By IDSE News Staff
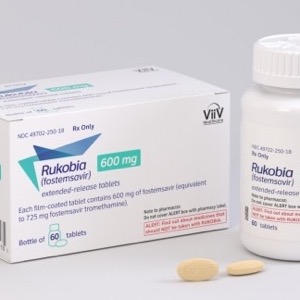
The FDA approved fostemsavir (Rukobia, ViiV Healthcare) to treat adults with multidrug resistance (MDR) HIV, whose viral loads are not reduced despite taking multiple HIV medications.
Fostemsavir, provided as 600 mg extended-release tablets, is a novel attachment inhibitor for the treatment of HIV-1 infection indicated for use with other antiretroviral therapies (ART) in heavily treatment-experienced adults with MDR HIV-1 infection, who are failing their current ART due to resistance, intolerance or safety considerations.
Fostemsavir works by converting to temsavir, which is then absorbed and exerts antiviral activity by attaching directly to the glycoprotein 120 (gp120) subunit on the surface of the virus, which blocks HIV from attaching to host immune system CD4+ T-cells and preventing the virus from infecting those cells and multiplying. Because fostemsavir is the first ART to target this step of the viral cycle, there is no demonstrated resistance to other classes of antiretrovirals, which may help patients who have become resistant to most other medicines.
“The availability of new classes of antiretroviral drugs is critical for heavily treatment-experienced patients living with multidrug resistant HIV infection—helping people living with hard-to-treat HIV who are at greater risk for HIV-related complications, to potentially live longer, healthier lives,” said Jeff Murray, MD, the deputy director of the Division of Antivirals in the FDA’s Center for Drug Evaluation and Research.
Despite the significant advances in ART, the 6% of heavily treatment-experienced adults with MDR HIV have little to no options left due to resistance, tolerability or safety considerations, according to the OPERA cohort studies (22nd International AIDS Conference; July 23–27, 2018; Amsterdam, the Netherlands. Poster THPEB044). Adults with MDR HIV are at risk of progressing to AIDS and death.
The approval was supported by data from the phase 3 BRIGHTE study, which evaluated the safety and efficacy of fostemsavir with optimized background therapy (OBT) in heavily treated adults living with MDR HIV. Most participants had been treated for HIV for more than 15 years (71%), had been exposed to five or more different HIV treatment regimens before entering the trial (85%) and/or had a history of AIDS (86%), according to the FDA.
The BRIGHTE trial is an international, partially randomized, double-blind, placebo-controlled study conducted in 371 heavily treatment experienced (HTE) adults living with MDR HIV. All trial participants were required to have a viral load at least 400 copies/mL and have two or fewer classes of antiretroviral medications remaining at baseline due to resistance, intolerability, contraindication or other safety considerations. Trial participants were enrolled in either a randomized or nonrandomized cohort defined as follows:
- The 272 participants in the randomized cohort had one, but no more than two, fully active and available antiretroviral agents at screening, which could be combined as part of an efficacious background regimen. Randomized participants received either blinded fostemsavir 600 mg twice daily (n = 203) or placebo (n = 69) plus their current failing regimen for eight days of functional monotherapy. Beyond Day 8, randomized participants received open-label fostemsavir 600 mg twice daily plus an investigator-selected OBT.
- The 99 participants in the nonrandomized had no fully active and approved ART available at screening. Nonrandomized participants were treated with open-label fostemsavir 600 mg twice daily plus OBT from Day one onward. The use of an investigational drug as a component of the OBT was permitted in the nonrandomized cohort.
The primary endpoint analysis, based on the adjusted mean decline in HIV-1 RNA from Day 1 at Day 8 in the randomized cohort, demonstrated superiority of fostemsavir to placebo (0.79 vs. 0.17 log10 copies/mL decline, respectively; P<0.0001, Intent-to-Treat-Exposed [ITT-E] population). In the randomized cohort, HIV-1 RNA <40 copies/mL was achieved in 53% and 60% of subjects at Weeks 24 and 96, respectively (ITT-E, Snapshot algorithm). Mean changes in CD4+ cell count from baseline continued to increase over time (i.e., 90 cells/mm3 at Week 24 and 205 cells/mm3 at Week 96).
In the randomized cohort, 60% (n=163/272) of individuals who received fostemsavir in addition to an investigator-selected OBT achieved undetectable HIV viral load and clinically meaningful improvements to CD4+ T-cell count through Week 96.
“The data were very promising in that the viral load stayed nondetectable in a large number of patients out to week 48,” said Michael Kozal, MD, a professor of medicine at the Yale School of Medicine, in New Haven, Conn., and the chief of staff for the VA Connecticut Healthcare System. “There’s no cross-resistance to other classes, so we think it’s going to be helpful for people who have exhausted other drug classes or can’t take other drug classes because [of intolerance],” Dr. Kozal told Infectious Disease Special Edition in an earlier interview.
The proportion of participants who discontinued treatment with fostemsavir due to an adverse event was 7% at Week 96 (randomized: 5% and nonrandomized: 12%).
The most common adverse reaction (all grades) observed in about 5% of participants were nausea. The proportion of participants who discontinued treatment with fostemsavir due to an adverse event was 7% at Week 96 (randomized: 5% and nonrandomized: 12%).
In the nonrandomized cohort, HIV-1 RNA <40 copies/mL was achieved in 37% of subjects at Weeks 24 and 96. At these times, the proportion of subjects with HIV-1 RNA <200 copies/mL was 42% and 39%, respectively (ITT-E, Snapshot algorithm). Mean changes in CD4+ cell count from baseline increased over time: 41 cells/mm3 at Week 24 and 119 cells/mm3 at Week 96. The most common adverse reactions reported in nonrandomized subjects were fatigue, nausea and diarrhea. Click here for the package insert.
The most common adverse reaction to fostemsavir was nausea. Severe adverse reactions included elevations in liver enzymes among participants also infected with hepatitis B or C virus, and changes in the immune system (immune reconstitution syndrome), according to the FDA.
Fostemsavir was granted Fast Track and Breakthrough Therapy Designations.