By Marie Rosenthal, MS
Updated on May 23 at 4:30 p.m.
So far, only one case of monkeypox has been confirmed in the United States, but there are four cases of confirmed orthopoxvirus. Since monkeypox is an orthopoxvirus, the agency expects them to be monkeypox, too, according to Jennifer McQueston, DVM, MS, the deputy director, Division of High Consequence pathogens and Pathology, at the CDC.
"I want to emphasize that we are in the early days of this response, and it is likely that there are going to be additional cases reported in the United States," Dr. McQueston said a briefing on May 23.
She added that so far the strain being seen in the United States and globally is the West African strain, "which is the milder of the two strains of monkey orthopoxvirus. Most people who are infected with monkeypox recover within two to four weeks without specific treatments."
In addition, Dr. McQueston said, the United States does have two vaccines, which are part of the national stockpile that could be used in at-risk populations.
In addition to U.S. cases, the CDC is tracking multiple clusters of monkeypox that have been reported within the past two weeks in several countries that do not normally report monkeypox, including Portugal, Spain and the United Kingdom.
Monkeypox reemerged in Nigeria in 2017, after more than 40 years with no reported cases. Since then, there have been more than 450 reported cases in Nigeria, according to the World Health Organization.
The virus is endemic in some animal populations in a number of countries, leading to occasional outbreaks among local people and travelers. The recent outbreaks reported across 11 countries, so far, are atypical because they are occurring in non-endemic countries, the WHO said.
So far, there have been about 80 confirmed cases, and 50 pending investigations, according to the WHO, which like the CDC, expects more cases to be reported as surveillance expands.
The CDC said it was not clear how people in these clusters were exposed to monkeypox, but cases include people who self-identify as men who have sex with men (MSM).
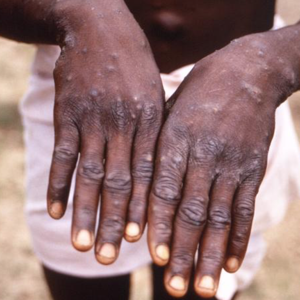
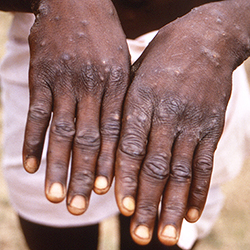
The CDC urged U.S. healthcare providers to be alert for patients who have rash illnesses consistent with monkeypox, regardless of whether they have travel or specific risk factors for monkeypox.
Anyone, regardless of sexual orientation, can spread monkeypox through contact with body fluids, monkeypox sores or shared items (e.g., clothing and bedding) that have been contaminated with fluids or sores of a person with monkeypox. Monkeypox virus can also spread between people through respiratory droplets typically in a close setting, such as the same household or a healthcare setting. Common household disinfectants can kill the monkeypox virus.
“Many of these global reports of monkeypox cases are occurring within sexual networks. However, healthcare providers should be alert to any rash that has features typical of monkeypox. We’re asking the public to contact their healthcare provider if they have a new rash and are concerned about monkeypox,” said Inger Damon, MD, PhD, a poxvirus expert with more than 20 years’ experience and the director of the CDC’s Division of High-Consequence Pathogens and Pathology, where the agency’s poxvirus research is based.
If healthcare providers identify patients with a rash that resembles monkeypox, consider monkeypox, regardless of whether the patient has a travel history to Central or West Africa, the CDC said.
Although many cases do seem to be appearing among MSM, do not limit concerns to MSM, said John Brooks, MD, a medical epidemiologists with the CDC's Division of HIV/AIDS Prevention. "Anyone can develop and spread monkeypox infection," Dr. Brooks said, "but as Dr. mcQuiston also noted many of those affected in the current, global outbreak identify as gay and bisexual men."
Those who have any sort of close personal contact with people with monkeypox could potentially also be at risk for the disease, the CDC said.
Some patients with genital lesions and the rash may be hard to distinguish from syphilis, herpes simplex virus infection, chancroid, varicella-zoster and other more common infections, the CDC warned.
Isolate any patients suspected of having monkeypox in a negative pressure room, and ensure staff understand the importance of wearing appropriate personal protective equipment and that they wear it each time they are near suspected cases.
Consult the state health department or CDC’s monkeypox call center through the CDC Emergency Operations Center (770-488-7100) as soon as monkeypox is suspected.