA nasal screening among ICU patients has been associated with an even higher cost avoidance of $108 per patient based on the cost of surveillance testing, vancomycin, and vancomycin therapeutic drug monitoring levels.87
The clinical utility of the MRSA nasal PCR appears to extend to other indications, such as skin and soft tissue infections (SSTIs).88 A Veterans Administration (VA) study supported this notion in the largest cohort to date, which includes 561,325 clinical cultures. A high overall NPV was observed for all infection types (96.5%) and specific infections such as BSIs (96.5%), IAIs (98.6%), respiratory infections (96.1%), surgical site infections (93.1%), and urinary tract infections (99.2%).89 A retrospective quasi-experimental VA study leveraged a negative MRSA screening protocol to decrease MRSA therapy in patients with diabetic foot infection. The study has a baseline MRSA positivity by nasal PCR of 12%. After implementation of a protocol, there was a decrease in duration of MRSA therapy from 72 hours (IQR, 27-120 hours) to 24 hours (IQR, 12-72 hours) (P<0.01).90
Gastrointestinal Infection Panels
Gastrointestinal (GI) multiplex PCR panels, such as the Film- Array Gastrointestinal Pathogen Panel (bioMérieux), xTAG Gastrointestinal Pathogen Panel (Luminex), and microarray-based panels such as Verigene Enteric Pathogen (Luminex), have been developed to help rapidly identify causative pathogens of infectious diarrhea.91 Conventional testing, such as stool culture, has a slow turnaround time of 3 to 5 days.92,93 These rapid panels are highly sensitive, encompass a broad range of community-acquired bacterial, viral, and parasitic pathogens in the United States, and typically yield results in 1 to 5 hours. These panels, however, have very specific niches where they are of clinical utility. Since most organisms on the panel represent community acquisition, use of these panels is limited after 72 hours of hospital admission.91 Additionally, where the pretest probability for specific pathogens is low (ie, based on patient symptomatology and exposure history), there is a chance for false positives that are difficult to verify by conventional methods. Lastly, since prolonged shedding of unviable viral pathogens is common, these tools may lead to false-positive diagnosis for active infection or prolonged treatment if used as a test of cure.
Diagnostic stewardship strategies such as development of clinical criteria for testing, selective reporting of results, and maintenance of separate testing methods for Clostridioides difficile are potential AMS strategies to mitigate incidental detection and inappropriate treatment.94 They are needed because negative consequences of these broad multiplex molecular panels may be introduced through inclusion of several targets of questionable clinical significance in specific patient populations, including enteropathogenic E. coli (EPEC), C. difficile, and low-incidence targets.95 EPEC is one of the most frequently positive targets, followed by C. difficile, but may represent colonization and lead to unnecessary treatment due to its prevalence in adults in the United States.96 These false positives also have important public health consequences in terms of “pseudo-outbreaks” and the CDC’s National Healthcare Safety Network reporting. For example, inclusion of C. difficile (toxin a/b) raises serious concerns for overdiagnosis and treatment since C. difficile colonizes more than half of children younger than 12 months of age and 5% to 10% of asymptomatic adults.91 As such, the BioFire Film- Array Panel received FDA approval to conceal the C. difficile target.95 In a single-center, quasi-experimental study, Marcelin et al implemented a hard stop in the electronic health record as diagnostic stewardship to prevent clinicians from ordering the panel more than once per admission or in patients with diarrhea hospitalized for more than 72 hours, resulting in significant reductions in inappropriate testing and costs. There was an estimated 30% reduction in total ordering rates (relative risk, 0.70; 95% CI, 0.63-0.78; P<0.001), with the rate of inappropriate tests also decreasing from 21.5% to 4.9% (P<0.0001).97 Total savings calculated, factoring only orders triggering the hard stop, were about $67,000. Robust studies with diagnostic stewardship are needed to fully capture the impact of these panels on hospital clinical and financial outcomes.
The use of multiplex GI panels, compared with standard stool culturing, has demonstrated mixed results in terms of both antimicrobial use metrics and patient outcomes. In a single-center pre/post-implementation study, researchers found an association between panel implementation and decreased hospital LOS, from 7.5 down to 3 days (P=0.0002).98 They did not observe changes in empiric antimicrobial use, but reported fewer patients being discharged on an antimicrobial agent (from 14% to 4.5%; P<0.001). These results contrast with another recent study that found use of the GI panel directly associated with more use of antimicrobials after implementation (36.7% before versus 63.9% after implementation; P=0.014).99 Importantly, this study was limited to bacterial pathogens detected on the panel, excluding patients with viral or parasitic pathogens. In a single-center, prospective observational study, Keske et al reported that the panel post-AMS intervention, educational meetings, and activities with providers decreased antibiotic use compared with pre-AMS intervention (42.9% vs 25.8%, respectively; P=0.023).100 Antimicrobial stewardship programs should work closely with clinical microbiology when implementing these tests to ensure they are leveraged safely and effectively.
Central Nervous System Infections
Infections of the central nervous system (CNS) are associated with significant morbidity and mortality, requiring timely medical management, including rapid identification of infectious etiology and administration of antimicrobial therapy.101,102 Bacterial meningitis and viral encephalitis rely heavily on cerebrospinal fluid (CSF) examination. In bacterial meningitis, CSF cultures are positive in 70% to 85% of patients who have not received prior antimicrobial therapy, but cultures may take up to 48 hours for organism identification. For viral encephalitis, more than 10% of patients can have normal CSF findings and CSF cultures are often of limited clinical value.103 Current meningitis and encephalitis treatment guidelines support the adjunctive use of multiplex molecular diagnostic tests to establish the specific etiology of infection.101,103 Molecular diagnostics are increasingly being relied on to provide definitive diagnosis, particularly in viral CNS infections.104 The BioFire FilmArray Meningitis/Encephalitis (ME) Panel (bioMérieux) tests for 14 common community-acquired bacterial, viral, and fungal pathogens.105,106
Despite the rapidity of this panel, false positives for S. pneumoniae, variable sensitivity for herpes simplex virus 1/2, and poor sensitivity for Cryptococcus, compared with antigen testing, have been seen.107-109 Impact on patient outcomes, such as hospital LOS and antimicrobial duration, show inconsistent results.110,111 A recent quasi-experimental study implementing the BioFire FilmArray ME Panel demonstrated decreased median days of antimicrobial therapy (3 [IQR, 0-5 days] vs 2 days [IQR, 2-5 days]; P=0.099) and acyclovir (3 [IQR, 2.5-4.5 days] vs 2 days [IQR, 1-3 days]; P=0.002).112 There was no difference in hospital LOS or inpatient mortality. A systematic review and meta-analysis examined 13 publications investigating the effect of the BioFire FilmArray ME Panel on patient outcomes.113 The reviewers determined that using the panel was associated with a decreased LOS (mean difference, –1.20 days; 95% CI, –1.96 to –0.44 days) and a significant reduction in duration of acyclovir therapy. Further clinical validation, possibly with an AMS approach, may be beneficial since the panel falls short as a stand-alone test, requiring additional tests for confirmation.92,114 An example can be found in a diagnostic stewardship intervention among pediatric patients where clinical decision support coupled with AMS audit and feedback were able to demonstrate significant improvements in time to optimal therapy.115
Limited novel technologies are in development to assist in the management of CNS infections. There is currently a CE-IVD-marked rapid multiplex PCR test from QIAstat-Dx (Qiagen).116 This ME panel includes 15 pathogens that are associated commonly with community-acquired CNS infections. Compared with the BioFire FilmArray ME panel, the QIAstat-Dx ME panel does not detect cytomegalovirus and instead includes Mycoplasma pneumoniae and Streptococcus pyogenes. Limited clinically relevant data are available currently for the QIAstat-Dx ME panel. The panel had a PPA of 100% and NPA of 98.7% compared with standard reference methods.
Outpatient Diagnostic Testing
Although AMS initiatives around RDTs have been primarily in the inpatient setting, the importance of AMS in the outpatient setting has been increasingly recognized, leading to the release of the Core Elements of Outpatient Antibiotic Stewardship.117 Based on population database evaluations in the United States, at least one-third of antimicrobial prescribing is considered inappropriate, mainly related to respiratory infections.118 Clinical Laboratory Improvement Amendments (CLIA)-waived point-of-care (POC) testing is becoming increasingly common in outpatient and community settings.119 Examples include ID NOW and BinaxNOW (Abbott), Cobas Liat PCR (Roche Diagnostics), Xpert Xpress (Cepheid), and FilmArray Respiratory Panel EZ (bioMérieux). The ID NOW influenza A & B 2 (ID NOW 2) was found to have a significantly higher sensitivity than the rapid antigen detection test (97.8% vs 78.9%).120 In a study comparing the performance of ID NOW 2, Cobas influenza A/B PCR, and Xpert Xpress Flu for Flu A and Flu B, the overall sensitivities were 93.2%, 100%, and 100% and 97.2%, 94.4%, and 91.7%, respectively.121
Although there are logistical and reimbursement limitations to implementing POC testing in outpatient settings such as community pharmacies, their importance and public health benefit cannot be denied.122 For instance, a recent study documented 661 visits during which pharmacy-based group A Streptococcus (GAS) infection and influenza POC testing was performed. This availability greatly improved access to care because nearly 50% of individuals tested did not have a primary care provider.123 Through collaborative practice agreements, pharmacists can prescribe therapies for those testing positive for GAS or influenza, which can not only improve access to care but decrease burden on already stressed systems such as emergency departments.124 The importance of equitable access to diagnosis and treatment recently became apparent during the COVID-19 pandemic, when pharmacies became easily accessible spaces for SARS-CoV-2 testing and the first oral antiviral agent targeting COVID-19.125
These tools are also indispensable in the urgent care and emergency department (ED) settings. The impact of Xpert Xpress Flu on clinical decisions was evaluated in 339 pediatric encounters.126 After results became available, original plans were changed in 44.5% of positive cases compared with 92.6% of negative cases (P<0.001). A total of 135 antiviral prescriptions were avoided in patients with negative results. The BioFire FilmArray Respiratory Panel EZ has also demonstrated its ability to assist in the appropriate use of antibiotics and was associated with a decrease in clinic appointment duration in the outpatient pediatric setting.127 There is uncertainty, however, whether the implementation of Respiratory Panel EZ would reduce the use of downstream health care resources, including radiological and laboratory tests, and follow-up appointments.128 These tests should be used with AMS intervention to improve prescribing practices. A recent trial among children seen in the ED randomized patients to routine clinical care versus rapid diagnostic testing for influenza-like illness. Among the 931 visits, children with rapid testing showed there was no significant difference in prescriptions for antimicrobials or antivirals.129 Implementation of these new technologies will require consideration of appropriate patient populations and process measures, such as antibiotic avoidance and use of antivirals, radiological and laboratory tests, and other health care resources.130
Conclusion
A multitude of technological advances for the management of BSIs, LRTIs, infectious diarrhea, CNS infections, and outpatient respiratory infections have continued to advance the field of infectious diseases. Molecular RDTs have been increasingly recognized for their significant impact on clinical outcomes, antimicrobial use, and cost savings. Many of these RDTs show promise in their potential to improve patient care, but implementation of efficient evidence-based ASP interventions and diagnostic stewardship with pragmatism in mind are expected to be necessary to augment appropriate use and interpretation for translational outcomes. As clinicians, we should ensure the value of RDTs is not only increasing the accuracy and rapidity of diagnosis, but also changing clinical management, improving patient outcomes, and yielding overall cost-effectiveness, thus highlighting the importance of continued efficacy evaluations of these technologies.
References
- Graf EH, Pancholi P. Curr Infect Dis Rep. 2020;22:5.
- Briggs N, Campbell S, Gupta S. Diagn Microbiol Infect Dis. 2021;99(1):115219.
- Palavecino EL, Williamson JC, Ohl CA. Infect Dis Clin North Am. 2020;34(1):51-65.
- Pogue JM, Heil EL, Lephart P, et al. Antimicrob Agents Chemother. 2018;62:e02538-17.
- Rader TS, Stevens MP, Bearman G. Curr Infect Dis Rep. 2021;23(4):5.
- Timbrook TT, Morton JB, McConeghy KW, et al. Clin Infect Dis. 2017;64(1):15-23.
- Messacar K, Parker SK, Todd JK, et al. J Clin Microbiol. 2017;55(3):715-723.
- Lapin JS, Smith RD, Hornback KM, et al. Pharmacotherapy. 2023 May 9. doi:10.1002/phar.2813
- Claeys KC, Johnson MD. Drugs Context. 2023;12:2022-9-5.
- Barlam TF, Cosgrove SE, Abbo LM, et al. Clin Infect Dis. 2016;62(10):e51-e77.
- Banerjee R, Humphries R. Front Med (Lausanne). 2021;8:635831.
- Patel TS, Kaakeh R, Nagel JL, et al. J Clin Microbiol. 2017;55(1):60-67.
- Perez KK, Olsen RJ, Musick WL, et al. Arch Pathol Lab Med. 2012;137(9):1247-1254.
- Pliakos EE, Andreatos N, Shehadeh F, et al. Clin Microbiol Rev. 2018;31(3):e00095-17.
- Claeys KC, Schlaffer K, Smith R, et al. Clin Infect Dis. 2021;73(6):1103-1106.
- Claeys KC, Hopkins TL, Schlaffer K, et al. Antimicrob Agents Chemother. 2021;65(9):e0044121.
- Wilson BM, Jiang Y, Jump RLP, et al. Clin Infect Dis. 2021;73(3):344-350.
- Pancholi P, Carroll KC, Buchan BW, et al. J Clin Microbiol. 2018;56(4):e01329-17.
- Charnot-Katsikas A, Tesic V, Love N, et al. J Clin Microbiol. 2018;56:e01166-17.
- Bhalodi AA, Magnano P, Humphries RM. Diagn Microbiol Infect Dis. 2020;98(4):115171.
- Pfaller MA, Wolk DM, Lowery TJ. Future Microbiol. 2016;11(1):103-117.
- Weinrib DA, Capraro GA. Ann Intern Med. 2019;170(12):888-889.
- Nguyen MH, Clancy CJ, Pasculle AW, et al. Ann Intern Med. 2019;170(12):845-852.
- Kalligeros M, Zacharioudakis IM, Tansarli GS, et al. BMC Infect Dis. 2020;20(1):326.
- Quirino A, Scaglione V, Marascio N, et al. BMC Infect Dis. 2022;22(1):113.
- Giannella M, Pankey GA, Pascale R, et al. Expert Rev Med Devices. 2021;18(5):473-482.
- Monday LM, Parraga Acosta T, Alangaden G J Fungi (Basel). 2021;7(7):178.
- Pfaller MA, Diekema DJ. Clin Microbiol Rev. 2007;20(1):133-163.
- Pappas PG, Kauffman CA, Andes DR, et al. Clin Infect Dis. 2016;62(4):e1-e50.
- Mylonakis E, Clancy CJ, Ostrosky-Zeichner L, et al. Clin Infect Dis. 2015;60(6):892-899.
- Patch ME, Weisz E, Cubillos A, et al. J Antimicrob Chemother. 2018;73(suppl 4):iv27-iv30.
- Steuber TD, Tucker-Heard G, Edwards J, et al. Diagn Microbiol Infect Dis. 2020;97(4):115086.
- Bomkamp JP, Sulaiman R, Hartwell JL, et al. J Clin Microbiol. 2020;58(3):e01408-19.
- Patrocínio de Jesus R, Houston H, Schutte AHJ, et al. JAC Antimicrob Resist. 2023;5(2):dlad035.
- Lamoth F, Clancy CJ, Tissot F, et al. Open Forum Infect Dis. 2020;7(3):ofaa075.
- Zurl C, Prattes J, Zollner-Schwetz I, et al. Med Mycol. 2020;58(5):632-638.
- Bassetti M, Righi E, Ansaldi F, et al. Intensive Care Med. 2015;41(9):1601-1610.
- Bork JT, Leekha S, Heil EL, et al. Antimicrob Agents Chemother. 2015;59(3):1588-1595.
- Claeys KC, Heil EL, Pogue JM, et al. Diagn Microbiol Infect Dis. 2018;91(2):144-146.
- Goggin KP, Gonzalez-Pena V, Inaba Y, et al. JAMA Oncol. 2020;6(4):552-556.
- Hogan CA, Yang S, Garner OB, et al. Clin Infect Dis. 2021;72(2):239-245.
- MacIntyre AT, Hirst A, Duttagupta R, et al. Appl Health Econ Health Policy. 2021;19(2):231-241.
- Shishido AA, Noe M, Saharia K, et al. BMC Infect Dis. 2022;22(1):372.
- Ramirez JA, Wiemken TL, Peyrani P, et al. Clin Infect Dis. 2017;65(11):1806-1812.
- Metlay JP, Waterer GW, Long AC, et al. Am J Respir Crit Care Med. 2019;200(7):e45-e67.
- Burk M, El-Kersh K, Saad M, et al. Eur Respir Rev. 2016;25(140):178-188.
- Piralla A, Mariani B, Rovida F, et al. J Clin Virol. 2017;92:48-51.
- Jain S, Self WH, Wunderink RG, et al. N Engl J Med. 2015;373(24):2382.
- Huang DT, Yealy DM, Filbin MR, et al. N Engl J Med. 2018;379(3):236-249.
- Ruuskanen O, Lahti E, Jennings LC, et al. Lancet. 2011;377(9773):1264-1275.
- Gilbert DN. Clin Infect Dis. 2011;52(suppl 4):s346-s350.
- Schuetz P, Wirz Y, Sager R, et al. Cochrane Database Syst Rev. 2017;10(10):CD007498.
- Ammar AA, Lam SW, Duggal A, et al. Pharmacotherapy. 2017;37(2):177-186.
- Branche AR, Walsh EE, Vargas R, et al. J Infect Dis. 2015;212(11):1692-1700.
- Broyles MR. Open Forum Infect Dis. 2017;4(4):ofx213.
- Nguyen CT, Li J, Occhipinti EA, et al. Open Forum Infect Dis. 2018;5(2):ofy012.
- Self WH, Balk RA, Grijalva CG, et al. Clin Infect Dis. 2017;65(2):183-190.
- Kamat IS, Ramachandran V, Eswaran H, et al. Clin Infect Dis. 2020;70(3):538-542.
- Newton JA, Robinson S, Ling CLL, et al. Open Forum Infect Dis. 2019;6(11):0fz355.
- Klompas M, Imrey PB, Yu P-C, et al. Infect Control Hosp Epidemiol. 2021;42(7):817-825.
- Covert K, Bashore E, Edds M, et al. J Clin Pharm Ther. 2021;46(2):277-285.
- Bergese S, Fox B, García-Allende N, et al. Rev Argent Microbiol. 2023;s0325-s7541(23)00026-3.
- Hanson KE, Azar MM, Banerjee R, et al. Clin Infect Dis. 2020;71(10):2744-2751.
- Lee C-C, Chang JC-Y, Mao X-W, et al. J Am Med Dir Assoc. 2020;21(1):62-67.
- Moradi T, Bennett N, Shemanski S, et al. Clin Infect Dis. 2019;71(7):1684-1689.
- Timbrook T, Maxam M, Bosso J. Infect Dis Ther. 2015;4(3):297-306.
- Srinivas P, Rivard KR, Pallotta AM, et al. Pharmacotherapy. 2019;39(6):709-717.
- Kalil AC, Metersky ML, Klompas M, et al. Clin Infect Dis. 2016;63(5):e61-e111.
- The BioFire FilmArray Pneumonia Panel. Accessed July 3, 2023. https://www.biofiredx.com/ products/ the-filmarray-panels/ filmarray-pneumonia/
- Buchan BW, Windham S, Balada-Llasat J-M, et al. J Clin Microbiol. 2020;58(7):e00135-20.
- Webber DM, Wallace MA, Burnham CA, et al. J Clin Microbiol. 2020;58(7):e00343-20.
- Kamel NA, Alshahrani MY, Aboshanab KM, et al. 2022;11(3):377.
- Kolenda C, Ranc A-G, Boisset S, et al. Open Forum Infect Dis. 2020;7(11):ofaa484.
- Falsey AR, Branche AR, Croft DP, et al. J Infect Dis. 2023;jiad221.
- Ferrer J, Clari Má, Giménez E, et al. Diagn Microbiol Infect Dis. 2023;105(2):115847.
- Monard C, Pehlivan J, Auger G, et al. Crit Care. 2020;24(1):434.
- Yoo IY, Huh K, Shim HJ, et al. Int J Infect Dis. 2020;95:326-331.
- Unyvero lower respiratory pneumonia can be fatal. OpGen. Accessed July 3, 2023. https://www.opgen.com/ unyvero/ unyvero-lower-respiratory/
- Klein M, Bacher J, Barth S, et al. J Clin Microbiol. 2021;59(3):e02497-20.
- Collins ME, Popowitch EB, Miller MB. J Clin Microbiol. 2020;58(5):e02013-19.
- Bono K, Caceda JA, Zhai M, et al. J Surg Res. 2023;283:1047-1052.
- Marinucci V, Louzon PR, Carr AL, et al. Ann Pharmacother. 2023;57(5):560-569.
- Meng L, Pourali S, Hitchcock MM, et al. Open Forum Infect Dis. 2021;8(4):ofab099.
- Smith MN, Brotherton AL, Lusardi K, et al. Ann Pharmacother. 2019;53(6):627-638.
- Parente DM, Cunha CB, Mylonakis E, et al. Clin Infect Dis. 2018;67(1):1-7.
- Willis C, Allen B, Tucker C, et al. Am J Health Syst Pharm. 2017;74(21):1765-1773.
- Smith MN, Erdman MJ, Ferreira JA, et al. J Crit Care. 2017;38:168-171.
- Butler-Laporte G, De L’étoile-Morel S, Cheng MP, et al. J Infect. 2018;77(6):489-495.
- Mergenhagen KA, Starr KE, Wattengel BA, et al. Clin Infect Dis. 2020;71(5):1142-1148.
- Harb G, Hopkins T, Yang L, et al. BMC Infect Dis. 2023;23(1):297.
- Hata DJ, Powell EA, Starolis MW. J Appl Lab Med. 2023;jfad009.
- Hanson KE, Couturier MR. Clin Infect Dis. 2016;63(10):1361-1367.
- Ramanan P, Bryson AL, Binnicker MJ, et al. Clin Microbiol Rev. 2017;31(1):e00024-17.
- Baghdadi JD, Coffey KC, Leekha S, et al. Curr Infect Dis Rep. 2020;22:15.
- Dien Bard J, McElvania E. Clin Lab Med. 2020;40(4):393-420.
- Buss SN, Leber A, Chapin K, et al. J Clin Microbiol. 2015;53(3):915-925.
- Marcelin JR, Brewer C, Beachy M, et al. Infect Control Hosp Epidemiol. 2019;40(6):668-673.
- Torres-Miranda D, Akselrod H, Karsner R, et al. BMC Gastroenterol. 2020;20:246.
- Carmon D, Rohana H, Azrad M, et al. Diagnostics (Basel). 2023;13(6):1094.
- Keske S, Zabun B, Aksoy K, et al. J Clin Microbiol. 2018;56(5):e00148-18.
- Tunkel AR, Hartman BJ, Kaplan SL, et al. Clin Infect Dis. 2004;39(9):1267-1284.
- Dagra A, Lyerly M, Lucke-Wold B. Clin Res. (Westerville). 2023;4(1):8.
- Tunkel AR, Glaser CA, Bloch KC, et al. Clin Infect Dis. 2008;47(3):303-327.
- Gundamraj V, Hasbun R. Curr Opin Infect Dis. 2023;36(3):177-185.
- Saravolatz LD, Manzor O, VanderVelde N, et al. Clin Infect Dis. 2003;36(1):40-45.
- BioFire FilmArray Meningitis/Encephalitis Panel (ME) | BioFire Diagnostics. Accessed June 30, 2023. https://www.biofiredx.com/ products/ the-filmarray-panels/ filmarrayme/
- Leber AL, Everhart K, Balada-Llasat J-M, et al. J Clin Microbiol. 2016;54(9):2251-2261.
- Liesman RM, Strasburg AP, Heitman AK, et al. J Clin Microbiol. 2018;56(4):e01927-17.
- O’Halloran JA, Franklin A, Lainhart W, et al. Open Forum Infect Dis. 2017;4(4):ofx242.
- DiDiodato G, Bradbury N. Open Forum Infect Dis. 2019;6(4):ofz119.
- Dack K, Pankow S, Ablah E, et al. Kans J Med. 2019;12(1):1-3.
- Markovich K, Wingler MJB, Stover KR, et al. Diseases. 2022;10(4):110.
- Hueth KD, Thompson-Leduc P, Totev TI, et al. Antibiotics (Basel). 2022;11(8):1028.
- Vetter P, Schibler M, Herrmann JL, et al. Clin Microbiol Infect. 2020;26(6):706-712.
- Messacar K, Palmer C, Gregoire L, et al. J Pediatr. 2022;244:161-168.e1.
- Humisto A, Antikainen J, Holma T, et al. Microbiol Spectr. 2023;11(3):e0514422.
- Sanchez GV, Fleming-Dutra KE, Roberts RM, et al. MMWR Morb Mortal Wkly Rep Recomm Rep. 2016;65(6):1-12.
- Fleming-Dutra KE, Hersh AL, Shapiro DJ, et al. JAMA. 2016;315(17):1864-1873.
- Weber NC, Klepser ME, Akers JM, et al. Expert Rev Mol Diagn. 2016;16(2):253-264.
- Mitamura K, Yamazaki M, Ichikawa M, et al. J Infect Chemother. 2021;27(3):450-454.
- Kanwar N, Michael J, Doran K, et al. J Clin Microbiol. 2020;8(3):e01611-19.
- Klepser M, Koski RR. Expert Rev Mol Diagn. 2022;1-14.
- Klepser DG, Klepser ME, Smith JK, et al. Res Social Adm Pharm. 2018;14(4):356-359.
- Klepser DG, Klepser ME, Dering-Anderson AM, et al. J Am Pharm Assoc. (2003) 2016;56(3):323-329.e1.
- Mahoney MV, Bhagat H, Christian R, et al. Antimicrob Steward Healthc Epidemiol. 2022;2(1):e112.
- El Feghaly RE, Nolen JD, Lee BR, et al. J Pediatr. 2021;228:271-277.e1.
- Beal SG, Posa M, Gaffar M, et al. Pediatr Infect Dis J. 2020;39(3):188-191.
- Fenton J, Posa M, Kelly M, et al. Pediatr Infect Dis J. 2020;39(9):e282-e283.
- Rao S, Lamb MM, Moss A, et al. JAMA Netw Open. 2021;4(6):e2111836.
- Kozel TR, Burnham-Marusich AR. J Clin Microbiol. 2017;55(8):2313-2320.
Copyright © 2023 McMahon Publishing, 545 West 45th Street, New York, NY 10036. Printed in the USA. All rights reserved, including the right of reproduction, in whole or in part, in any form.

Download to read this article in PDF document:![]() Keeping Updated on Clinical Rapid Diagnostic Tests for Bacteremia and Beyond
Keeping Updated on Clinical Rapid Diagnostic Tests for Bacteremia and Beyond