By IDSE News Staff
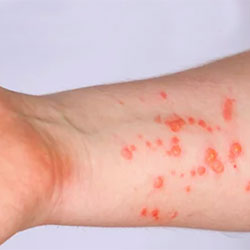
A California man who traveled to the United Kingdom was diagnosed with monkeypox virus (MPV) after presenting with vesicular and pustular skin lesions, according to a report from Stanford University School of Medicine (Emerg Infect Dis 2022;28[10]. doi:10.3201/eid2810.221191).
Most cases in the current multicountry outbreak of MPV have been linked to intimate contact among men who have sex with men (MSM), and while the man in the Stanford case identifies as bisexual, the man reported no sexual contact during the three months prior to presentation. He did not have anogenital involvement, and reported no preceding fevers, chills, headache, lymph node swelling, cough or fatigue. He had a history of syphilis treated three months prior to presentation and was taking preexposure prophylaxis for HIV.

The 20-year-old man presented to the emergency department on day 7 of an asynchronous, diffuse vesicular rash. The first lesion appeared about 14 days after he spent several hours at a large, crowded outdoor event. The event was not an LBGTQ+ event.
He reported close contact with people, including dancing, and that many attendees were dressed for the hot weather, wearing sleeveless shirts and shorts. He told the physicians that he did not notice any sick guests or lesions/sores on anyone.
He also reported sharing an e-cigarette with a woman he met at the party. He said he drank alcohol, but did not do drugs at the event, nor did he wear a mask. He also reported contact with several pet dogs.
He reported no close indoor activities, but he traveled on crowded trains.
He had a connection on the return home. Masks were worn on one flight, but not the other.
He said his roommate does not have any symptoms.
The physicians described multiple nondraining skin lesions at various stages of appearance, “including a centrally umbilicated vesicle on his left palm, a crusting flat lesion on his lip, and pustules on his right and left knuckles and on his lateral torso and back. He had no penile, testicular, or anal lesions and no cervical, axillary, or inguinal lymphadenopathy.”
His tests for SARS-CoV-2, HIV, gonorrhea and chlamydia were negative, but he tested positive for MPV. The physicians did not prescribe specific treatment for MPV because “the patient did not have complications or risk factors for severe disease.
“We performed follow-up [MPV] testing with patient consent 3 days after initial evaluation (day 10 after symptom onset) to clarify viral shedding. We detected virus DNA in a saliva sample, as well as from patient-collected conjunctival and rectal swabs using both the non-variola orthopoxvirus and clade 2/3 [MPV] qPCRs [quantitative polymerase chain reaction tests]. Lesions resolved by day 26 after symptom onset,” the physicians wrote.
In addition, the patient tested positive for MPV from several samples that were taken that did not have lesions. The physicians called the nasopharyngeal and saliva findings noteworthy because the patient did not report respiratory symptoms. “In addition, the detectable viral DNA in the rectal swab specimen in the absence of visible anal lesions or pain indicates a potential for sustained sexual transmission, although the viral DNA levels were low; contamination during self-collection cannot be ruled out. We were unable to assess whether internal rectal lesions were present,” they wrote.
“The lack of both sexual exposure and anogenital involvement indicates that mode of transmission may be associated with clinical symptoms; fomites (hotel bedding and sheets, high-touch areas in public settings) may be alternative modes of transmission,” they wrote.