Originally published by our sister publication Anesthesiology News
Shreveport, Louisiana
Shingles affects millions of people worldwide annually, with the acute phase marked by intense pain and discomfort that can disrupt daily life. Traditionally, primary care providers treat these cases with antivirals and systemic analgesics. Unfortunately, not all patients achieve adequate pain control, and many progress to postherpetic neuralgia (PHN)—a debilitating condition characterized by persistent, often intractable neuropathic pain. Recent clinical experiences and studies have highlighted the potential of epidural steroid injections (ESIs) to relieve acute pain symptoms and mitigate the transition to chronic pain states. Despite these compelling data, ESIs remain underused in the initial phases of shingles management.
As a resident at Parkland Hospital, in Dallas, in 1981, I learned that ESI might be an effective treatment for shingles. However, there were no opportunities for me to manage patients with the condition until a CRNA colleague presented with it. I treated her, and have had the opportunity to do so 10 to 12 times since. Without exception, the patients had very good outcomes. Last week, an 81-year-old man came to the GI lab for evaluation for bleeding. He had shingles and I treated him. His good outcome inspired this message.
Pathophysiology of Shingles and Rationale for ESIs
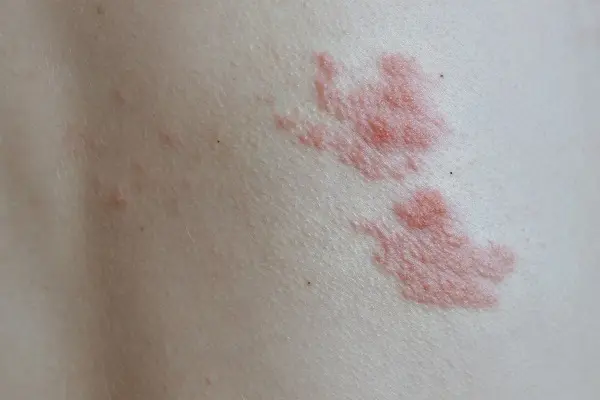
The reactivation of latent varicella-zoster virus in the dorsal root ganglia results in an inflammatory cascade. This inflammation not only produces the characteristic rash but also triggers intense neuritic pain through nerve irritation and damage. ESIs deliver corticosteroids directly to the epidural space, targeting local inflammation and reducing edema around affected nerve roots. By curtailing the inflammatory process, there are both symptomatic relief in the acute phase and a theoretical reduction in the risk of progressing to PHN. Several studies have noted rapid pain relief following appropriately administered ESIs, sometimes producing measurable improvement within 24 hours.
Current Clinical Practice and Referral Challenges
Despite the promising evidence, referrals for acute shingles pain management via ESIs remain surprisingly rare. Several factors contribute to this conundrum:
- Conventional treatment protocols. Most healthcare providers managing shingles are accustomed to initiating antiviral therapy combined with systemic pain management. This traditional approach, which centers on pharmacotherapy, leaves little room for early interventional procedures. The emphasis is often placed on treating the rash and controlling systemic symptoms rather than addressing the local nerve inflammation directly.
- Limited awareness among referring physicians. Many primary care physicians and dermatologists may be unaware of the utility of ESIs during the acute phase. Educational gaps regarding the benefits of early interventional pain management result in missed opportunities for significant pain relief—a gap that, if acknowledged, could reshape treatment algorithms.
- Established referral patterns. Anesthesiologists and pain specialists are frequently seen as providers of chronic pain management rather than acute care. These ingrained referral practices mean that patients suffering severe acute symptoms often do not get the chance to benefit from interventional treatments unless they progress to chronic pain syndromes.
- Systemic and insurance barriers. Institutional protocols and health insurance policies may discourage or complicate interventional pain techniques early in the course of shingles. These external factors can exacerbate the reluctance to refer patients for procedures that deviate from standard antiviral and analgesic regimens.
The Case for Early Interventional Pain Management
The anecdotal experiences of many anesthesiologists—including firsthand accounts of robust pain relief during the acute phase of shingles—underscore a critical unmet need. Early interventional pain management has the potential not only to alleviate immediate suffering but also to decrease the likelihood of developing PHN. This dual benefit emphasizes the importance of rethinking current treatment protocols.
For practitioners who are already attuned to interventional techniques, an opportunity exisis to advocate for change. By presenting data supporting the efficacy of ESIs, collaborating on research and engaging in interdisciplinary educational efforts, anesthesiologists can pave the way for a paradigm shift in shingles management.
Recommendations for Changed Practice
- Enhanced interdisciplinary education. Establish educational sessions and seminars to inform primary care providers, dermatologists and infectious disease specialists about the benefits of early ESIs in shingles management.
- Research and data collection. Encourage multicenter trials that examine the long-term outcomes of acute-phase ESIs to provide robust data on pain relief and PHN prevention. Such evidence could be pivotal in altering clinical guidelines.
- Referral protocols. Develop streamlined referral processes that allow for timely consultation with pain specialists when acute shingles cases are identified as particularly severe or refractory to standard treatment.
- Patient advocacy. Educate patients about all available treatment options, including interventional approaches. Informed patients can drive demand for alternative therapies and motivate physicians to consider broader treatment modalities.
Conclusion
Epidural steroid injections represent a promising therapeutic intervention for patients suffering from acute shingles pain. Despite demonstrated efficacy, the lack of referrals for early intervention highlights a significant gap in current clinical practice. By fostering greater awareness, encouraging interdisciplinary collaboration and supporting further research into ESIs, the medical community can better address the acute distress experienced by patients with shingles. Anesthesiologists and pain specialists are uniquely positioned to lead this change, ultimately improving patient care and potentially preventing the chronic suffering associated with progression to PHN.