By Ethan Covey
A case of cutaneous Pneumocystis jirovecii pneumonia (PJP) has been confirmed in a 67-year-old man who underwent an allogeneic stem cell transplant (SCT).

Pneumocystis jirovecii.
Created by CDC/ Lois Norman, MS.
“Despite their rarity, cutaneous Pneumocystis jirovecii infections are a significant area of study, especially in vulnerable populations,” said Nikhil Sood, MD, a hospitalist in the Department of Medicine at Banner Health in Gilbert, Ariz., and lead author of the report. “By adding to the limited literature on extrapulmonary manifestations of the disease, this publication expands our understanding of risk factors and clinical presentations.
“[The publication] underscores the importance of early recognition of unusual manifestations in vulnerable populations, particularly those with weakened immune systems,” Dr. Sood added.
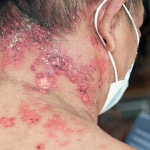
The man had T-cell prolymphocytic leukemia, underwent an allogeneic SCT and had multiple issues after transplant. Six months after transplant, he presented to the ER and was diagnosed with PJP and cytomegalovirus. Six weeks later, he presented with multiple nodular lesions on the forearms, ankles and legs. A diagnosis of CPJ was made, and he received therapeutic doses of trimethoprim-sulfamethoxazole (TMP-SMX).
The patient was treated with TMP-SMX for six weeks and recovered with near resolution of his skin lesions.
While TMP-SMX prophylaxis has significantly reduced PJP infections, for various reasons many patients cannot tolerate it as first-line treatment. In these cases, patients are given pentamidine prophylaxis, which doesn’t prevent extrapulmonary infection.
“This report raises intriguing questions about the mechanisms underlying the development of cutaneous infections, given their rarity, and how they differ in progression from the pulmonary form,” Dr. Sood said. “This could stimulate future research on whether specific patient profiles are more susceptible to these unusual manifestations or if specific treatments predispose individuals to cutaneous pneumocystis infections over respiratory ones.”
Dr. Sood also noted that further investigation into the diagnostic challenges is crucial.
“We did two skin biopsies, which were not definitive, and as explained in the report, the diagnosis was based on expert opinions,” he said. “This is another area of research that needs to be explored to improve the diagnosis of these infections. We wonder how many such infections are missed, not discovered timely, or misdiagnosed.”
Dr. Sood also said work should be done to look into alternatives to TMP-SMX for use in patients who are unable to receive the prophylactic treatment.
“Since TMP-SMX isn’t well tolerated in many patients, we should look for regimens in transplant patients that are better tolerated and carry less risk of extrapulmonary pneumocystis infections other than just inhaled pentamidine,” he said.
Dr. Sood reported no relevant financial disclosures.