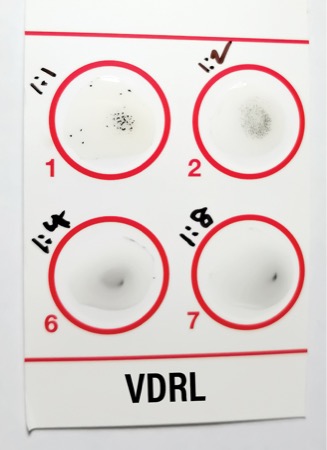
The outcomes of a syphilis infection during pregnancy can be tragic. Because of this, the U.S. Preventive Services Task Force (USPSTF) is continuing to recommend early, universal syphilis screening during pregnancy.
The new guidance, a restatement of its 2018 recommendations, comes at a time when syphilis cases remain high in the United States. That also includes 3,882 cases of congenital syphilis in the United States in 2023, the highest number of cases in 30 years, which caused 279 stillbirths or neonatal/infant deaths (JAMA 2025 May 13. doi:10.1001/jama.2025.5009).
“Syphilis during pregnancy can cause tragic outcomes, like miscarriage, stillbirth, infant death and lifelong medical issues,” Laura Bachmann, MD, the chief medical officer in the CDC’s Division of STD Prevention, who was not involved with the guidance, told Infectious Disease Special Edition. “Early, universal screening for pregnant women remains one of the most important ways we can prevent the worst outcomes of the syphilis epidemic.”
Giving the recommendation a letter A rating, the USPSTF found that early, universal syphilis screening during pregnancy has a “substantial net benefit.” The USPSTF recommends that screening takes place early in pregnancy, but if that is not possible, then it should be performed at the earliest available opportunity. In addition, the screening is recommended universally, regardless of symptoms.
The Risks for Congenital Syphilis
Universal screening is essential because it can prevent birth defects and infant deaths, and some people could potentially have syphilis asymptomatically or have had general vague symptoms that resolved but still carry the virus. “It can be passed from mom to baby while the baby is in utero, even if mom doesn’t have symptoms. These birth defects can be life-changing if mom doesn’t get treated in time. If we catch it early and we’re able to treat it, it drastically decreases the risk of any adverse effects on the fetus or the newborn child,” explained Casey Pinto, PhD, CRMP, a nurse practitioner and an assistant professor at Penn State Cancer Institute, in Hershey, Pa. “Since syphilis can attack every part of your body, in babies, it causes changes in teeth, it causes changes in palate, it causes brain changes and they can be developmentally delayed. It can cause heart defects, bone defects, organ defects—it can literally attack anywhere in the body.”
Rates Remain High
The need to test all pregnant people is evident; cases of syphilis in the United States have risen steadily over the last 30 years, according to the USPSTF.
“They’re still increasing, but the increase is not as sharp as it was. It seems like we’re leveling off,” Dr. Pinto told IDSE. “We’re all waiting with bated breath to see the 2024 numbers, but I have no idea when we’ll get them because CDC is the one who reports those.”
In particular, cases in women have jumped. Although syphilis still is a disease more commonly seen in men, it’s now two to four times more common in women than it was in the past, as of data in 2017 and 2021, according to CDC statistics. Rates of primary and secondary syphilis increased over 600% in women, compared with just over 100% in men in the same period. Due to this increase in women, congenital syphilis has increased 10-fold from 334 cases in 2012 to 3,882 cases in 2023 (MMWR Morb Mortal Wkly Rep 2023;72[46]:1269-1274; JAMA 2025 May 13. doi:10.1001/jama.2025.5009).
“We’re seeing a lot,” Dr. Pinto said He said sometimes it feels like “all I see in clinic anymore is syphilis.”
These increases are not just occurring in the United States. Syphilis cases and in turn congenital syphilis have been increasing in developed nations around the globe. Clare Nourse, MD, MB BCh, BAO, DCH, FRACP, a professor and pediatric infection specialist at Children’s Health Queensland and the University of Queensland, in Brisbane, Australia, told IDSE that rates have also risen in her country. Where cases once were limited to men who have sex with men, as in the United States, or remote communities of Aboriginal and Torres Strait Islander people, they are now rising in women living in urban areas, “leading to a worrying resurgence of congenital syphilis,” she said. “It’s the same occurring in most high-income countries in the world.”
According to the numbers from Australian national data, just more than 5,000 cases of syphilis in women ages 15 to 44 years were reported from 2011 to 2021, with the annual number increasing from 141 in 2011 to 902 in 2021, she said. In that same period, 74 cases of congenital syphilis were reported in Australia, which breaks down to 40 Aboriginal and Torres Strait Islander infants, 32 non-Indigenous infants, and two infants of unknown ethnicity (Med J Aust 2024;221[4]:201-208).
A New Hope
Maybe rates will begin to come down. “There is a glimmer of hope,” Dr. Bachmann said, “as we’re seeing signs the syphilis epidemic may be slowing [in the United States]. In 2023, syphilis in our country increased at the lowest levels in more than a decade. Still, our nation has a long way to go to get back to where we were in the early 2000s. 2023 syphilis cases were still extremely high—the highest reported since 1950.”
However, Dr. Bachmann said to slow down the increase and potentially reduce cases, the field has to be proactive—empowering people with information and tools to protect themselves and increasing access to prevention for sexually transmitted infections (STIs), screening and treatment, among other actions, she said. “We may be at a turning point for syphilis, but only if we can maintain the current momentum.”
One method to rein in syphilis cases is to offer screening outside of obstetrics-gynecology clinics, Dr. Bachmann said. “Many cases of newborn syphilis occur among mothers who are not engaged in prenatal care, but they may access healthcare in other settings during pregnancy, such as emergency departments, maternal and child health programs, prisons or jails, and substance use programs,” she said. “It’s important that all healthcare providers serving women of reproductive age are familiar with syphilis screening recommendations for pregnant women.”
Dr. Pinto agreed that there is hope in the fight against syphilis. “In the past, the U.S. has done a really good job at controlling it, and they can do it again,” she said. The disease is not airborne, making it easier to trace in some respects than COVID-19. “But one of the things that requires is money.”
Public health officials need contact tracers, trained professionals to diagnose the condition and find contacts, medical supplies and tests, personal protective equipment, and sometimes a brick-and-mortar venue to test in. But in this time of federal budget cuts, Dr. Pinto said they’re unsure whether the funding will continue for these clinics, and she is concerned these funding cuts will lead to increases, not decreases, in cases.
“We’ll have to see how this plays out with the current administration if they decide to keep STI clinics that are government funded or not,” Dr. Pinto said. “It’s unclear what will happen in the future. But we’re all waiting.”
The sources reported no relevant financial disclosures.
This article is from the June 2025 print issue.