Measles cases in the United States have now hit 1,197, as of data reported from the CDC on June 13, 2025. Although the majority of cases—more than 700—are centered around the Texas outbreak, there have been confirmed measles cases in 33 states, and nearly all (90%) of the confirmed cases have been related to 21 outbreaks in 2025 (as opposed to cases linked to travel). Three deaths and 144 hospitalizations have been attributed to measles.
However, 95% of confirmed measles cases occurred in unvaccinated individuals or those with unknown vaccination status— meaning there are things that infectious disease and other healthcare providers can do to keep numbers down in your area. A presentation from the American Society for Microbiology outlined best practices and tips when dealing with measles.
Diagnosing Measles
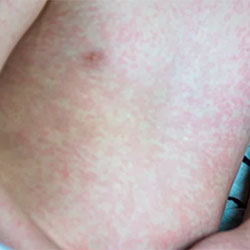
Classic measles symptoms—fever, cough, coryza, conjunctivitis and rash—are also signs of other fever causing viruses. “It’s difficult to sometimes differentiate from other viral presentations,” said speaker Denver Niles, MD, D(ABMM), the associate director of medical microbiology and virology at Texas Children’s Hospital and an assistant professor of pathology and immunology and of pediatrics at Baylor College of Medicine, in Houston. Two characteristics that could help identify measles are biphasic fever and Koplik spots, Dr. Niles explained. Fevers may present twice: at onset of infection, then subsiding and reemerging with the first appearance of the rash. Koplik spots are “unique to measles,” he said, and “consist of small, white, sand grain-like papules or spots in the mouth.”
Dr. Niles explained that other viruses can mimic measles. Although German measles, or rubella, is a classic mimic of measles, “we don’t really see a lot of it,” he said. It also has a rash that starts from the head down, but it instead has lymphadenopathy that is occipital or postauricular. Parvovirus B19, which causes fifth disease, also leads to a rash, but it has a classic slap-cheek appearance and sometimes a lacy rash on the trunk of the body, without cough or conjunctivitis, he said. Unlike measles, roseola, or sixth disease, causes a high fever that subsides, followed by a rash.
On the other hand, adenovirus can be hard to differentiate from measles, Dr. Niles said, because it also comes with fever, conjunctivitis and rash. But adenovirus often causes pharyngoconjunctivitis, and sometimes follicular conjunctivitis, the latter of which is not seen in measles, he said.
Other viruses could be confused with measles. However, an enterovirus rash involves the palms and soles, which don’t occur with measles; dengue often has a retro-orbital headache and thrombocytopenia, and the patient has traveled outside the United States; a rash from Epstein-Barr virus usually follows a treatment of amoxicillin or ampicillin if the patient was previously misdiagnosed. “Finally,” he said, “COVID-19 early on in the pandemic could be confused [with measles] because patients may have fever, conjunctivitis and may occasionally have rash as well.”
It’s important to know the difference, especially as many current doctors have not seen measles in their offices or clinics. “I personally haven’t seen measles,” he said, so “it’s important to know those distinguishing features for measles versus some of these febrile rash illnesses.”
What Test to Use
The options for testing a suspected measles case include real-time polymerase chain reaction (RT-PCR) and serological testing. “Laboratory confirmation is essential for all suspected cases of measles, whether sporadic or outbreak associated,” said speaker Paul Rota, PhD, a former microbiologist in the Division of Viral Diseases at the CDC and an adjunct professor at Emory University, in Atlanta.
RT-PCR testing
For RT-PCR testing, samples can be taken through throat or nasopharyngeal swabs (NPS) or a urine sample. “For throat swabs or NPS, it’s important to collect them as soon as possible after rash onset, but up to 10 days,” Dr. Rota said. “Urine also should be collected as soon as possible.”
Dr. Rota also recommends collecting, storing and shipping samples to maintain specimen integrity, and the RT-PCR assay should detect with a cellular reference gene to check the specimen quality and help interpreting test results.
The CDC’s standard RT-PCR assay detects vaccine and wild-type strains of measles virus, It’s a laboratory-developed test using Singleplex TaqMan (Thermo Fisher Scientific) assays that use the company’s Applied Biosystems 7500 or 7500 fast Dx equipment.
In addition to the CDC, many state, county and commercial labs, as well as the Association of Public Health Laboratories Vaccine Preventable Diseases (APHL-VPD) Reference Centers, perform measles RT-PCR. The CDC and APHL-VPD centers can provide assistance when local labs are validating or onboarding measles testing, Dr. Rota said. Positive control RNA is also available in limited supply through the CDC’s International Reagent Resource, and measles viral isolates are available through the American Type Culture Collection, he said.
The CDC and the APHL-VPD centers also provide a vaccine specific RT-PCR that specially detects vaccine strains. This assay can provide rapid confirmation of suspected vaccine reactions in individuals up to 21 days after vaccination.
The CDC and APHL-VPD centers are also where to send positive RT-PCR samples for genotyping. “The genotyping and sequence analysis is really mostly used for tracking transmission pathways. We think about measles a little bit differently than say you would be thinking about influenza or COVID, where you’re looking for variants that you may need to consider for vaccines,” Dr. Rota explained. “For measles, we’re really using the sequence data to track transmission pathways and to show that virus cases are either in a single chain of transmission or separate chains of transmission.”
If the genotyping is performed at a state, county or commercial lab, the sample also should be sent to the CDC or APHL-VPD, Dr. Rota said.
Serological testing
For serological testing, there is a benefit to immunoglobulin M (IgM) tests if a patient sample can’t be taken until very late after rash onset, Dr. Rota said, since RT-PCR’s detection capability decreases each day after rash onset. However, serum collected within the first three days of rash can produce a false negative, potentially leading to false-positive results, especially in low-incidence settings, Dr. Rota explained.
Of note, the market for commercially supplied IgM test kits has been in flux. “There’s been some variation of kits going on and off the market,” he said, “so it’s been a little bit inconsistent to be able to acquire these kits.” Nonetheless, the CDC, as well as some public health and commercial labs, will perform IgM testing, Dr. Rota said.
Serological testing, specifically IgG, also can be used to determine whether exposed individuals or healthcare workers have preexisting immunity, particularly when documentation of childhood vaccination is unavailable. However, IgG testing only shows one part of a person’s immunity, Dr. Niles noted. “One of the caveats with IgG testing is that you may have lower, undetectable IgG levels with declining levels over time, but patients may still have immunity because there’s some cellular immunity that measles patients who have had measles vaccine may have with memory B cells or T cells,” he said.
When to Turn to Prophylaxis
Measles is the most contagious known virus, with one case infecting nine to 10 other people, according to the CDC. “So you can see how this would spread like wildfire if you had measles in a community where there’s under vaccination,” Dr. Niles said. Herd immunity means that 95% of a community is immune to measles, he explained, and the communities in Texas currently experiencing outbreaks are well below that level. “Post-exposure prophylaxis [PEP] is key,” along with contract tracing, Dr. Niles said.
For PEP, the measles, mumps and rubella (MMR) vaccine is recommended for infants 6 months of age and older as long as there are no contraindications, such as in immunocompromised or certain pregnant people. The vaccine is highly effective if given 72 hours of exposure, Dr. Niles said. For infants younger than 6 months of age and pregnant people, intramuscular immunoglobulin can be administered within six days of exposure.
If an individual has documented immunity (especially with two doses of MMR), then no PEP is needed. However, if a person only has one dose of MMR, a second dose can be given as PEP, Dr. Niles said.
So You Have a Patient With Measles
Given that measles is highly contagious, the first step is to isolate an infected patient. If available, a negative pressure room is ideal, and staff should use airborne precautions, Dr. Niles said.
Next, staff should notify the hospital’s infection control department to alert them of a suspected case of measles, and then notify the local health department to handle contact tracing and PEP distribution.
Other Viruses Circulating
It’s not just measles that is circulating in the United States. Mumps is also circulating in the United States, with 139 cases reported this year, as of May 22; California accounts for 14 of these infections. However, these numbers pale compared with recent U.S. outbreaks that have ebbed and flowed since 2006, when there were 6,584 cases of mumps. Most of these outbreaks have occurred among young adults and vaccinated people. Large outbreaks have happened in settings with frequent close contact, such as college campuses, large gatherings and close-knit communities, according to the CDC.
Pertussis cases also remain elevated. Preliminary data from the CDC show more than six times as many cases in 2024 compared with 2023. a provisional total of 7,343 cases. As of May 31, 2025, there have been a total of 12,527 pertussis cases in the United States, up from last year’s count of 7,343 cases. The CDC recommends continued vaccination as the best way to prevent pertussis, as immunity can wane over time.
Dr. Niles reported a financial relationship with bioMerieux.