By Donald M. Pizzi
Originally published by our sister publication Pain Medicine News
Admitting it underestimated the incidence and extent of severe pain in reported monkeypox cases during the current crisis, the CDC is now advocating aggressive pain treatment at the first signs of monkeypox lesions.
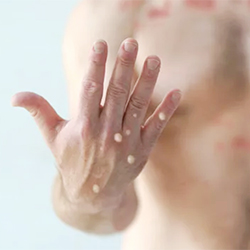
As part of that effort, the CDC is providing guidance to healthcare professionals that is designed to aid in the development of monkeypox treatment programs.
“Early recognition of mucosal or genital lesions may help prevent severe pain and other complications at vulnerable sites—e.g., proctitis causing severe pain in the rectum,” the CDC wrote in a press statement, stressing the need for pain treatment “tailored to the needs and context of an individual patient.”
Perianal and oral mucosal lesions are reported in 40% of U.S. monkeypox cases, and are often associated with severe pain. Penile swelling and genital lesions are other common pain complaints that often require hospitalization (N Engl J Med 2022;387:679-691; BMJ 2022;378:e072410 and MMWR Morb Mortal Wkly Rep 2022;71[32]:1018-1022).
In a letter to healthcare providers and medical societies, CDC Director Rochelle P. Walensky, MD, MPH, asked for documentation related to the pain experience in monkeypox patients, stating it has been “out of proportion to expectation.”
“We have much to learn about the novel clinical presentations of monkeypox in the 2022 outbreak,” Dr. Walensky wrote. “The experiences of healthcare providers on the front lines are critical for building the evidence base to inform optimal approaches to pain management.” Specifically, the CDC is asking for information regarding incidence, predictive factors and successful pain control methods, according to the letter.
In addition, the letter stated that studies are underway to evaluate antiviral medications to treat monkeypox virus (MPV) infection, including related pain.
The guidance stresses that healthcare professionals should assess pain in all patients with MPV infection, “and recognize that substantial pain may exist from mucosal lesions not evident on physical exam; validation of the pain experience can build trust in the care provider and care plan.”
First-line treatment for monkeypox lesion pain includes topical steroids and agents such as lidocaine localized, although caution should be used near open sores or broken skin, according to the World Health Organization
Kevin L. Ard, MD, MPH, the medical director of the National LGBTQIA+ Health Education Center at The Fenway Institute, and the director of the Sexual Health Clinic at Massachusetts General Hospital, in Boston, agreed, telling Pain Medicine News sister publication Infectious Disease Special Edition, “We try to address pain as much as we can and that can be with topical treatments or painkillers,” Dr. Ard said. “Another strategy is to use the antiviral TPOXX [tecovirimat (Siga Technologies)].” Tecovirimat is a core treatment for monkeypox, with anecdotal reports that it shortens lesion healing to about three or four days rather than three or four weeks
To minimize the risk for autoinoculation, persons with MPV infection or their caregivers should use disposable gloves when applying topical medications to lesions. Warm baths of water and baking soda or Epsom salt could be considered for symptomatic relief of rectal pain.
Over-the-counter pain medications, such as acetaminophen and nonsteroidal anti-inflammatory drugs, are recommended for general pain, according to the World Health Organization.
Uncontrolled pain following standard treatment may require the short-term use of gabapentin or opioids, according to the CDC. If opioids are prescribed, “immediate-release opioids at the lowest effective dose should be prescribed for no longer than the expected duration of pain severe enough to require opioids,” according to the agency. Constipation related to opioid use can be prevented or lessened with proper hydration, exercise and fiber intake. Stool softeners and laxatives can be used as needed.
For management of oropharyngeal symptoms, patients can consider rinsing the mouth with clean saltwater or an oral antiseptic (e.g., chlorhexidine mouthwash), local anesthetic (e.g., viscous lidocaine), and prescription analgesic mouthwash can also be considered.
Oral antihistamines may provide some relief of pruritus associated with monkeypox lesions. Topical agents such as calamine lotion, petroleum jelly or colloidal oatmeal also may improve symptoms.
Based on press materials from the CDC and additional reporting from Infectious Disease Special Edition.