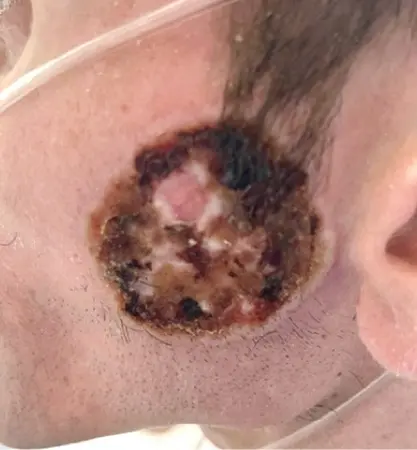
How does HIV affect mpox risk? Two abstracts presented at IDWeek 2025, in Atlanta, built on lessons learned during the 2022 mpox outbreak in New York City, including what factors put people with HIV at higher risk for severe mpox infection.
“Multiple studies have now shown that poorly controlled HIV is a risk factor for severe mpox. What is less clear is which aspect of having uncontrolled HIV is most associated with having more severe mpox,” said Bruce Aldred, MD, an assistant professor of infectious diseases at the Emory University School of Medicine, in Atlanta, who was not involved with the research.
CD4+ Counts, Viremia, And Antiretroviral Therapy
New York City had the highest number of people infected with mpox during the outbreak, with 3,821 confirmed cases by the end of 2022 (Nat Med 2025;31[5]1464-1473). In the first of the new studies, researchers collected data from 395 men in the city who had initiated the antiviral tecovirimat between May and December 2022, which was used as a proxy for severe mpox infections (abstract P-218). Of the 395 total patients, 70 (17.72%) were hospitalized. All of the men in the study had HIV.
The researchers expected to find that people without HIV viral load suppression (>200 copies/mL) would be at higher risk for hospitalization, but that was not the case after adjusting for confounders. However, the data showed that people who had low CD4+ counts (<200 cells/mm3), who tested positive for syphilis, or were off antiretroviral therapy were at higher risk for hospitalization from mpox. The findings illustrated how a single number, such as CD4+ count, does not solely account for a person’s risk for a severe mpox infection.
“These are all proxies for people not getting consistent HIV care,” said lead researcher Ofole Mgbako, MD, the section chief of infectious diseases at NYC Health + Hospitals/Bellevue.
Dr. Aldred agreed, telling Infectious Disease Special Edition that higher rates of syphilis among those hospitalized with mpox was likely an illustration of a broader issue with access to care.
“I suspect this isn’t causal, but is a shared risk factor for both,” Dr. Aldred said. “Either they don’t like going to doctors or they have trouble getting in to see doctors.”
The researchers also found that men who were hospitalized for mpox were more likely to be Black, highlighting how structural racism is amplified during an infectious disease outbreak.
“This finding keeps coming up in different cohorts,” Dr. Mgbako said. “Folks living at the intersection of these factors—experiencing racism, lack of access to insurance, having HIV—are more vulnerable to severe disease risk and severe outcomes.”
Dr. Aldred echoed that this is a lesson seen in all infectious disease outbreaks: “It is almost always the case that the group most affected is the group that was forgotten about, that was last to get access to prevention or education,” he said.
Showing Fear
The second of the two studies was a qualitative assessment that shed light on why patients may struggle to get the care they need (abstract P-735). Dr. Mgbako and his co-authors asked 20 men how they felt about their experiences seeking care for mpox.
The researchers conducted the interviews between March and December 2024, but the participants had all seen a healthcare provider for mpox during the 2022 outbreak. Nearly all of the men were sexual minorities, meaning they identified as gay, bisexual, or transgender; these minorities were most affected by the outbreak. The majority (80%, n=16) identified as gay, 45% (n=9) were Black, and 45% (n=9) were Hispanic/Latino. More than half (n=12) had an HIV diagnosis.
When patients sought treatment at emergency departments, urgent care facilities, or with their primary care providers, “a lot of providers showed their fear, and because providers did not know how to treat the virus itself, that meant that a lot of patients were turned away,” Dr. Mgbako said.
This lack of knowledge led to people having to wait longer to eventually be treated, he said. He added that when healthcare providers are faced with treating a virus they do not understand, they can start by treating the symptoms they do know how to treat.
“People described having horrible pain, and we as doctors do know how to treat pain,” he said, noting that people also struggled with having to isolate for as long as three weeks. “Connect them to other resources or specialists who do know how to treat it.”
Many of the men in the study reported that they eventually did find a provider or practice where they felt they were well taken care of and respected.
“They found someone who called and followed up, treated them with respect, and asked them how they were doing,” Dr. Mgbako said. “There are good models out there for how we give compassionate and respectful care.”
Dr. Mgbako reported a financial relationship with Gilead Sciences.
This article is from the February 2026 print issue.