Kaposi sarcoma (KS) continues to play a significant part in morbidity and mortality among Black patients with HIV living in the South.
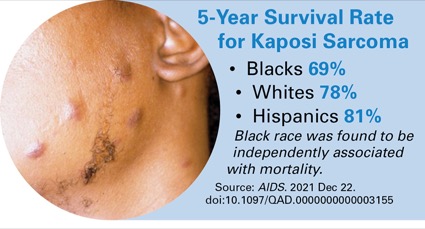
A recent study showed Black patients with HIV-associated KS had double the mortality of white or Hispanic patients with HIV-associated KS (AIDS 2021 Dec 22. doi:10.1097/QAD.0000000000003155).
“There seems to be this notion that Kaposi sarcoma is no longer a disease of interest or concern in the United States because clinicians don’t see it as much as they did in the pre-ART [antiretroviral therapy] era, and outcomes have improved because we have such effective treatment for HIV these days,” said study author Sheena Knights, MD, of The University of Texas Southwestern Medical Center, in Dallas. “While these points are true, our study highlights the fact that not only is Kaposi sarcoma still prevalent in certain areas of the U.S., but there are outcomes disparities that need to be addressed to improve outcomes in this HIV population.”
History of Kaposi Sarcoma
In the 1980s and 1990s, before ART, the presence of KS was how AIDS was diagnosed, explained Dirk P. Dittmer, PhD, of the UNC Lineberger Comprehensive Cancer Center, in Chapel Hill. It was one of the defining conditions of AIDS.
“Then came highly active ART and that led to a decline in KS,” Dr. Dittmer said. “With ART, we all of a sudden no longer had people who were severely immune suppressed.”
Rates of KS were much lower but still three to five times higher than before the 1980s, Dr. Dittmer said.
“Now we have a background level of KS that you cannot treat with just ART,” Dr. Dittmer said. “We now see KS in people that still have AIDS but don’t take ART, have had their ART disrupted or have become resistant, and in people who do take ART and have no detectable disease, but are older now.”
Dr. Dittmer said the results of the study by Dr. Knights’ team was not surprising to him, as he sees similar trends in North Carolina.
“There was an ascertainment bias that KS had gone away, which was driven by HIV providers that saw mostly white patients in San Francisco, New York City or Chicago,” Dr. Dittmer said. “That number is going down, not because there is no more KS but because many of the patients are African American and living in more rural areas.”
Differences Seen by Race and Ethnicity
Dr. Knights and her colleagues reviewed the electronic health records of patients diagnosed with HIV and KS from January 2009 to December 2018, and included 262 patients for analysis.
Of the patients, 30% were receiving ART at the time of KS diagnosis and one-fourth were first diagnosed with HIV and KS at the same time. Regarding disease stage, 46% of patients had T1, 75% had I1 and 54% had S1 stage disease.
Of the included patients with KS, 30.9% died, with a median survival duration of 11 months from KS diagnosis. Black patients had the highest mortality of all race/ethnic groups, including white and Hispanic patients.
According to Dr. Knights, U.S. Surveillance, Epidemiology, and End Results program data indicate an expected five-year survival rate of about 77% in KS, but in the current study, that rate for Black patients was 69%. The five-year survival rate was 78% for white patients and 81% for Hispanic patients. A multivariable analysis showed Black patients had a mortality risk twice that of white or Hispanic patients (hazard ratio, 2.07; 95% CI, 1.12-3.82). Black race was found to be independently associated with mortality.
“Although white and Hispanic patients had slightly better mortality than expected in our study, Black patients had worse mortality than expected,” Dr. Knights said.
Implications
Dr. Knights and her colleagues found Black patients had more advanced KS disease at diagnosis, and often were younger than other ethnicities, which could explain the mortality difference.
“What’s not clear from our study is why these patients are presenting with more advanced disease,” Dr. Knights said. “Could these patients be infected with a specific genotype of KS-associated herpesvirus that may be associated with more advanced disease? Could there be a complex combination of socioeconomic factors involved that are difficult to measure?”
She said they were unable to answer this question in this study, but hope to do so in future studies.
Dr. Knights said according to the CDC’s HIV Surveillance program, Black people in the southern United States have the highest death rates from HIV, too.
“I suspect that whatever the underlying etiology of the mortality disparity in KS is, it is most likely related to the same factors that contribute to higher mortality in HIV deaths in the southern United States,” Dr. Knights said. “We as HIV providers still have a lot of work to do to help identify and alleviate healthcare disparities.”
Dr. Dittmer reported a position as an investigator with the AIDS Malignancy Consortium. Dr. Knights reported grant funding from the UT Southwestern Simmons Comprehensive Cancer Center Pilot Award.
This article is from the March 2022 print issue.