By Leslie Cantu
A recent study that followed a cohort of more than 110,000 people found significant disparities in the risk for anal cancer for people with HIV and for men who have sex with men (MSM) with HIV, depending on the region of the country where they live.
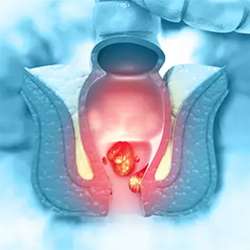
It's known that people with HIV have the highest risk for anal cancer, said lead author Ashish A. Deshmukh, PhD, a co-leader of the cancer control research program at Medical University of South Carolina Hollings Cancer Center, in Charleston.
But this study shows vast geographic disparities in anal cancer risk and an association with opportunistic illnesses and comorbidities, like diabetes, chronic kidney disease and cardiovascular disease, for people with HIV (J Nation Cancer Inst 2024 May 7. https://doi.org/10.1093/jnci/djae096).
Almost all cases of anal cancer are caused by HPV. It seems that there’s some as-yet-unknown effect, such as inflammation, in people with comorbidities that allows HPV to gain a foothold and cause cancer to develop, the paper noted.
People with HIV have a greater relative risk for anal cancer compared with those without HIV, no matter where they live. But the study showed that the relative risk varies across the country: It’s higher for people with HIV in the Midwest or South than the West or Northeast.
“In the Northeast, the risk for people with HIV compared with people without HIV is 16-fold higher,” Dr. Deshmukh said. “But for people with HIV in the Midwest, the risk increases to almost 47.5-fold, reaching nearly 100-fold for men who have sex with men with HIV.”
Dr. Deshmukh has a few preliminary theories about the causes of these differences but cautioned that this study doesn’t attempt to determine the reasons.
“The objective was to understand whether there are disparities and what may be important risk factors,” he said. However, he noted that screening rates for anal cancer are relatively higher in the Northeast and West. New York state, for example, stands out as the only state with established guidelines for anal cancer screening, a rarity given the absence of national guidelines and lack of specific protocols in other states for this relatively rare cancer, among the general population.
Various professional societies have begun to develop screening guidelines. In fact, Deshmukh contributed to the International Anal Neoplasia Society’s consensus guidelines, published in January.
Those guidelines started with the premise of beginning screening at specific ages based on risk: for example, beginning screening at age 35 for MSM with HIV and 45 for women with HIV and other men with HIV.
However, this new study suggests that guidelines should consider risk factors like previous opportunistic illnesses or having had a CD4 count below 200. CD4 count is the number of CD4 T cells, a type of white blood cell, in the blood. A count above 500 is considered healthy, but a count below 200 can trigger an AIDS diagnosis.
Dr. Deshmukh said he hopes to see the U.S. Preventive Services Task Force develop guidelines for anal cancer screening. The task force previously determined that there wasn’t enough information about the risk–benefit balance of anal cancer screening to issue guidelines, Dr. Deshmukh said.
However, his ongoing research will provide direct evidence quantifying the potential harms versus benefits of screening for anal cancer among people with HIV.
The current paper noted that anal cancer among people with HIV appears to be on the decline. However, it warned that geographic disparities could increase if the differences in screening activity remain.
This work was supported by grants from the National Institutes of Health and Canadian Institutes of Health Research. The story was originally published on the Medical University of South Carolina website. It was edited for style and length.