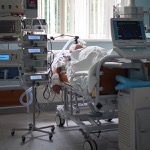
By Myles Starr
According to the CDC, 1 in 3 people who die in an American hospital have an infection that becomes sepsis (bit.ly/CDC_sepsis). This situation has necessitated the development of rapid response teams that quickly diagnose and treat sepsis in an effort to decrease mortality associated with the infection.
“We can safely say there is evidence that sepsis [rapid] response teams [SRRTs] increase guideline adherence and reduce mortality,” explained Frank Bloos, MD, PhD, an ICU physician at Jena University Hospital, in Germany, and first presenter in a panel discussion held at SCCM 2025, in Orlando, Fla.
Dr. Bloos drew these conclusions based on studies that assessed patient outcomes before and after the implementation of SRRTs. For example, a 2024 literature review published in SAGE Open Medicine found that implementation of an SRRT led to a statistically significant reduction in mortality among sepsis patients (2024;12:20503121241290378). Furthermore, a 2020 study published in the American Journal of Emergency Medicine found that the implementation of an SRRT increased guideline-recommended administration of broad-spectrum antibiotics within three hours of presenting sepsis symptoms from 72% to 96% of patients (2020;38[5]:879-882). Despite these encouraging results, Dr. Bloos warned that implementation of SRRTs can require significant amounts of effort and capital; as such, his co-presenters focused on strategies to meet these challenges.
The Role of Leaders
The first crucial keystone in building a successful SRRT is the presence of strong leaders who understand the importance of providing human resources, financial backing and IT support to tackle sepsis infections.
“These individuals will lead a team of doctors, nurses, pharmacists and electronic medical record experts in implementing an active structure and process for identifying sepsis; understanding what management looks like; and standardizing this process across an institution,” explained co-panelist Casey Cable, MD, MSc, FCCP, the director of resource intensivists and an associate professor at Virginia Commonwealth University Health, in Richmond. She noted that leaders must equip their SRRTs with the correct tools, training and technology.
Tools
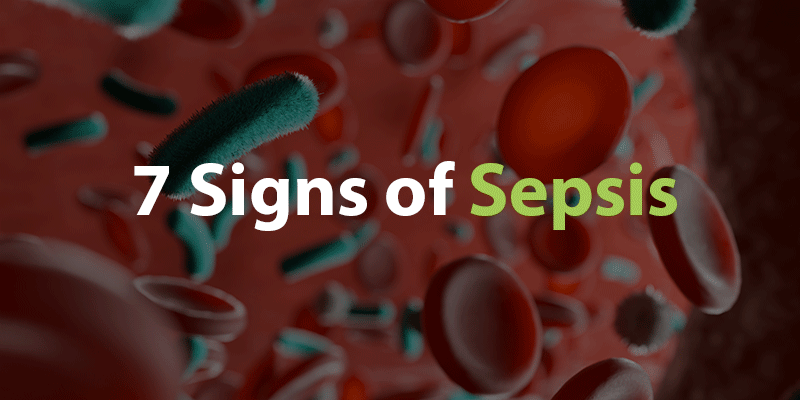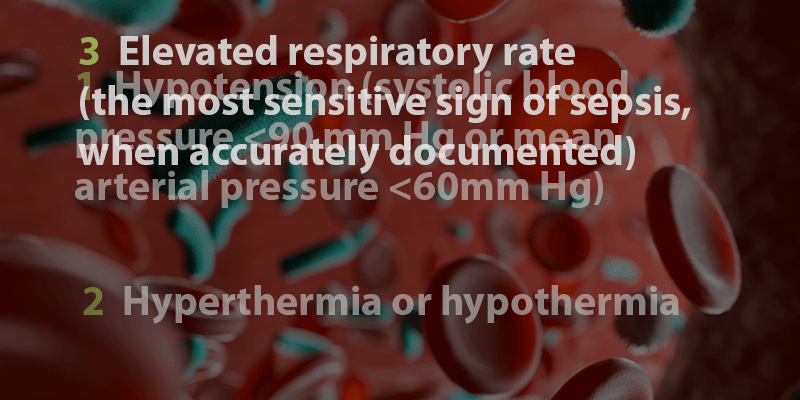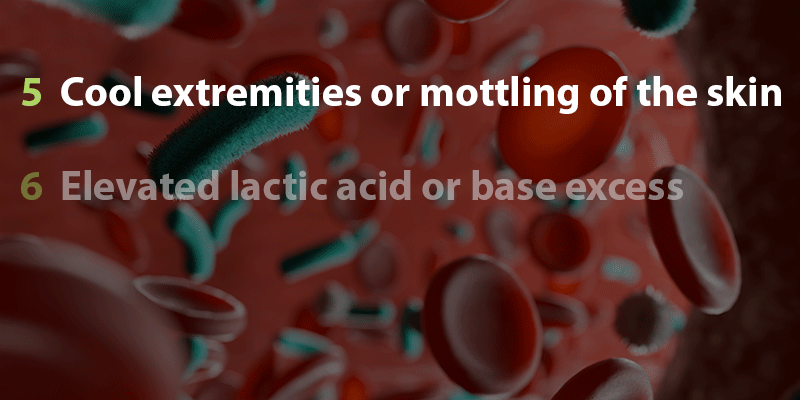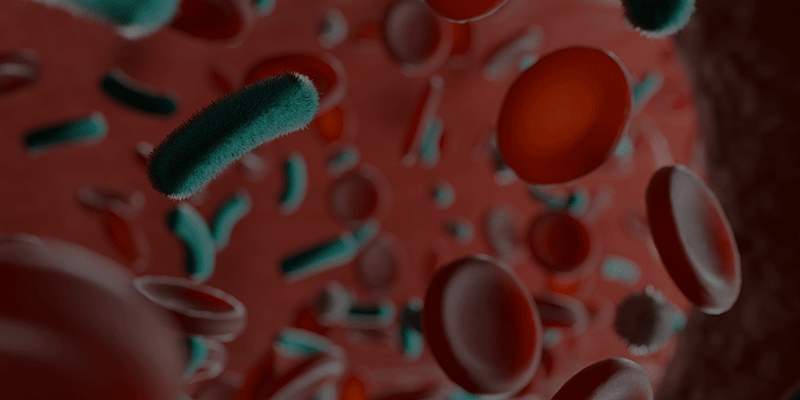
There are several clinical metrics available to SRRTs to determine whether a patient has sepsis, including the SIRS (Systemic Inflammatory Response Syndrome) Criteria, SOFA (Sequential Organ Failure Assessment) Score, and ESM (EPIC Sepsis Model). However, co-presenter Brandy McKelvy, MD, FCCP, an associate professor of medicine at McGovern Medical School with UTHealth Houston, warned that none of these metrics should be solely relied upon by an SRRT to diagnose sepsis. Instead, they should choose the metric that best fits their institution and augment these tools by looking for the following signs of sepsis (see box).
Technology
After an institution has identified the metrics it wants to use to identify sepsis, IT staff need to help build out these tools. When building these tools, several parameters need to be considered: how (and in what time frame) clinical data are captured; how errors are handled; and what interface will be used to communicate alerts. Once these parameters have been decided upon, assessment, standardization and documentation are critical to keeping the system functioning. All this planning is in the service of “good messaging, communication and coordination within a SRRT to understand how the patient looks, what’s happening and if there needs to be any, any sort of escalation,” Dr. Cable explained.
Training and Education
A solid foundation of reliable identification tools and well-implemented technology must be supported with adequate training and education of staff. “Leadership is tasked with ensuring that all staff understands what sepsis is, how to recognize it and be familiar with standards of care,” Dr. Cable said. Key to this effort is initial training, which includes role-playing, lectures and case-based discussions. However, ongoing training including e-learning modules, antibiotic stewardship education and annual competency assessment are also recommended.
When hospital leadership invests in appropriate tool selection, well-integrated technology and training, creating a successful SRRT is possible. However, “the landscape around sepsis is constantly changing,” Dr. Cable concluded. “To make sure that an SRRT stays relevant and effective, giving the highest quality care to patients, hospitals must invest in continuous improvements, performance reviews and metrics analysis.”
Drs. Bloos, Cable and McKelvy reported no relevant financial disclosures.